By Dr. Prateek Porwal, ENT & Vertigo Specialist | Prime ENT Center, Hardoi
Last Updated: February 2026 | VAI Budapest 2025 Award Recipient
If I had to pick one single intervention that helps the most vertigo patients recover, it’s vestibular rehabilitation therapy (VRT). Not medication. Not fancy imaging. Simple, targeted exercises that teach your brain to compensate. I see patients week after week do these exercises and gradually reclaim their livesgetting back to work, climbing stairs without fear, going shopping alone.
In my practice across Uttar Pradesh, I’ve treated thousands of patients with balance disorders. When dealing with vestibular rehabilitation therapy, The ones who recover fastest aren’t those who rest in bed or take pills indefinitely. They’re the ones who understand how their balance system works and actively retrain it. That’s what VRT does.
What Vestibular Rehabilitation Therapy Actually Does
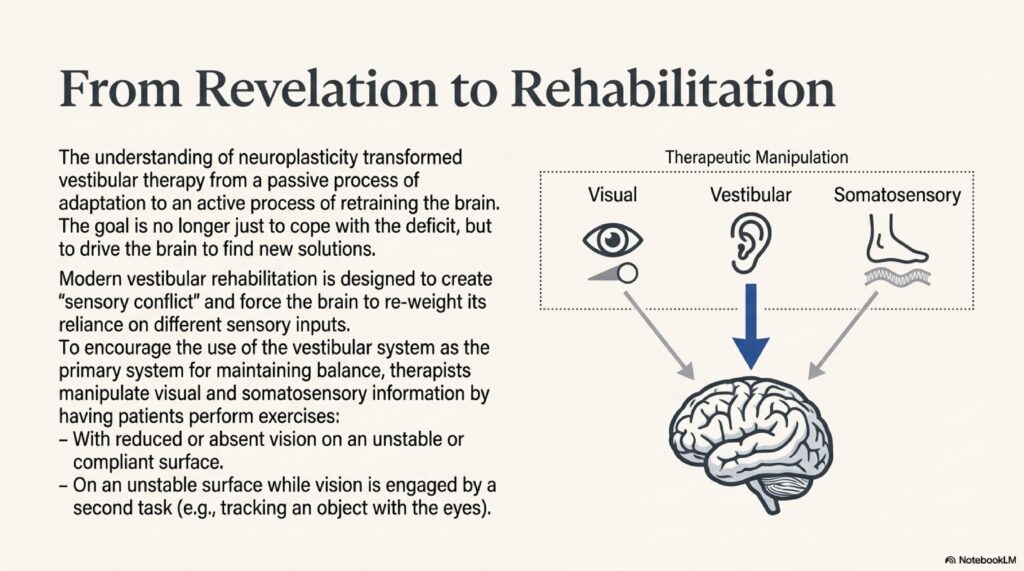
Vestibular rehabilitation works through neuroplasticitythe brain’s remarkable ability to rewire itself and create new neural pathways. When your balance system (inner ear) is damaged or not working properly, your brain doesn’t just accept defeat. It learns to compensate. Your eyes can take over some functions. Your proprioception (body position sense) can fill in gaps. VRT accelerates this natural compensation process.
Think of it this way: if one of your three balance sensorsvestibular, visual, or proprioceptiveis damaged, the other two can learn to work harder. VRT is like strength training for those remaining systems. Your brain’s neuroplasticity allows it to build new connections and new ways of interpreting balance information. This adaptation takes weeks or months, but it genuinely works.
The science is solid. When dealing with vestibular rehabilitation therapy, Studies show that patients who do VRT consistently recover significantly faster than those who simply wait for symptoms to improve. My own experience in clinic confirms this repeatedly. A patient with vestibular neuritis who starts VRT immediately will often be back to normal activities in 4-6 weeks, while someone who just rests might take 3-6 months.
The Three Core Mechanisms of VRT Recovery
1. Adaptation (Retuning the Vestibular System)
Adaptation is the brain’s ability to adjust its response to a compromised vestibular signal. If your left ear is damaged, it keeps sending wrong signals. But your brain can learn to ignore those faulty signals and rely more on your right ear, your eyes, and your body position sense. Over time, the bad signal becomes less important to your balance calculation.
This is why exercises that engage both ears together are important. They help your brain figure out which signal to trust. The damaged system’s signals gradually get dampened in the brain’s priority hierarchy.
2. Substitution (Other Systems Taking Over)
Your visual system can compensate for a damaged vestibular system. Your proprioceptive system (feeling where your body is in space) can also take over. VRT exercises specifically train these backup systems to work better. This is why gaze stabilization exercises are so powerfulthey’re training your eyes to do some of the work your inner ear normally does.
I explain it to patients like this: They’re always there, but usually they don’t need to work at full capacity. When dealing with vestibular rehabilitation therapy, VRT puts them through training to work at peak performance when needed.
3. Habituation (Getting Used to Triggering Movements)
Habituation is the most counter-intuitive principle of VRT but often the most effective. When a movement triggers your vertigo, your natural instinct is to avoid that movement. But avoiding it means your brain never learns to handle it. Habituation exercises deliberately expose you to the movements that cause dizziness, but in controlled, gradually increasing doses.
With repeated exposure, something remarkable happens: your brain stops treating that movement as a threat. The dizziness response diminishes. You might feel 80% dizzy on the first attempt, 60% on the third, 40% by the tenth. Eventually, the movement no longer triggers vertigo at all. This is habituation in action.

Vestibular Rehabilitation Therapy
The Three Types of Vestibular Rehabilitation Therapy Exercises Explained in Detail
Gaze Stabilization (Vestibulo-Ocular Reflex Training)
Your eyes should stay fixed on a target while your head moves. This stabilization is controlled by something called the vestibulo-ocular reflex (VOR). When your inner ear is damaged, this reflex becomes impaired. Your eyes drift instead of staying locked on target, and that’s when you experience oscillopsiathe feeling that the world is bouncing or jiggling when you move your head.
Gaze stabilization exercises retrain this reflex. The principle is simple: fixate on a point, then turn your head side-to-side while keeping your eyes locked on that point. As your vestibular system compensates, the muscles controlling your eye movements become more responsive. Over weeks, your eyes track better, and the oscillopsia improves.
I teach patients a practical progression:
- Week 1-2: Fixate on a large X on a piece of paper. Turn your head slowly side-to-side (20 reps, 2-3 times daily)
- Week 3-4: Same exercise but with eyes closed. This forces your proprioception to work harder
- Week 4-6: Do the exercise while walking, or while turning your head up-and-down instead of side-to-side
- Week 6+: Combine with other activitieswatching a video while turning your head, reading while moving your head
The goal is to gradually increase the challenge, forcing your brain to adapt and strengthen the eye-head coordination system.
Balance Training (Postural Stability and Proprioceptive Enhancement)
Balance training progressively challenges your body’s ability to maintain equilibrium. It starts simple and gradually increases difficulty as your system adapts.
The progression usually follows this pattern:
- Level 1 (Easiest): Stand on both feet with eyes open. Maintain balance for 30-60 seconds. This engages proprioception and vestibular input
- Level 2: Same position but eyes closed. Now proprioception has to work harder because visual input is gone
- Level 3: Stand on one leg with eyes open. Single-leg stance forces stronger proprioceptive compensation
- Level 4: Stand on one leg with eyes closed. Maximum proprioceptive challenge
- Level 5: Stand on a soft surface (pillow or foam pad) with eyes open. An unstable surface requires faster vestibular and proprioceptive responses
- Level 6: Soft surface with eyes closed. Very challenging; don’t attempt without support nearby
- Level 7: Dynamic activitieswalking while turning your head, walking in straight lines with eyes closed, tandem walking (heel-to-toe), turning in circles
- Level 8: Marching in place while focusing on a target, picking up objects from teh ground while maintaining balance, walking while looking up or down
I usually have patients practice 1-2 minutes at each level before progressing. When dealing with vestibular rehabilitation therapy, There’s no need to rush. The key is consistencydoing these exercises daily builds stronger neural connections.
Habituation Exercises (Systematic Desensitization)
Habituation exercises deliberately trigger small amounts of dizziness by repeating the movements that cause it. This seems counterintuitivewhy make yourself dizzy?but it’s powerful because habituation is how the brain stops treating a stimulus as threatening.
Common habituation exercises include:
- Head Turns While Walking: Walk slowly while turning your head side-to-side. The combined motion typically triggers dizziness in vestibular disorders, but repeated exposure reduces the response
- Head Bobs: Move your head up and down while standing or walking. Some people find vertical head movement more triggering than horizontal
- Quick Head Movements: After tolerance improves, make head movements faster. Speed increases the vestibular challenge
- Rolling in Bed: For BPPV specifically, roll from back to side to prone position repeatedly. Each roll redistributes crystals and can trigger dizziness, but repetition causes habituation
- Bending and Straightening: Bend forward to pick up an object, straighten quickly. This movement typically provokes dizziness initially but improves with repetition
The key principle: you want to trigger mild dizziness (3-4 out of 10 severity), not severe dizziness (8-10 out of 10). Mild dizziness allows habituation. Severe dizziness is counterproductive and scary. Once you trigger mild dizziness with an exercise, repeat it 5-10 times in a session. The response typically dampens across those repetitions.

Who Benefits Most From VRT and Who Doesn’t
Conditions That Respond Excellently to VRT
- Vestibular Neuritis: VRT speeds recovery significantly. Most patients with vestibular neuritis improve dramatically within 4-8 weeks of starting VRT, versus 3-6 months without it
- Labyrinthitis: Inner ear inflammation causing vertigo responds well to VRT because the goal is central compensation while the inflamed nerve recovers
- Chronic Balance Disorders and Bilateral Vestibular Loss: When vestibular function is permanently lost (bilateral vestibular hypofunction, for example), VRT becomes essential because there’s no damaged system that will recover. The goal shifts entirely to maximizing substitution and adaptation
- Vestibular Migraine: VRT combined with migraine prevention works well. Balance exercises improve stability between migraine episodes
- Post-Stroke Patients: Cerebellar or brainstem strokes damage central balance processing. VRT helps rebuild these pathways
- Post-Concussion Dizziness: Traumatic brain injury affecting vestibular pathways responds well to systematic rehabilitation
When VRT Is Not Indicated or Not Enough
BPPV patients: This is the most important distinction. BPPV is caused by crystals (otoconia) that have migrated into the semicircular canals. A repositioning maneuver like the Dix-Hallpike or Epley maneuver puts the crystals back where they belong. Once they’re repositioned, the system works fine again. VRT is unnecessary because there’s no vestibular damage to compensate forthe system is normal again.
I see many BPPV patients who’ve been doing months of VRT exercises unnecessarily. When dealing with vestibular rehabilitation therapy, They just needed one correct repositioning maneuver. That said, if BPPV recurs or if someone has concurrent balance dysfunction, then VRT might be helpful.
Acute Meniere’s attacks: During an acute attack (spinning, nausea, hearing loss), exercise makes everything worse. VRT should start only after the acute attack resolves. Between attacks, VRT can help with balance and adjustment to hearing loss
Central causes (tumors, strokes, multiple sclerosis): These often need different management. VRT helps with residual balance dysfunction but doesn’t address the primary problem
How Long Does VRT Take? Timeline and Expectations
This is the question every patient asks me: “How long until I feel better?”
The honest answer: it depends on your condition, your age, your consistency, and severity of the underlying problem.
Week 1-2: Most patients notice no improvement yet. They’re learning the exercises and establishing routine. But Some may notice slightly fewer severe episodes, but this is too early to celebrate
Week 2-4: Here’s where improvements start appearing. Patients report “dizziness isn’t as bad,” “I can turn my head faster,” “I walked to the market without holding onto anything.” These small wins matter psychologically and indicate the brain is adapting
Week 4-8: Significant improvements are standard. Most patients report major reduction in spinning sensation, better balance, ability to do activities they’d avoided. By week 6-8, 60-70% of patients are substantially better
Week 8-12: Further refinement. Remaining symptoms diminish. Confidence returns. Patients return to work, driving, complex activities
Beyond 12 weeks: For some conditions (especially bilateral vestibular loss or severe damage), adaptation continues for months. But most patients see their major improvement in the first 8-12 weeks
In my clinic in Hardoi, I’ve tracked outcomes carefully. Average recovery time:
- Vestibular Neuritis: 6-8 weeks with VRT (versus 3-6 months without)
- Labyrinthitis: 4-8 weeks
- Post-Concussion Dizziness: 6-12 weeks
- Chronic Balance Disorders: Ongoing improvement for 3-6 months or longer; focus shifts from recovery to management
Consistency matters more than duration. When dealing with vestibular rehabilitation therapy, A patient doing 20 minutes of exercises daily will improve faster than someone doing 1 hour once per week. Your brain needs regular input to establish new neural connections.
Practical VRT Exercises I Prescribe in My Practice
These are the core exercises I teach patients at PRIME ENT Center:
Basic Home Program (No Equipment Needed)
- The X Exercise (Gaze Stabilization): Write a large X on a piece of paper or print one. Hold it at arm’s length. Look at the X. Turn your head side-to-side slowly, keeping eyes on the X. Do 20-30 repetitions, 3 times daily. This directly trains your vestibulo-ocular reflex
- Marching in Place (Balance + Gaze): Stand while looking at a fixed point across the room. March in place, lifting knees high. Continue for 30-60 seconds. Do 3 sets daily. This combines balance training with visual fixation, increasing difficulty
- Head Turns While Walking (Habituation): Walk in a straight line (corridor, hallway, long room). While walking, slowly turn your head side-to-side. Do 2 full-length walks daily. This combines head movement with body movement, typically triggering mild dizziness that habituates with repetition
- Tandem Walking (Balance): Walk in a straight line with the heel of one foot directly in front of the toes of the other (like walking a tightrope). Walk 10-15 meters forward, turn, walk back. Do 2 times daily. This challenges proprioception and balance significantly
- Turning in Circles (Habituation + Vestibular Stimulation): Stand in the middle of a room. Slowly turn 360 degrees to the right. Pause. Turn 360 degrees to the left. Repeat 3-5 times. This repetitive rotation typically triggers dizziness initially but improves markedly with habituation. Do once or
- Bending and Standing (Habituation): Stand with feet shoulder-width apart. Bend forward from the waist to pick up an imaginary object from the ground. Stand back up quickly. Repeat 10 times. This vertical motion, especially the quick standing, often provokes dizziness in vestibular disorders but improves quickly with repetition. Do
- Single Leg Stance (Balance): Stand on one leg while holding a countertop or wall with light fingers (for safety, not support). Hold for 30 seconds. Relax. Switch to the other leg. Work up to 60 seconds per leg. Do. This forces profound proprioceptive engagement
- Stairs (Progressive Challenge): Once basic balance improves, climbing stairs with head turns is an excellent real-world VRT exercise. Walk up stairs normally. Walk up while turning your head side-to-side. Walk up while looking up and down. This mimics real-world demands on your balance system

Progression Principle
Start with exercises that are mildly challenging but not overwhelming. Each week, increase difficulty by:
- Increasing repetitions (from 10 to 15 to 20 reps)
- Increasing speed (slower movements to moderate speed to faster movements)
- Combining exercises (gaze stability + balance + movement all together)
- Removing visual input (same exercise with eyes closed, if safe)
- Changing surfaces (soft surface instead of flat floor)
Safety During VRT
VRT exercises can trigger dizziness. This is expected and necessary for improvement. But safety is critical:
- Initially do exercises near a wall, countertop, or with someone present
- Wear comfortable, non-slip shoes
- Remove tripping hazards from your exercise area
- Never exercise when severely fatigued or ill
- If you feel severe dizziness (8-10/10) or nausea during an exercise, stop and rest. Scale back the difficulty next session
- Mild dizziness (3-4/10) during exercises is expected and beneficial. Moderate dizziness (5-6/10) is acceptable if you can continue safely
Key Principles for VRT Success
- Consistency matters more than intensity: Daily 20-30 minute sessions beat once-a-week marathon sessions. Your brain builds new connections through repeated, regular input. Think of it like learning a languagedaily 30 minutes beats weekly 3-hour sessions
- Progress gradually: Don’t jump from level 1 to level 8 exercises in one week. Gradual progression allows your brain to adapt without overwhelming it. Each week, add slightly more challenge
- Motion causes improvement, not harm: This is the hardest lesson for patients to accept. Bed rest is harmful for vestibular disorders. Activity accelerates recovery. Gentle movement initially, but movement nonetheless
- Some dizziness during exercises is beneficial: This seems backwards, but mild dizziness is how your brain learns to compensate. You won’t fall and make things worse. You’ll actually improve. The dizziness indicates the brain is working on adaptation
- Patience is necessary: Recovery isn’t overnight, but improvement is measurable week by week. Don’t give up after 1-2 weeks. Give it at least 4-6 weeks of consistent effort before expecting significant improvement
- Document progress: Keep a simple diary. Rate your dizziness 0-10 daily. Track which exercises you did. This psychological reinforcement of improvement keeps you motivated when progress feels slow
India-Specific Challenges in VRT Compliance
In my practice in Uttar Pradesh, I see specific challenges that prevent patients from getting full benefit from VRT:
Patients stop too soon: In India, there’s often expectation that medical treatment should work immediately. VRT doesn’t work that way. Patients improve but gradually. Many stop after 2-3 weeks because they don’t see instant results. They miss the window where significant improvement happens (weeks 4-8)
Home exercises are inconsistent: Patients do exercises for a few days, then forget. They come to clinic for one session, receive exercises, but don’t practice daily. Consistency is everything in VRT. I now send WhatsApp reminders and have patients report back with photos/videos of their exercises
Cost of formal VRT sessions: Not all areas of Uttar Pradesh have access to qualified vestibular physiotherapists. Patients either travel long distances or skip formal therapy and try to do exercises at home without proper instruction. Teaching exercises correctly, even in clinic, helps tremendously
Confusion with other therapies: Some patients have been told they need expensive balance equipment or complex rehabilitation. Simple home exercises with proper instruction are often sufficient. I prioritize teaching over expensive devices
Bed rest culture: There’s still a misconception in parts of North India that vertigo means you should rest. The opposite is true. Gentle, progressive activity is necessary. I have to explicitly tell patients “exercise is healing, not harmful”
VRT Versus “Just Waiting It Out”
Some conditions improve over time without VRT. When dealing with vestibular rehabilitation therapy, Vestibular neuritis, for example, will often resolve in 3-6 months even without therapy because the inflamed nerve gradually heals. But this comparison misses the point:
With VRT: Recovery in 4-8 weeks, full function restored faster, confidence returns sooner, lower risk of developing chronic balance anxiety
Without VRT (just waiting): Recovery in 3-6 months, prolonged disability, higher risk of falls, development of anxiety around movement, potential for chronic vestibular-related anxiety
VRT doesn’t change the fundamental healing process, but it accelerates it significantly by actively training the brain’s compensation mechanisms rather than passively waiting for them to develop.
Think of it like a physical injury. A broken arm might heal in 6 weeks without any therapy. But with physiotherapy, you get better function, better strength, and return to normal activities much faster. VRT is the physiotherapy for your balance system.
When to Start VRT and When to Hold Off
When to start immediately:
- Vestibular neuritis diagnosed in clinic
- Labyrinthitis (after acute infection begins improving)
- Mild-moderate balance dysfunction from various causes
- Post-stroke balance recovery
- Chronic balance disorders
- Migraine-related dizziness
When to wait a few days or hold off:
- Acute Meniere’s disease attack (start after acute symptoms settle)
- Acute severe vertigo from any cause (too severe to exercise safely initially)
- New vestibular neuritis with severe nausea/vomiting (wait 24-48 hours for acute symptoms to improve)
- BPPV (not indicated if repositioning maneuver worksVRT is unnecessary)
Combining VRT with Other Treatments
VRT works best as part of a detailed approach:
VRT + Medication: Vestibular suppressant medications (like anti-nausea medication for nausea) are helpful in the first few days of severe vertigo to allow patients to function and begin VRT. But long-term medication dependency is not the goal. VRT should be started as soon as vertigo allows, with gradual medication reduction
VRT + Repositioning Maneuvers: For BPPV, the Epley maneuver or other repositioning maneuvers are first-line. VRT is not indicated unless BPPV recurs or concurrent balance problems exist
VRT + Migraine Prevention: For vestibular migraine, combine VRT with prophylactic migraine medications and lifestyle modifications
VRT + Dietary Modifications: For Meniere’s disease, combine VRT with dietary salt restriction and diuretics (if used) for detailed management
VRT + Psychological Support: Some patients develop anxiety around movement or falling. Combining VRT with cognitive behavioral therapy or reassurance about the safety of exercise improves outcomes
Special Considerations for Different Populations
VRT in Elderly Patients
elderly patients and seniors absolutely benefit from VRT and often improve as well as younger patients. When dealing with vestibular rehabilitation therapy, Modifications include:
- Increased emphasis on safety and support during exercises
- Slower progression of difficulty
- Accommodations for arthritis or other mobility limitations
- Potentially more supervision (family member present)
- Shorter exercise sessions (15-20 minutes instead of 30)
The improvement timeline is similar, but the risk of falls during exercise is higher, so careful progression is necessary.
VRT in Children and Teenagers
Young patients typically improve rapidly with VRT, often faster than adults. When dealing with vestibular rehabilitation therapy, The challenge is explaining the exercises and maintaining motivation. Gamifying the exercises (apps, videos, challenges) helps. Children’s brains are highly adaptable, so recovery is often faster.
VRT in Patients with Comorbidities
Diabetes, hypertension, arthritis, or other conditions complicate VRT but don’t prevent it. When dealing with vestibular rehabilitation therapy, Exercise modifications are necessary, and careful monitoring is important.
Frequently Asked Questions About Vestibular Rehabilitation Therapy About Vestibular Rehabilitation
How long until VRT helps and I notice improvement?
Many patients notice subtle improvement within 1-2 weeks if they’re consistent. When dealing with vestibular rehabilitation therapy, Significant improvement (that friends and family notice) usually takes 4-6 weeks of daily exercises. Major functional recovery often takes 8-12 weeks. The timeline depends on consistency, condition severity, and your age.
Can I do VRT exercises at home, or do I need a therapist?
Simple exercises can absolutely be done at home with proper instruction. When dealing with vestibular rehabilitation therapy, I teach basic exercises during clinic visits, and most patients do them independently at home. Complex cases or patients with severe anxiety about exercise benefit from working with a physical therapist. The key is getting correct instruction initially, then consistent home practice.
Will my vertigo return after I complete VRT?
For conditions that recover completely (like vestibular neuritis after vestibular rehabilitation), vertigo typically doesn’t return. For chronic conditions like Meniere’s disease, recurrent episodes are possible, but VRT helps you manage flare-ups when they occur. Some patients benefit from occasional refresher VRT exercises if balance gradually declines over years.
Is VRT better than medication for treating vertigo?
They’re complementary, not competing. Medication helps acute symptoms immediately, allowing you to function and begin VRT. VRT provides long-term recovery and prevention of chronic dysfunction. The best approach combines both initially, then gradually reduces medication as VRT improves function.
Can elderly patients safely do VRT?
Yes, absolutely. Elderly patients with balance disorders actually benefit greatly from VRT. Elderly brains are still capable of neuroplasticity, and exercise improves balance and reduces fall risk. VRT must be modified for safety and any mobility limitations, but age alone is not a contraindication. In fact, elderly patients who don’t do VRT have higher fall rates and slower functional recovery.
What if I do VRT for 6-8 weeks and it’s not helping?
This is relatively uncommon but requires reassessment. Possible explanations: incorrect diagnosis (the condition might not be vestibular), insufficient consistency with exercises, central causes like stroke or tumor that need different management, or atypical presentations. If VRT isn’t helping after 8 weeks of genuine effort, I recommend repeat evaluation by a vestibular specialist. Sometimes additional testing (like VNG testing or MRI) reveals the true cause and allows proper management.
My Clinical Experience with Vestibular Rehabilitation Therapy with VRT at PRIME ENT Center
Over the past 13+ years treating thousands of vertigo patients across Uttar Pradesh, I’ve seen VRT transform lives. Patients who thought they’d be permanently disabled return to work, driving, and normal activities. The most rewarding cases are elderly patients with severe balance dysfunction who regain confidence and independence through consistent VRT.
I’ve also learned what doesn’t work. Expensive equipment, complex programs, and infrequent therapy sessions produce poor results. Simple, daily exercises at home, with clear instruction and periodic reassessment, work remarkably well.
The patients who improve fastest are those who understand the science. Once they understand that their brain can actually rewire itself, that mild dizziness during exercises is beneficial, and that consistency matters more than anything else, they commit fully and improve dramatically.
VRT isn’t the answer for every vertigo patient (BPPV patients rarely need it, for example), but for the right conditionsvestibular neuritis, labyrinthitis, chronic balance disorders, bilateral vestibular lossVRT is . It’s the single most effective intervention in my practice for helping patients recover function and reclaim confidence in their bodies.
Experiencing vertigo or chakkar? Get diagnosed usually in one visit.
Dr. Prateek Porwal, ENT Surgeon & Vertigo Specialist at PRIME ENT Center, Hardoi UP has treated thousands of vertigo patients across Uttar Pradesh. VAI Budapest 2025 International Award recipient. Most BPPV cases resolved in the same appointment no long medication courses, no unnecessary MRIs.
Call/WhatsApp: 7393062200 | Chat on WhatsApp
Medical Disclaimer: This article is for educational purposes only. It does not constitute medical advice or prescribing guidance. All medications mentioned should only be taken under the direct supervision of a qualified physician. Specific doses, durations, and drug choices depend on your individual clinical condition and must be determined by your treating doctor. If you experience severe symptoms, please seek immediate medical attention.
References
- Hillier SL, McDonnell M. Vestibular rehabilitation for unilateral peripheral vestibular dysfunction. Cochrane Database of Systematic Reviews. 2011;(2):CD005397.
- Whitney SL, Sparto PJ. Principles of vestibular physical therapy rehabilitation. NeuroRehabilitation. 2011;29(2):157–166.
About the Author — Vestibular Rehabilitation Therapy Specialist
Dr. Prateek Porwal is an ENT & Vertigo Specialist with over 13 years of experience, holding MBBS (GSVM Medical College), DNB ENT (Tata Main Hospital), and CAMVD (Yenepoya University). He is the originator of the Bangalore Maneuver for Anterior Canal BPPV and has published research in Frontiers in Neurology and IJOHNS. Serving at Prime ENT Center, Hardoi.
