One of the first things I teach residents is that if you only know the Dix-Hallpike test for BPPV, you’re missing about 30% of your cases. The Dix-Hallpike is brilliant for posterior canal BPPV, probably 80-90% of all BPPV cases, but it misses horizontal canal BPPV completely. That’s where the supine roll test comes in. This post covers supine roll test horizontal in detail.

I used to have patients come back frustrated because they did the canalith repositioning maneuver in my clinic and felt better for a week, then got dizzy again. Often it was because they actually had horizontal canal BPPV all along, not posterior canal. Now I make sure to do the supine roll test on everyone before I commit to a treatment plan.
Why the Dix-Hallpike Isn’t Enough: Supine Roll Test Horizontal
The Dix-Hallpike test works by moving the otoliths (calcium carbonate crystals) out of their resting position in the horizontal plane. When you hang the patient’s head backward off the edge of the bed, you’re specifically testing the posterior semicircular canal.
But if the loose crystals are stuck in the horizontal canal instead, the Dix-Hallpike won’t move them enough to provoke nystagmus. The patient might have positive horizontal canal BPPV and get a completely negative Dix-Hallpike test. This is a trap I fell into myself early in my career.
What Is the Supine Roll Test?
The supine roll test (also called the Roll test or McClure test) specifically moves the patient in the horizontal plane to stimulate the horizontal canals. It’s simple but you have to do it right.
How to Perform the Test
Here’s my step-by-step approach:
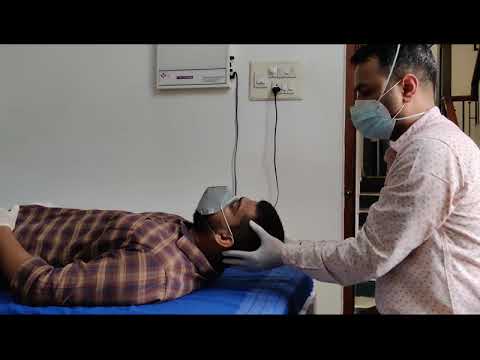
- Start position: Patient lies flat on their back on the examination table. This is supine position.
- Head positioning: The patient’s head should be aligned with their body, not hanging off the edge. I sometimes put a pillow under the head to keep the neck neutral.
- Eyes open: I ask the patient to keep their eyes open and watch for my finger as I move their head. Sometimes I do it with eyes closed too, but open is better for seeing nystagmus.
- Head rotation: I rotate the patient’s head about 45 degrees toward one side, over about 2-3 seconds. I’m looking for nystagmus.
- Hold and observe: I keep the head rotated for about 10 seconds, looking carefully at the eyes. Sometimes the nystagmus takes a few seconds to appear.
- Return to center: I slowly rotate the head back to center.
- Repeat other side: Then I rotate the head 45 degrees to the other side and repeat the whole thing.
- Check latency: I note the exact timing of any nystagmus, does it start immediately or after a few seconds? This tells me whether we’re dealing with canalolithiasis or cupulolithiasis.
The whole test takes maybe 2-3 minutes. Easy to do, but easy to miss if you don’t know what you’re looking for.
Reading the Nystagmus, Geotropic vs Apogeotropic
This is important. When the patient’s head rotates, the way their eyes move tells me exactly which side has the problem and what type of horizontal canal BPPV they have.
Geotropic Nystagmus
Geotropic means “toward the earth.” When I roll the patient’s head to the right, their eyes beat toward the right (in the direction of the roll). This is the most common type of horizontal canal BPPV, maybe 70-80% of horizontal canal cases.
Geotropic nystagmus suggests canalolithiasis, the crystals are floating freely in the horizontal canal. The affected canal is typically on the side toward which the eyes are beating.
Apogeotropic Nystagmus
Apogeotropic means “away from the earth.” When I roll the patient’s head to the right, their eyes beat to the left. This is less common but important to recognize because the treatment is slightly different.
Apogeotropic nystagmus usually means cupulolithiasis, the crystals are stuck to the cupula of the canal rather than floating freely. Or sometimes it means the crystals are on the opposite side of the canal.
Strong Side vs Weak Side
I also note the strength and duration of the nystagmus. If rolling right produces strong, long-lasting nystagmus but rolling left produces weak or no nystagmus, then the right horizontal canal is the problem.
Sometimes I’ll see direction-changing nystagmus, the nystagmus changes direction depending on which way I roll the patient. This tells me the crystals might be moving around or switching canals. It’s less common but definitely happens.
What Does Latency Tell You?
In true canalolithiasis, the nystagmus usually starts right away or within a second or two, the moving crystals immediately stimulate the cupula. Latency of more than 3-4 seconds suggests cupulolithiasis or possibly that we’re not dealing with simple BPPV at all.
Fatigue is also important. In canalolithiasis, if I repeat the roll several times, the nystagmus gets weaker each time, it fatigues. In cupulolithiasis, the nystagmus might stay strong because the cupula is constantly stimulated by the stuck crystals.
👉 Also read: సమతుల్యం వ్యాయామాలు — ఇంట్లోనే చేయటానికి 10 సులభ వ్యాయామాలు
Interpreting the Results
Okay, so I’ve done the supine roll test. What does each finding mean?
Geotropic nystagmus on one side: Horizontal canal BPPV with canalolithiasis. The affected side is the one toward which the eyes beat. This patient needs a horizontal canal repositioning maneuver.
Apogeotropic nystagmus: Horizontal canal BPPV with either cupulolithiasis or crystals on the canal wall. This usually needs barbecue maneuver or different positioning.
No nystagmus or very subtle nystagmus: Probably not horizontal canal BPPV. Might be posterior canal BPPV (which you’d catch with Dix-Hallpike) or might not be BPPV at all.
Vertical component nystagmus: Sometimes I see nystagmus that has both horizontal and vertical components during the roll test. This suggests you might be stimulating more than one canal, maybe a superior canal component too. Treatment becomes more complex.
When to Do the Supine Roll Test
I do the supine roll test on:
- Any patient with BPPV symptoms (brief spinning attacks, head-dependent)
- Patients who had Dix-Hallpike done but it was negative, I don’t want to miss horizontal canal BPPV
- Patients with recurrent BPPV after treatment, sometimes they have horizontal canal involvement
- Patients who describe horizontal spinning sensations rather than vertical
I don’t waste time waiting for an imaging test to diagnose BPPV. The supine roll test is diagnostic when positive. And it takes two minutes.
👉 Also read: સમતુલા કસરતો — ઘરે બેઠા કરી શકાય એવી 10 સરળ કસરતો
After You Find Horizontal Canal BPPV
Once I’ve confirmed horizontal canal BPPV with the supine roll test, I explain to the patient what we found and what treatment looks like. For canalolithiasis (geotropic), I usually do the Lempert roll maneuver (barbecue maneuver). For cupulolithiasis (apogeotropic), I might try the Gufoni maneuver instead.
The point is, if I didn’t do the supine roll test, I might have tried the standard Epley maneuver (which is for posterior canal) and been confused when it didn’t work.
My Clinical Experience
I had a 52-year-old woman come in with BPPV. Classic history, waking up with the room spinning, brief attacks triggered by rolling in bed. I did the Dix-Hallpike and got a negative result. But something about her history made me do the supine roll test anyway. Strong geotropic nystagmus to the right. Aha! Horizontal canal BPPV. I did the roll maneuver and she got much better. If I’d just relied on the Dix-Hallpike, I might have told her she probably didn’t have BPPV after all.
Another patient had recurrent BPPV that kept coming back. After treating for posterior canal BPPV three times without good lasting results, I finally tested for horizontal canal. Yep, that was the real problem. Different maneuver, complete resolution. Frustrating that I took so long to check.
The Bottom Line
The supine roll test is mandatory if you think a patient might have BPPV. It takes two minutes and can completely change your diagnosis and treatment. Too many patients are getting the wrong maneuver because doctors only know Dix-Hallpike. Don’t be one of those doctors.
If you have BPPV symptoms, make sure your doctor does both the Dix-Hallpike test AND the supine roll test. One test alone isn’t enough.
👉 Also read: Hiriyara Tale Tiruguvike
Contact Prime ENT Center
If you have vertigo-and-imbalance/”>vertigo or dizziness and need proper testing and treatment, call me at 7393062200 or WhatsApp https://wa.me/917393062200 to schedule an evaluation at Prime ENT Center in Hardoi.
This also applies to seniors and older adults who may face similar symptoms.
FAQ Schema
What is the difference between the Dix-Hallpike and supine roll test?
The Dix-Hallpike test the posterior semicircular canal by hanging the head backward, while the supine roll test checks the horizontal canals by rotating the head side to side while lying flat.
What does geotropic nystagmus mean in the supine roll test?
Geotropic nystagmus means the eyes beat toward the direction of head rotation. It indicates horizontal canal canalolithiasis and is the most common type of horizontal canal BPPV.
What does apogeotropic nystagmus indicate?
Apogeotropic nystagmus (eyes beating away from the direction of head rotation) suggests horizontal canal cupulolithiasis, where crystals are stuck to the canal wall rather than floating freely.
How many patients with BPPV have horizontal canal involvement?
Approximately 30% of BPPV cases involve the horizontal canal, which means a significant number of cases will be missed if only the Dix-Hallpike test (posterior canal) is performed.
What treatment is used for horizontal canal BPPV?
For canalolithiasis (geotropic nystagmus), the Lempert roll maneuver (barbecue maneuver) is typically used. For cupulolithiasis (apogeotropic), the Gufoni maneuver may be preferred.
How long does the supine roll test take?
The supine roll test typically takes 2-3 minutes to perform and can immediately diagnose horizontal canal BPPV without need for any imaging tests.
About Dr. Prateek Porwal
Dr. Prateek Porwal is an ENT & Vertigo Specialist with over 13 years of experience, holding MBBS (GSVM Medical College), DNB ENT (Tata Main Hospital), and CAMVD (Yenepoya University). He is the originator of the Bangalore Maneuver for Anterior Canal BPPV and has published research in Frontiers in Neurology and IJOHNS. Serving at Prime ENT Center, Hardoi.
Medical
When to See a Doctor
Seek immediate medical attention if you experience severe symptoms or sudden changes. For ongoing concerns, contact Prime ENT Center to schedule an evaluation. Early consultation often prevents complications and speeds recovery.
How to Prepare for the Test
Proper preparation helps make sure we get the most accurate results. Here’s what you should do:
- Avoid caffeine 24 hours before the test if possible
- Get adequate sleep the night before
- Wear comfortable, non-restrictive clothing
- Bring a list of current medications
- Arrange for someone to drive you home if you feel dizzy afterward
- Eat a light meal before arriving
At Prime ENT Center, we’ll explain every step of the process before we begin, so you know exactly what to expect.
Understanding Your Results
After your test, I review all data carefully and discuss findings with you in detail. Results typically indicate:
- Normal function
- Specific patterns associated with particular conditions
- Severity level of any dysfunction
- Recommended next steps for treatment
I always explain results in plain language, not medical jargon. We then work together to develop the best treatment plan for your situation.
Frequently Asked Questions
Q: How long until I see improvement?
A: Most patients notice improvement within days to weeks, depending on the condition. I’ll provide realistic timelines during your consultation.
Q: Do I need to take time off work?
A: This depends on your specific condition and treatment. We’ll discuss activity restrictions during your appointment.
Q: What if treatment doesn’t work?
A: We have multiple treatment options available. If one approach isn’t effective, we’ll adjust the plan. It’s rare that we don’t find something that works.
Q: Is treatment painful?
A: Most treatments are comfortable. I’ll explain what to expect and manage any discomfort during the process.
Disclaimer: This article is for educational purposes only. It does not constitute medical advice or prescribing guidance. All medications mentioned should only be taken under the direct supervision of a qualified physician. Specific doses, durations, and drug choices depend on your individual clinical condition and must be determined by your treating doctor. If you experience severe symptoms, please seek immediate medical attention.
References
- Bhattacharyya N, et al. Clinical Practice Guideline: Benign Paroxysmal Positional Vertigo (Update). Otolaryngology–Head and Neck Surgery. 2017;156(3_suppl):S1–S47.
Related: BPPV treatment guide.