Reviewed by Dr. Prateek Porwal, MBBS, DNB ENT, CAMVD. Dr. Porwal evaluates Meniere disease, vertigo, tinnitus, hearing fluctuation, VNG findings and balance disorders at Prime ENT Center, Hardoi.
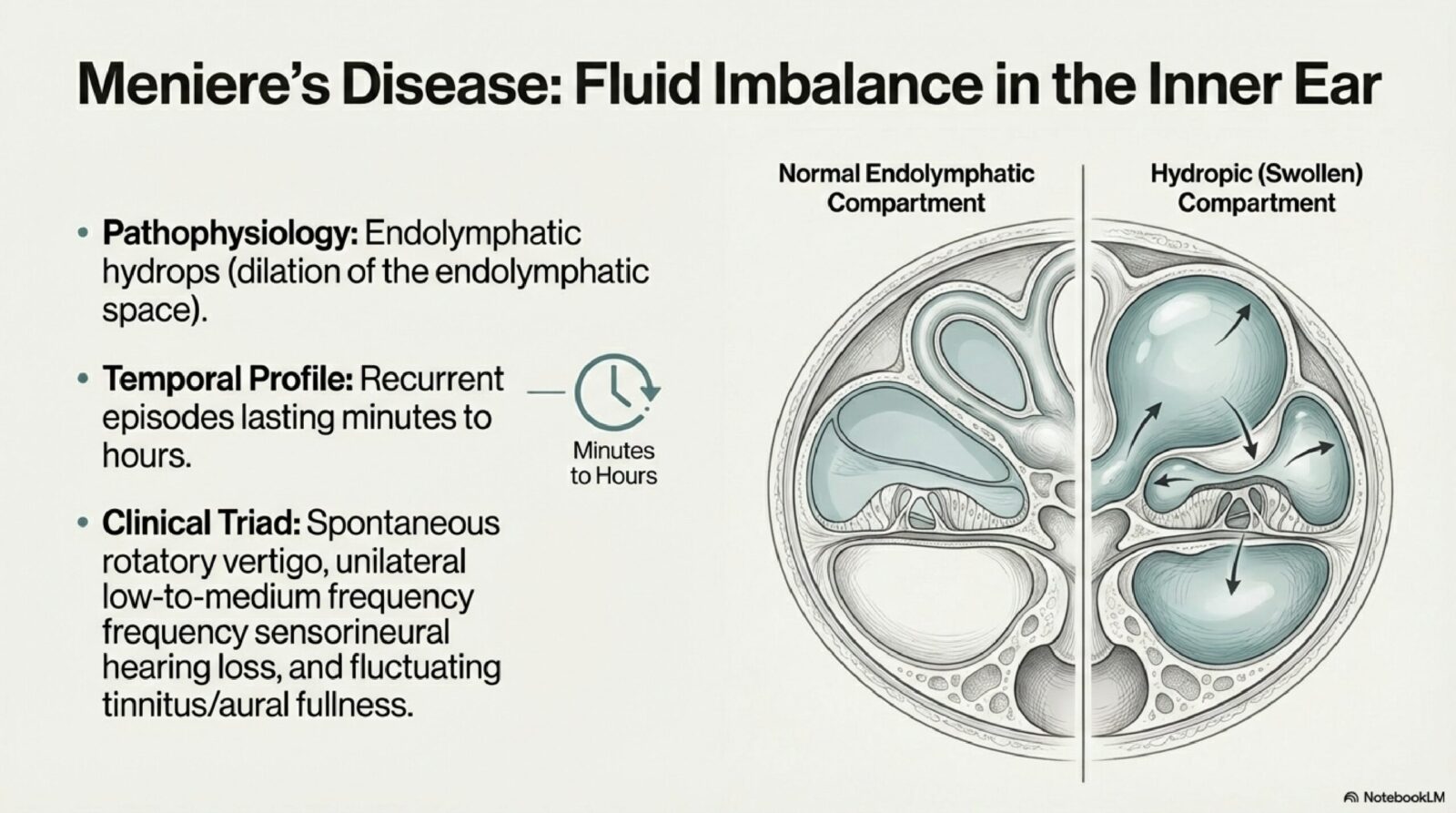
meniere vs bppv is part of a Meniere disease evaluation. The main question is whether vertigo attacks, tinnitus, ear fullness and hearing changes fit the same ear-focused pattern, or whether another diagnosis explains the symptoms better.
meniere vs bppv: quick answer
Meniere vs BPPV matters because the treatments are different. BPPV is a canal crystal problem that usually causes brief position-triggered spinning. Meniere disease causes longer spontaneous vertigo attacks with ear fullness, tinnitus and hearing fluctuation.
Why this topic matters
BPPV attacks usually last seconds to under a minute after rolling in bed, looking up or bending. Meniere attacks classically last 20 minutes to 12 hours and are not explained by a single head position. Meniere also needs hearing assessment because low-frequency sensorineural hearing loss supports the diagnosis.
How I check this in clinic
I compare the story with Dix-Hallpike, roll test, audiogram and nystagmus pattern. A patient may have both disorders, so a positive positional test does not automatically explain every longer attack with tinnitus.
What tests may be needed
Audiogram is usually the first anchor test because Meniere disease is linked with sensorineural hearing change. Depending on the case, VNG, vHIT, VEMP, MRI, blood pressure review or migraine screening may be needed. The AAO-HNS guideline also emphasizes checking for vestibular migraine when assessing suspected Meniere disease.
Red flags
Red flags include new neurological symptoms, severe gait ataxia, fainting, sudden hearing loss, persistent vertical nystagmus, or attacks that do not fit either BPPV or Meniere disease. These patients need broader assessment.
Treatment direction
BPPV treatment is canalith repositioning. Meniere management may include diet and fluid planning, attack medicines, hearing monitoring, betahistine or diuretics, vestibular rehab for chronic imbalance, and escalation when attacks remain disabling.
How it connects to the Meniere silo
Read the main Meniere disease guide first if you need the full overview. For attack pattern comparison, use Meniere vs BPPV and Meniere vs vestibular migraine. For testing, use the vertigo diagnosis guide and VNG testing guide.
If hearing is already poor or attacks remain disabling despite noninvasive care, treatment conversations may move toward intratympanic steroids, gentamicin or surgery. Those decisions should be based on attack severity, hearing status, daily risk and patient goals.
What patients should track
Keep an attack diary that records date, start time, duration, ear fullness, tinnitus side, hearing change, nausea, headache, visual symptoms, salt-heavy meals, sleep, stress, medicines taken and recovery time. Bring old audiograms because hearing trend is more useful than a single report.
Common mistakes
Do not diagnose Meniere disease from dizziness alone. Do not keep repeating Epley maneuvers for long spontaneous attacks with hearing fluctuation. Do not ignore migraine features. Do not start strict salt restriction or diuretics without considering blood pressure, kidney status and other medicines.
How follow-up changes the diagnosis
Meniere disease often becomes clearer over time. A first visit may only show probable disease, because hearing can fluctuate and the patient may arrive between attacks. Repeating audiograms, comparing the affected ear with the other ear, and documenting whether tinnitus or fullness appears before vertigo can prevent both overdiagnosis and missed diagnosis.
Follow-up also protects patients from the wrong treatment path. A patient whose attacks shorten to seconds may need positional testing for BPPV. A patient with headache, light sensitivity and motion sensitivity may need migraine care. A patient with progressive asymmetric hearing loss may need imaging or broader ear evaluation. The label should follow the evidence, not the other way around.
Safety and daily planning
During active Meniere disease, patients should think practically about safety. Avoid driving during an attack, avoid ladders and heights when attacks are unpredictable, sit or lie down when ear pressure and spinning begin, and tell family members what symptoms mean emergency care. Older patients and patients living alone need a fall plan.
The goal is not to make the patient afraid of normal life. The goal is to match risk to the pattern. Someone with rare mild attacks needs reassurance and monitoring. Someone with vomiting, falls, drop attacks or poor hearing needs a more structured plan and faster escalation.
FAQ
Can meniere vs bppv be diagnosed online?
No. Online information can help you prepare questions, but Meniere disease decisions need history, ear examination, audiogram and sometimes vestibular testing or imaging.
Is Meniere disease curable?
There is no guaranteed cure. Many patients can reduce attack burden and improve safety with staged care, but hearing and balance need follow-up over time.
References
AAO-HNS Clinical Practice Guideline: Meniere’s Disease key action statements: https://bulletin.entnet.org/home/article/21247843/clinical-practice-guideline-mnires-disease
NIDCD. Meniere’s Disease diagnosis and treatment: https://www.nidcd.nih.gov/health/menieres-disease
Merck Manual Professional. Meniere Disease: https://www.merckmanuals.com/professional/ear-nose-and-throat-disorders/inner-ear-disorders/meniere-disease
Tumarkin/drop attacks in Meniere disease, PubMed: https://pubmed.ncbi.nlm.nih.gov/24729095/
For non-emergency Meniere disease, vertigo, tinnitus, hearing fluctuation or VNG evaluation, call Prime ENT Center, Hardoi at 7393062200. Sudden weakness, double vision, slurred speech, severe headache, fainting or inability to walk needs urgent care first.
Medical disclaimer: This article is for educational purpose and patient education. Meniere disease can resemble vestibular migraine, BPPV and central vertigo. Diagnosis and treatment should be individualized after ENT evaluation and hearing testing.
