Reviewed by Dr. Prateek Porwal, MBBS, DNB ENT, CAMVD. Dr. Porwal evaluates nystagmus, vertigo, VNG findings, HINTS patterns and balance disorders at Prime ENT Center, Hardoi.
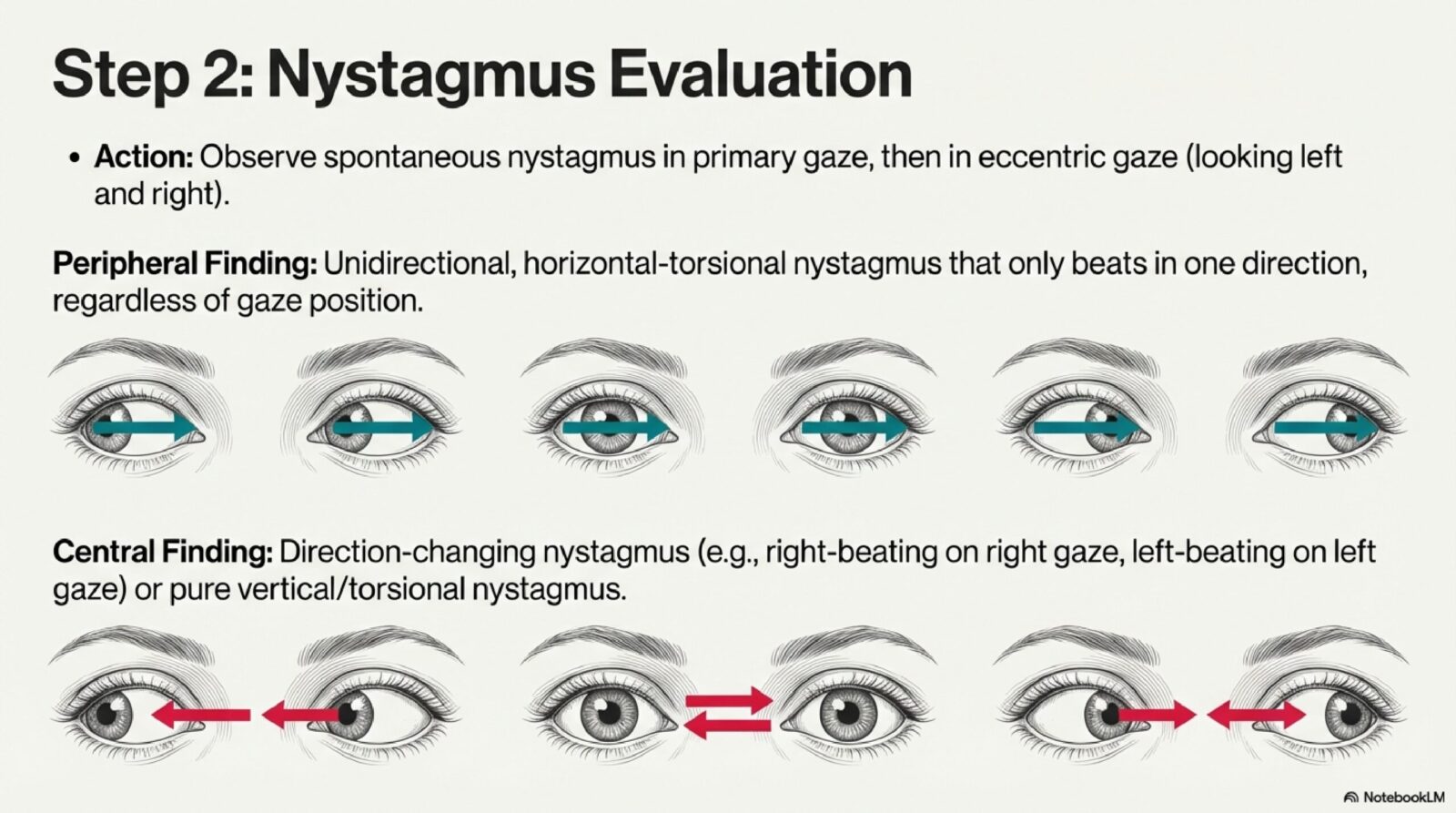
gaze-evoked nystagmus is a specialist eye-movement finding in vertigo and dizziness evaluation. It should be described carefully because the direction, trigger and associated symptoms can separate an inner-ear problem from a central neurological warning pattern.
gaze-evoked nystagmus: quick answer
Gaze-evoked nystagmus appears when the eyes are held away from center. It can occur from cerebellar or brainstem problems, medicine toxicity, alcohol, demyelination or other neurological causes.
What is gaze-evoked nystagmus?
The eyes normally hold an eccentric position steadily. If the neural integrator is weak, the eyes drift back and corrective fast phases create nystagmus. This is why gaze testing is part of careful vertigo and eye-movement examination.
Common causes
Common causes include sedatives, anticonvulsants, alcohol, cerebellar degeneration, multiple sclerosis, brainstem lesions and acute stroke patterns. It can also appear in patients with poor fixation or fatigue, so context matters.
How I evaluate it in clinic
I check whether the nystagmus is symmetric at both sides, whether it changes direction with gaze, whether there is spontaneous nystagmus in primary position, and whether there are neurological signs. VNG or video goggles can document subtle patterns.
Red flags
Direction-changing gaze-evoked nystagmus during acute continuous vertigo is a central warning sign in the HINTS framework. It should not be casually labelled as weakness or cervical dizziness.
Treatment direction
Treatment is not an eye drop. The cause must be found: medicine review, neurological evaluation, imaging when indicated, vestibular rehab for compensation, and emergency care when stroke signs are present.
How it connects to vertigo testing
I connect gaze-evoked nystagmus with the vertigo diagnosis guide, VNG testing, Frenzel goggles, and HINTS exam guide when the pattern suggests acute vestibular syndrome.
If the symptom is blackout or collapse rather than eye movement with spinning, read syncope vs vertigo. If the issue is bouncing vision while walking, dynamic visual acuity and vestibular rehab planning may be more relevant.
What to tell the doctor
Tell the doctor whether the eye movement is constant or position-triggered, whether vision bounces, whether there is double vision, whether symptoms started suddenly, whether walking is unsafe, and whether hearing loss, tinnitus, headache or neurological symptoms are present.
Common mistakes
Do not assume every positional nystagmus is BPPV. Do not assume every normal ear examination rules out a central problem. Do not keep repeating maneuvers if the nystagmus pattern does not match canal physiology or if neurological red flags are present.
What a good report should mention
A useful report for gaze-evoked nystagmus should mention the position of the eyes, the direction of the fast phase, whether fixation changes the movement, whether the pattern appears only in a certain gaze or position, and whether it fatigues. These details are more helpful than simply writing ‘nystagmus positive’.
The report should also say whether the pattern fits a peripheral vestibular disorder, a positional canal pattern, a central warning pattern, or an inconclusive result. If the report and symptoms do not match, the patient needs re-examination rather than automatic treatment.
Why this matters for treatment
The treatment path changes completely depending on the pattern. Canalith repositioning helps true BPPV. Vestibular rehabilitation helps many compensated or chronic vestibular problems. Migraine needs trigger and prophylaxis planning. Central patterns may need neurological imaging, emergency care, medicine review or specialist follow-up.
This is why eye-movement examination is one of the most valuable parts of vertigo practice. It keeps patients from being labelled with cervical vertigo, gas, weakness or anxiety when the eye movement is actually giving a stronger clue.
For gaze-evoked nystagmus, I also ask whether the patient has taken vestibular suppressants, sedatives, anti-seizure medicines or alcohol recently, because these can alter eye movements. Older reports, videos from previous attacks and medication lists can prevent a wrong conclusion.
If symptoms are intermittent, the examination can be normal between attacks. That does not make the patient unreliable. It means the timing of examination, trigger testing and video documentation become more important.
FAQ
Is gaze-evoked nystagmus always dangerous?
No. Some nystagmus patterns are expected in BPPV or vestibular neuritis. The concern depends on direction, trigger, persistence, fixation effect, associated symptoms and examination findings.
Can VNG record this eye movement?
Yes, VNG or video-oculography can document many eye-movement patterns. The report still needs clinical interpretation, because a tracing without the patient story can mislead.
References
Eggers SDZ et al. Barany Society classification of nystagmus and nystagmus-like movements: https://doi.org/10.3233/VES-190658
Kattah JC et al. HINTS to diagnose stroke in acute vestibular syndrome. Stroke. 2009: https://pubmed.ncbi.nlm.nih.gov/19762709/
Nystagmus Types. StatPearls, NCBI Bookshelf: https://www.ncbi.nlm.nih.gov/books/NBK539711/
For non-emergency vertigo, nystagmus, VNG or dizziness evaluation, call Prime ENT Center, Hardoi at 7393062200. Sudden weakness, double vision, slurred speech, severe headache, fainting or inability to walk needs urgent care first.
Medical disclaimer: This article is for educational purpose and patient education. Nystagmus can be peripheral or central. A new vertical, direction-changing, severe or neurological pattern should be assessed urgently.
