In my OPD in Hardoi, “chakkar” is one of the top three complaints I hear every day. But vertigo is not a diagnosis — it’s a symptom. And the three conditions that cause it most often look almost identical to patients, yet each needs completely different treatment. Chakkar Vertigo Bppv Vs is a key topic discussed here.
BPPV, vestibular neuritis, and posterior circulation stroke. Get the diagnosis wrong and you’re treating the wrong thing — sometimes dangerously so.
This is how I tell them apart in my clinic, and what you should know before seeing any doctor about your dizziness.
Chakkar Vertigo Bppv Vs: Quick Summary
In my practice in Hardoi, I see these cases regularly. Based on my clinical experience with hundreds of patients, here’s what actually works.
BPPV (Benign Paroxysmal Positional Vertigo): Seconds-long spinning triggered by specific head movements, caused by loose crystals in the inner ear. Treatable with Epley Maneuver (success rate 80-90%). For complex cases, I use the Bangalore Maneuver — a technique I developed specifically for this.
Vestibular Neuritis: Viral inflammation of the balance nerve causing persistent dizziness lasting hours to days. Self-limiting; recovery occurs with central compensation.
Posterior Circulation Stroke: Dangerous condition mimicking vestibular neuritis but identified by failing the HINTS exam (Head Impulse, Nystagmus, Test of Skew). Requires immediate emergency intervention.
Table of Contents
ENGLISH VERSION
Stop Calling Everything “Chakkar”: How to Tell Apart 3 Serious Conditions That Mimic Each Other
The Problem with the Word “Chakkar”
When a patient walks into a clinic and says, “Doctor, mujhe chakkar aata hai,” it can mean almost anything. Chakkar—the Hindi/Urdu word for dizziness—describes a spectrum of sensations: violent spinning, feeling faint, confusion, unsteadiness, or even a vague sense of imbalance. This linguistic ambiguity is a major diagnostic hurdle in emergency medicine and primary care.
A patient saying “I have chakkar” is like a car owner telling a mechanic, “My car is making a noise.” The mechanic cannot fix the problem without knowing: Is it a squealing sound (belt issue)? A grinding sound (brake problem)? A knocking sound (engine trouble)? Similarly, your doctor cannot diagnose your vertigo correctly without understanding what exactly you feel, how long it lasts, and what triggers it.
In clinical practice, what a patient means by “dizziness” is often far less reliable for diagnosis than identifying the specific triggers and duration of the sensation. This is why precise symptom description can be the difference between receiving the correct treatment and enduring years of unnecessary medications or brain scans.
To make sure you receive the correct diagnosis and treatment, it is important to distinguish between three conditions that are frequently confused: Benign Paroxysmal Positional Vertigo (BPPV), Vestibular Neuritis, and Stroke. All three cause spinning sensations; all three are triggered by the balance system; but all three require completely different management approaches.
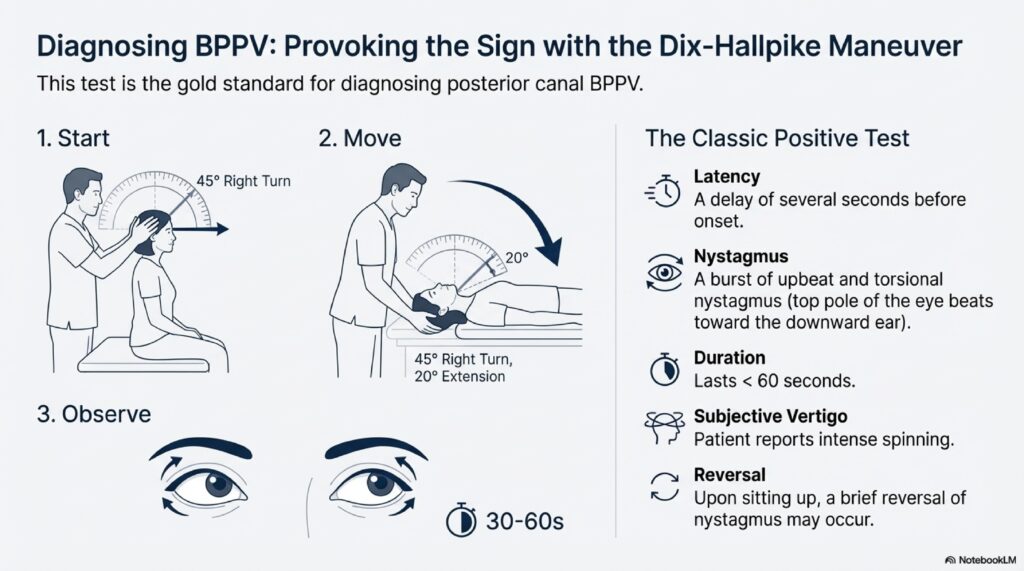
Condition 1: BPPV – The “Mechanical” Spin (Seconds)
What Is BPPV?
Benign Paroxysmal Positional Vertigo (BPPV) is teh most common cause of peripheral vertigo, accounting for approximately 20–25% of all consultations in specialized balance clinics. Importantly, it is not a disease in the traditional sense but rather a mechanical disorder of the inner ear.
The Crystal Culprit
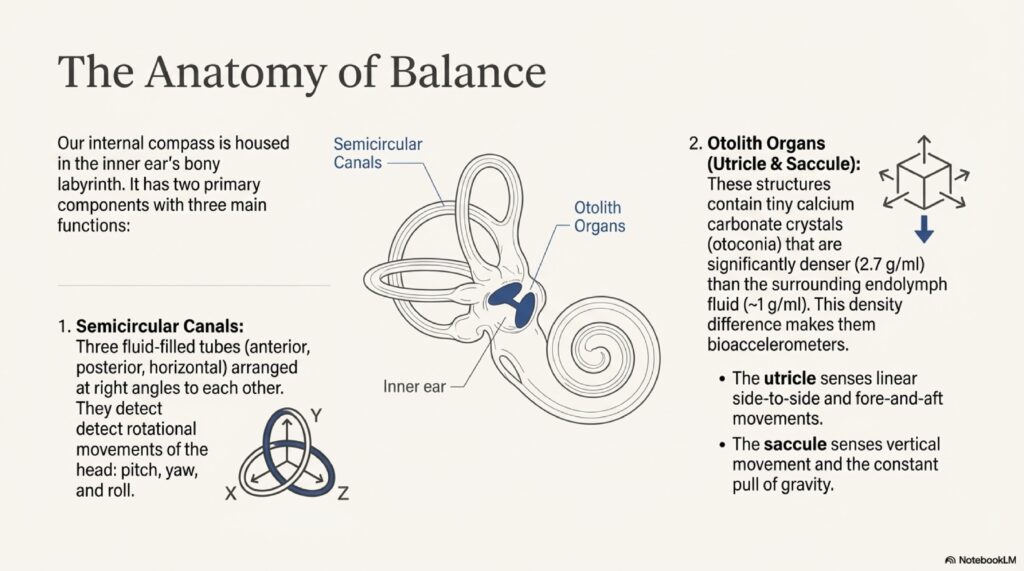
Inside your inner ear, there are specialized sensory organs called the utricle and saccule (part of the otolith organs). These organs contain tiny calcium carbonate crystals called otoconia—imagine them as microscopic “stones” that detect gravity and linear motion.
In BPPV, these crystals become dislodged from their normal position and migrate into one of the three semicircular canals (the tubes that detect head rotation). When you move your head, these “stones” move under the force of gravity, creating an inappropriate flow of fluid through the canal. This false signal tricks your brain into believing you are spinning—even though you are perfectly still.
Key Characteristics: The “5-Second Spinner”
Duration: 5–30 seconds (rarely exceeding 1 minute)
- The spinning is brief and self-limiting
- Episodes resolve quickly once the head is held still
- This short duration is the hallmark feature that distinguishes BPPV from other vertigo types
Triggers: Specific Head Movements
- Turning over in bed (especially rolling to one side)
- Lying down quickly
- Tilting the head back to look up at a ceiling or high shelf
- Bending forward and then straightening up
- Certain yoga or exercise positions
The “Morning Effect”
- Attacks are often most severe in the morning
- During sleep, the crystals may agglomerate (clump together), creating a larger mass that has a higher impact on balance sensors when you first move
- This is why BPPV patients often report, “Every morning, when I roll over, the room spins for 20 seconds”
Associated Symptoms:
- Nausea is common but usually mild because the episode is so brief
- No hearing loss
- No ear pain
- No neurological deficits (no weakness, slurred speech, or double vision)
Why BPPV Matters: The “Curable” Condition
BPPV is the only vertigo condition that can be can provide long-term relief for through a simple physical maneuver.
Epley Maneuver (Canalith Repositioning Procedure):
- A series of slow, controlled head movements that use gravity to guide the crystals out of the semicircular canal and back into the utricle where they belong
- Success rate: 70–90% after a single session
- Takes approximately 10–15 minutes to perform
Semont Maneuver:
- An alternative repositioning maneuver with similar efficacy
Why This Matters for Your Health:
Because BPPV is so common, it is frequently misdiagnosed as general weakness, low blood pressure, or even a vascular issue. Patients then undergo:
- Unnecessary brain MRI scans (costing money and time)
- Unnecessary medications (anti-dizziness drugs that may cause drowsiness)
- Years of missed opportunities for curative treatment
If you have brief, position-triggered vertigo lasting seconds, ask your ENT or neurologist specifically about the Dix-Hallpike maneuver (a diagnostic test) and the Epley maneuver (the cure). This single intervention can end your suffering.
Condition 2: Vestibular Neuritis – The “Prolonged” Spin (Days to Weeks)
What Is Vestibular Neuritis?
Vestibular Neuritis (also called acute unilateral vestibulopathy) is the second most frequent cause of peripheral vertigo. Unlike BPPV, which comes in brief attacks, this condition involves a sudden and sustained failure of the balance nerve on one side.
The Viral Culprit
Vestibular neuritis is believed to be caused by a viral or post-viral infection of the vestibular nerve. It often follows a cold, flu, or other respiratory infection by a few days to a week. The virus causes inflammation and swelling of the vestibular nerve (CN VIII), disrupting its ability to send balanced signals to the brain.
When one side of the vestibular system suddenly fails, the intact side sends unopposed signals to the brain. The brain interprets this asymmetry as if the head is spinning continuously—similar to what would happen if you spun around rapidly for 30 seconds and then stopped abruptly. The sensation of spinning persists until the brain adapts (compensation) and the inflammation resolves.
Key Characteristics: The “Multi-Day Spinner”
Duration: Hours to Days (sometimes weeks)
- The vertigo is violent and continuous, not brief
- It reaches peak intensity within 6–24 hours of onset
- It gradually improves over 2–4 weeks, with most recovery within the first 2 weeks
- Some patients report residual imbalance or motion sensitivity for months
Movement Sensitivity:
- While the spinning is constant, it is severely exacerbated by any head movement
- Patients typically lie as still as possible to minimize symptoms
- This is in stark contrast to BPPV, where symptoms depend on specific movements
Associated Symptoms:
- Nausea and vomiting (often severe due to prolonged nature)
- No hearing loss (this is important for diagnosis)
- No ear pain
- No facial weakness, slurred speech, or double vision (distinguishes it from stroke)
Physical Examination Findings:
- Abnormal head impulse test (HIT): The eyes move away from the target as the head turns, and a catch-up saccade is required to refixate—this indicates vestibular nerve damage
- Unidirectional nystagmus: Involuntary eye movements that beat in a consistent direction
- Mild skew deviation may be present but typically not severe
Why Vestibular Neuritis Matters: The “Movement Is Medicine” Paradox
The treatment approach for vestibular neuritis seems counterintuitive:
Acute Phase (First 1–2 weeks):
- Short course of corticosteroids (e.g., prednisolone) to reduce nerve inflammation and improve recovery
- Anti-emetics (anti-nausea medications like anti-nausea medication) to control severe vomiting
- Rest and reassurance
Recovery Phase (After 1–2 weeks):
- Gradual mobilization and movement is encouraged
- vestibular rehabilitation exercises help the brain “relearn” balance despite the damaged nerve
- Long-term vestibular suppressants (like a vestibular suppressant) should be avoided because they actually slow the brain’s ability to compensate for the nerve damage
Why This Matters:
Many patients with vestibular neuritis are told to rest for weeks or are prescribed long-term anti-dizziness medications. This approach delays recovery. The brain’s natural ability to compensate (vestibular compensation) is activated by movement and challenge. Early mobilization, even when uncomfortable, promotes faster recovery.
If you are diagnosed with vestibular neuritis, ask your doctor about:
- A referral to vestibular rehabilitation therapy (physical therapy specifically for balance disorders)
- The timeline for gradual return to activity
- Whether long-term medication use is appropriate for your situation
Condition 3: Posterior Circulation Stroke – The “Dangerous” Mimic (Sudden, Persistent)
The Stroke That Looks Like Vestibular Neuritis
Between 4% and 15% of patients who arrive at an emergency department with continuous vertigo are actually having a stroke in the brainstem or cerebellum. This is the most dangerous “chakkar” because it can present with symptoms nearly identical to vestibular neuritis.
What Happens in a Stroke
A stroke occurs when blood flow to a region of the brain is interrupted. The balance centers of the brain are located in the brainstem (especially the medulla and pons) and the cerebellum. These regions are supplied by the vertebral and basilar arteries (the “posterior circulation”).
When a blood clot blocks one of these arteries, the affected region of the brain becomes starved of oxygen (ischemia). Because the brainstem is densely packed with critical pathways—each controlling different functions (balance, eye movement, swallowing, speech, motor control)—even a small stroke can cause isolated vertigo that mimics an inner ear infection.
Key Characteristics: Red Flags of Dangerous “Chakkar”
Duration: Sudden Onset, Persistent
- Vertigo appears suddenly, often without warning
- It is continuous and does not resolve with rest or movement
- Unlike vestibular neuritis, it does not follow a predictable improvement curve
Associated Symptoms (The “Red Flags”):
- Double vision (diplopia)
- Slurred speech (dysarthria)
- Difficulty swallowing (dysphagia)
- Weakness or numbness in limbs (especially asymmetric)
- Severe imbalance where the patient cannot sit or stand unassisted (truncal ataxia)
- Facial drooping
- Loss of consciousness or altered mental status
Sudden Hearing Loss + Vertigo = DANGER:
- If severe vertigo is accompanied by sudden hearing loss in one ear, it may indicate an infarction of the Anterior Inferior Cerebellar Artery (AICA) territory
- This artery supplies both the inner ear (cochlea) and the brainstem
- This combination is a classic presentation of brainstem stroke and demands immediate neuroimaging
Why the HINTS Exam Matters: Detecting Stroke in 60 Seconds
The HINTS protocol (Head Impulse, Nystagmus, Test of Skew) is a three-step bedside examination that is more accurate than early MRI at detecting brainstem strokes in the first 48 hours. Understanding what doctors are looking for helps you advocate for proper evaluation.
Step 1: Head Impulse Test (HIT)
What the Doctor Does:
- You fixate on a target (usually the examiner’s nose or a mark on the wall)
- The examiner rapidly rotates your head 10–20 degrees to one side
- The examiner watches your eyes to see if they remain fixed on the target or require a catch-up movement
BPPV or Vestibular Neuritis Finding (Inner Ear Problem):
- Your eyes move away from the target as your head turns
- Your eyes require a quick catch-up saccade to return to the target
- This is an abnormal but reassuring finding because it indicates the inner ear or nerve is damaged, not the brain
Stroke Finding (Brainstem Problem):
- Your eyes remain fixed on the target despite the head movement
- No catch-up saccade is needed
- This is a major red flag because it means your inner ear is intact (normal reflex), but your brain’s integration is damaged
Critical Clinical Pearl: A normal HIT + continuous vertigo = high suspicion for stroke.
Step 2: Nystagmus Pattern
What the Doctor Does:
- The examiner observes your eyes as you gaze straight ahead, then to the right, then to the left
- The examiner specifically looks at the pattern of involuntary eye movements (nystagmus)
BPPV or Vestibular Neuritis Finding (Inner Ear Problem):
- Nystagmus is unidirectional—it always beats in the same direction regardless of where you look
- For example, if your right vestibular nerve is damaged, nystagmus may always beat to the left (away from the damaged side)
Stroke Finding (Brainstem Problem):
- Nystagmus is direction-changing—it beats to the right when you look right and to the left when you look left
- Or, nystagmus is purely vertical or rotatory (twisted), which is almost never seen in peripheral vertigo
- Vertical nystagmus is virtually pathognomonic (uniquely characteristic) of brainstem or cerebellar stroke
Step 3: Test of Skew (Vertical Eye Alignment)
What the Doctor Does:
- You fixate on a target while looking straight ahead
- The examiner covers one eye at a time, observing for vertical misalignment
- If one eye is higher than the other, the uncovered eye will jump up or down when the cover is removed to refixate
BPPV or Vestibular Neuritis Finding (Inner Ear Problem):
- Your eyes remain vertically aligned
- No corrective eye movements are necessary
Stroke Finding (Brainstem Problem):
- One eye is positioned higher than the other (skew deviation)
- When the cover is removed, the misaligned eye jumps to refixate
- Skew deviation is highly specific for brainstem lesions and strongly suggests stroke
Why Stroke Matters: The Critical Treatment Window
A patient presenting with what looks like vestibular neuritis but who actually has a brainstem stroke faces potentially catastrophic consequences:
- Cerebellar swelling can lead to increased intracranial pressure, coma, or death
- Brainstem infarction can impair important functions like breathing and heart rate regulation
- Early intervention with thrombolysis (clot-busting drugs) or thrombectomy (mechanical clot removal) can prevent permanent disability or death
The window for thrombolysis is 4.5 hours from symptom onset. The window for thrombectomy can extend to 24 hours in some cases. Missing the diagnosis wastes these critical windows.
Comparison Table: BPPV vs. Vestibular Neuritis vs. Stroke
| Feature | BPPV | Vestibular Neuritis | Posterior Circulation Stroke |
|---|---|---|---|
| Duration | Seconds (< 1 min) | Days to Weeks | Persistent/Sudden |
| Triggers | Specific head movements | Spontaneous (always present) | Spontaneous |
| Character | Brief, self-limiting | Violent, continuous | Severe, variable |
| Hearing Loss | None | None | Possible (AICA territory) |
| Slurred Speech/Double Vision | None | None | Often present |
| Balance Ability | Mild imbalance | Veering to one side | Profound ataxia (cannot sit) |
| Head Impulse Test | Abnormal (catch-up saccade) | Abnormal (catch-up saccade) | Normal (no catch-up) |
| Nystagmus Pattern | Unidirectional | Unidirectional | Direction-changing or vertical |
| Skew Deviation | Absent or mild | Absent or mild | Often present |
| Treatment | Epley/Semont maneuver | Corticosteroids, vestibular rehab | Thrombolysis/Thrombectomy |
| Prognosis | Excellent (curable) | Good (recovery in weeks) | Variable (depends on severity) |
Why “Chakkar” Isn’t Enough: The Blunderbuss Diagnosis Problem
If you simply tell your doctor, “Doctor, mujhe chakkar aata hai,” you risk receiving a “blunderbuss” investigation—a generic series of tests that may miss the specific cause and waste time and money.
Examples of Misdiagnosis:
Orthostatic Hypotension Misdiagnosed as BPPV:
- A patient reports dizziness only when standing up (orthostatic hypotension due to blood pressure drops)
- The doctor prescribes BPPV treatment, which is ineffective
- Correct diagnosis requires measuring blood pressure lying and standing, and adjusting medications or sodium intake
vestibular migraine Misdiagnosed as Menière’s Disease:
- A patient has episodes of vertigo lasting 4–6 hours with nausea
- Menière’s disease is suspected and salt restriction is recommended
- In reality, the patient has vestibular migraine, which requires lifestyle changes, migraine-specific medications (e.g., triptans), and migraine prevention
- Salt restriction is ineffective
Anxiety-Induced Dizziness Treated as Stroke:
- A patient with generalized anxiety disorder reports feeling faint and dizzy
- Extensive brain imaging is performed unnecessarily
- Cognitive behavioral therapy and anxiety management are the appropriate treatments
Your Tool: The Vertigo Diary—Track to Diagnose
To help your doctor make the correct diagnosis, start a Vertigo Diary immediately after an episode. Document the following details:
Vertigo Diary Checklist (Printable/Digital Format)
Episode #: _ | Date: ___ | Time: _
1. What Did You Feel?
- ☐ Spinning sensation (everything rotating)
- Swaying or tilting sensation
- Lightheadedness or faintness
- Unsteadiness or imbalance
- Other: ___
2. How Long Did It Last?
- Seconds (< 1 minute)
- Minutes (1–5 minutes)
- 5–30 minutes
- 30 minutes to 1 hour
- Hours
- Days or longer
3. What Triggered It?
- Specific head movement (rolling in bed, looking up, etc.)
- Standing up from sitting/lying down
- Sudden head turn
- No clear trigger (spontaneous)
- Stress or anxiety
- Other: ___
4. Associated Symptoms (Check All That Apply):
- Nausea
- Vomiting
- Ear pain
- Hearing loss or ringing in ears (tinnitus)
- Double vision
- Slurred speech
- Difficulty swallowing
- Weakness in limbs
- Facial drooping
- Headache (where? __)
- Severe imbalance (cannot sit/stand alone)
5. Recovery:
- Immediate (as soon as movement stopped)
- Within 10–15 minutes
- Within 1 hour
- Within several hours
- Gradual improvement over days/weeks
6. What Made It Better/Worse?
- Made Better: ___
- Made Worse: ___
7. Your Position When It Started:
- In bed
- Sitting
- Standing
- During activity/exercise
- At rest
Additional Notes:
(Any other details that seemed relevant: recent illness, medications, stress, etc.)
Why the Vertigo Diary Matters
When you bring this diary to your appointment at PRIME ENT Center Hardoi, it provides your doctor with:
- Objective data (not just memory)
- Pattern recognition (if episodes cluster or follow a trigger)
- Red flag identification (if you’ve documented neurological symptoms)
- Accurate severity assessment (duration and associated symptoms guide treatment urgency)
Submit the diary to your clinic before your appointment if possible, so the doctor has time to review it and come prepared with specific diagnostic tests.
When to Go to the Emergency Department vs. But Urgent Clinic
GO TO THE EMERGENCY DEPARTMENT IMMEDIATELY IF:
- First-ever episode of continuous vertigo lasting > 1 hour
- Vertigo + double vision, slurred speech, difficulty swallowing, or weakness
- Severe imbalance (cannot sit or stand without assistance)
- Vertigo + severe headache, especially at the back of the head
- Vertigo + sudden hearing loss
- Progressive worsening over hours
- Loss of consciousness or confusion
SCHEDULE AN URGENT APPOINTMENT AT PRIME ENT CENTER HARDOI (24–48 HOURS) IF:
- Brief, position-triggered vertigo lasting seconds (likely BPPV)
- Stable, gradual-onset vertigo with normal neurological examination
- Recurrent episodes of known vertigo type
- Vertigo with ear discharge or hearing loss (but stable condition)
- Pediatric vertigo with normal examination
Key Takeaways: Stop the Misdiagnosis
- “Chakkar” is too vague. Describe your spinning sensation, its duration, and its triggers.
- Brief vertigo (seconds) triggered by head position = BPPV. Seek the Epley maneuver—it cures you.
- Continuous vertigo (days) without other symptoms = Vestibular NeuritisCommon Symptoms of Vertigo. Expect corticosteroids and vestibular rehabilitation.
- Vertigo with neurological symptoms (double vision, slurred speech, weakness) = Possible Stroke. Go to the emergency department immediately.
- Use a Vertigo Diary to track patterns and provide your doctor with accurate diagnostic information.
- The HINTS exam (head impulse, nystagmus, skew deviation) can identify stroke at the bedside in 60 seconds, faster than MRI.
Contact PRIME ENT Center Hardoi
For Urgent Diagnosis and Management:
- Address: PRIME ENT Center, Hardoi (241001)
- Specialists: Dr. Prateek Porwal, ENT & Vertigo Specialist | Prime ENT Center, Hardoi, Dr. Harshita Singh
When calling, mention:
- Your vertigo diary observations
- Duration and triggers of your symptoms
- Any red flag symptoms (double vision, slurred speech, hearing loss)
Getting dizzy spells? Don’t wait.
If you’re unsure whether your chakkar is BPPV, vestibular neuritis, or something more serious — a proper examination makes all the difference. I see patients from across India for this.
Call or WhatsApp: 7393062200
Online consultations available pan-India.
In-person: Prime ENT Center, Nagheta Road, Hardoi, UP 241001.
FAQs
>
Frequently Asked Questions
1. What is the main difference between BPPV and vestibular neuritis?
Answer: BPPV causes brief spinning (seconds to a minute) triggered by specific head movements, usually resolving quickly. Vestibular neuritis causes prolonged, continuous spinning (days to weeks) that comes on suddenly without positional triggers. BPPV is cured by the Epley maneuver; vestibular neuritis resolves with steroids, anti-nausea medications, and vestibular rehabilitation. Duration is the key differentiator.
2. Why is my doctor checking my eyes during a vertigo assessment?
Answer: Eye movements reveal where the problem is located. In the HINTS exam, doctors observe the head impulse test (whether eyes follow smoothly), nystagmus (involuntary eye movements), and skew deviation (vertical eye misalignment). These findings distinguish between inner ear problems (peripheral) and brainstem/cerebellar problems (central/stroke).
3. What is the Epley maneuver and how does it work?
Answer: The Epley maneuver is a series of slow, controlled head and body positions that use gravity to guide dislodged crystals (otoconia) out of the semicircular canal and back into the utricle where they belong. It takes 10–15 minutes and has a 70–90% success rate in curing BPPV with a single session. The maneuver must be performed by a trained doctor.
4. Can I do the Epley maneuver at home myself?
Answer: While some modified versions exist for home use, the initial Epley maneuver should ideally be performed by a trained ENT specialist, neurologist, or physical therapist. They can confirm BPPV diagnosis with the Dix-Hallpike test before performing the maneuver, make sure proper positioning, and verify success. Improper technique can be ineffective or uncomfortable.
5. If I have brief positional vertigo, does that definitely mean I have BPPV?
Answer: Not necessarily. While BPPV is the most common cause of brief positional vertigo, other conditions can mimic it, including superior semicircular canal dehiscence (a bony defect), perilymphatic fistula, or even psychiatric dizziness. However, a positive Dix-Hallpike test and successful response to the Epley maneuver strongly support BPPV diagnosis.
6. What should I expect during vestibular neuritis recovery?
Answer: Recovery typically follows this pattern: (1) Peak vertigo in first 24 hours; (2) Gradual improvement over 2–4 weeks, with most recovery in the first 1–2 weeks; (3) Residual imbalance or motion sensitivity may persist for weeks to months. Early movement and vestibular rehabilitation exercises accelerate recovery. Long-term vestibular suppressants should be avoided as they slow the brain’s compensation process.
7. Why are vestibular suppressants discouraged in vestibular neuritis recovery?
Answer: Vestibular suppressants (like a vestibular suppressant) mask symptoms but actually delay the brain’s ability to compensate for the damaged vestibular nerve. The brain learns balance through movement and challenge. Early mobilization, even when uncomfortable, promotes faster compensation. Suppressing symptoms prevents this adaptive process, prolonging disability.
8. Can I develop BPPV again after the Epley maneuver?
Answer: Yes. While the Epley maneuver cures an episode by repositioning the crystals, BPPV can recur if crystals dislodge again. Recurrence rates are approximately 30% within 5 years. This is why BPPV is called “benign”—it is not dangerous, and recurrent episodes can be retreated with another Epley maneuver.
9. What is the most important feature that distinguishes vertigo caused by stroke from other causes?
Answer: The presence of neurological symptoms accompanying continuous vertigo is the strongest indicator of possible stroke. These include double vision, slurred speech, difficulty swallowing, weakness or numbness in limbs, severe ataxia (inability to sit or stand unassisted), and facial drooping. Any combination of continuous vertigo plus one of these symptoms demands emergency evaluation.
10. What does “direction-changing nystagmus” mean and why is it important?
Answer: Direction-changing nystagmus means involuntary eye movements that change direction based on where the patient looks—they beat to the right when looking right and to the left when looking left. This pattern is highly suggestive of brainstem or cerebellar involvement and is a red flag for stroke. Peripheral (inner ear) causes produce unidirectional nystagmus that beats in the same direction regardless of gaze.
11. How accurate is the HINTS exam for detecting stroke?
Answer: The HINTS exam has 100% sensitivity and 96% specificity for detecting acute brainstem strokes in the emergency setting within the first 48 hours. This makes it more accurate than early MRI, which can be false-negative in up to 50% of small brainstem strokes. The HINTS exam uses only eye movements and takes 60 seconds.
12. What is the critical time window for stroke treatment after symptom onset?
Answer: The window for thrombolysis (clot-busting medications like tPA) is 4.5 hours from symptom onset. The window for mechanical thrombectomy (clot removal via catheter) extends to 24 hours in some cases, depending on brain imaging findings and criteria. After these windows close, the treatment options become limited. This is why rapid diagnosis is critical.
13. If I have sudden vertigo and sudden hearing loss, what does that suggest?
Answer: The combination of sudden vertigo and sudden unilateral sensorineural hearing loss suggests possible infarction of the Anterior Inferior Cerebellar Artery (AICA), which supplies both the inner ear and the brainstem. This is a red flag for posterior circulation stroke and mandates immediate neuroimaging and stroke evaluation.
14. What is the difference between a Vertigo Diary and a medical consultation?
Answer: A Vertigo Diary is a self-recorded log of your symptoms—duration, triggers, associated symptoms, and recovery. A medical consultation involves a doctor’s physical examination, HINTS test, and diagnostic tests (hearing tests, imaging). The diary provides objective data that helps the doctor make faster, more accurate diagnoses. It is a complementary tool, not a replacement for professional evaluation.
15. Can anxiety cause vertigo that mimics peripheral or central causes?
Answer: Yes. Anxiety-related dizziness can present as vague unsteadiness or lightheadedness, and severe anxiety can occasionally trigger brief vertigo-like sensations. However, anxiety rarely causes the classic brief positional vertigo of BPPV or the days-long continuous vertigo of vestibular neuritis. If your Vertigo Diary documents true spinning with clear triggers and recovery patterns, organic causes (BPPV, neuritis, stroke) are more likely than anxiety alone.
16. Why shouldn’t I automatically assume my “chakkar” is just dizziness or low blood pressure?
Answer: Because “chakkar” is ambiguous, and different causes of vertigo require completely different treatments. Assuming low blood pressure and ignoring specific trigger patterns might delay diagnosis of BPPV (which needs Epley maneuver) or, worse, miss a stroke warning sign. Using your Vertigo Diary to document exact symptoms, triggers, and duration makes sure your doctor considers the full differential diagnosis.
17. What role does a hearing test (audiometry) play in diagnosing vertigo?
Answer: Audiometry (hearing test) helps differentiate peripheral from central causes. Sudden sensorineural hearing loss with vertigo suggests inner ear or AICA involvement. Vestibular neuritis should NOT cause hearing loss; if it does, imaging is warranted to rule out stroke or other central pathology. Audiometry is especially important if sudden hearing loss is new.
18. Can children have BPPV, vestibular neuritis, or stroke-related vertigo?
Answer: Yes, though frequencies differ. BPPV is rare in children but can follow head trauma. Vestibular neuritis is common in children 4–14 years and usually has an excellent prognosis. Pediatric posterior circulation strokes are rare but can occur with arterial dissection, cardiac disease, or clotting disorders. The HINTS exam and diagnostic approach are the same in children; red flag symptoms require the same urgent evaluation.
19. If my head impulse test is normal but I have continuous vertigo, what should I do?
Answer: A normal head impulse test with continuous vertigo is a red flag for central (brainstem or cerebellar) pathology, including stroke. Do not accept reassurance based on “normal” findings; specifically request MRI or CT angiography and ask for stroke protocol evaluation. Demand a neurology consultation if not already provided. Early imaging in this scenario is critical.
20. What is the best way to prepare for a vertigo diagnosis appointment?
Answer: (1) Complete a Vertigo Diary documenting all episodes from the past week or month; (2) Note all associated symptoms, especially neurological ones; (3) List all current medications; (4) Document any recent illnesses (colds, flu); (5) Prepare a timeline of symptom onset; (6) Arrive early to allow time for HINTS testing; (7) Ask your doctor specifically about your test results and what they mean for your diagnosis and treatment.
References
- Bhattacharyya N, et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngology–Head and Neck Surgery. 2017;156(3_suppl):S1–S47.
- von Brevern M, et al. Epidemiology of benign paroxysmal positional vertigo: A population based study. Journal of Neurology, Neurosurgery, and Psychiatry. 2007;78(7):710–715.
- Epley JM. The canalith repositioning procedure: For treatment of benign paroxysmal positional vertigo. Otolaryngology–Head and Neck Surgery. 1992;107(3):399–404.
This article is for educational purposes only. Please consult Dr. Prateek Porwal at Prime ENT Center, Hardoi or book an online consultation at 7393062200. Website: drprateekporwal.com
