Vertigo in Women Over 50 — 5 Causes Your Doctor Might Miss
Vertigo in women over 50 is something I deal with almost daily in my OPD. And I’m not exaggerating. If I look at my last 100 vertigo patients, easily 40-45 of them were women between 48 and 65. There’s a reason for this skew, and it’s not just “age.” Hormones play a much bigger role than most doctors give them credit for.
I wrote this because I kept getting the same questions from patients and their families. “Doctor sahab, meri mummy ko bahut chakkar aate hain, kya yeh menopause se related hai?” The short answer is: often, yes. The long answer is this article.
Table of Contents
Why do women over 50 get vertigo more than men?
The numbers are pretty clear on this. BPPV, which is the most common cause of vertigo, affects women 2 to 3 times more than men overall. But in the 50-60 age group, that ratio jumps to about 4.4:1. Four and a half women for every one man. A 2020 study in Frontiers in Neurology confirmed that the female-to-male ratio peaks right around the perimenopausal period.
So what’s going on?
The inner ear has estrogen receptors. When estrogen levels drop during menopause (typically between 45-55 years), it affects the metabolism of otoconia, those tiny calcium carbonate crystals in your inner ear that are responsible for sensing gravity and linear movement. When these crystals degenerate or break loose, they fall into the semicircular canals and cause BPPV.
Think of it this way: estrogen was helping keep those crystals stuck where they belong. Take away the estrogen, and the crystals become more brittle, more likely to dislodge. Add vitamin D deficiency on top of that (very common in Indian women who don’t get enough sun exposure), and you’ve got a perfect setup for recurrent BPPV.
The 5 most common causes of vertigo in women over 50
Not all dizziness is BPPV. In my clinic I see women over 50 with vertigo from these causes, roughly in this order of frequency:
BPPV (Benign Paroxysmal Positional Vertigo) is by far the most common. The room spins when you change head position, especially rolling over in bed or looking up. Episodes last seconds to a minute. I diagnose this with the Dix-Hallpike test and treat it with repositioning maneuvers. Most women feel better after one sitting.
Vestibular migraine is the second most common and the most underdiagnosed. Women who had migraines in their 20s and 30s often develop vestibular migraine symptoms around menopause, sometimes without any headache at all. Just spinning, nausea, and light sensitivity. I’ve written about this in detail in my vestibular migraine treatment guide.
Meniere’s disease is less common but tends to worsen around menopause. The classic triad: vertigo attacks lasting 20 minutes to several hours, fluctuating hearing loss, and tinnitus. Hormonal changes seem to affect endolymph fluid regulation.
PPPD (Persistent Postural-Perceptual Dizziness) is what happens when anxiety and a prior vertigo episode team up. Very common in women over 50 who had one BPPV episode, recovered physically but developed chronic anxiety-driven dizziness. The vertigo is gone but the brain keeps expecting it.
Cervical issues and blood pressure changes round out the list. Postmenopausal women often develop orthostatic hypotension (blood pressure dropping when standing up), cervical spondylosis, or medication-related dizziness from the 3-4 new medicines they’ve been put on since turning 50.

The menopause-vertigo connection: what the research says
I want to be specific here because “menopause causes vertigo” is too simplistic.
A 2014 study published in the European Archives of Oto-Rhino-Laryngology found that BPPV incidence peaks in the perimenopausal window. The researchers identified estrogen receptors in the inner ear and linked declining estrogen levels to otoconial degeneration. Basically, the same process that weakens bones (osteoporosis) also weakens the tiny crystals in your ear.
A Taiwanese population-based study from 2017, published in Frontiers in Aging Neuroscience, took this further. They found that women aged 45-65 who were on estrogen replacement therapy had a dramatically lower incidence of BPPV. The hazard ratio was 0.01, which in plain language means HRT almost eliminated the excess BPPV risk.
Now, I’m not recommending HRT to prevent BPPV. That would be ridiculous — HRT carries its own risks including breast cancer and stroke. But it tells us something important about the mechanism. Estrogen protects the inner ear. Lose the estrogen, the ear becomes vulnerable.
What I actually recommend for my patients is simpler: get your vitamin D levels checked. A 2021 study in Otology & Neurotology showed that vitamin D supplementation reduced BPPV recurrence by about 24% in patients who were deficient. And in my practice, I’d say 7 out of 10 women over 50 with recurrent BPPV have vitamin D levels below 20 ng/mL.
How I diagnose vertigo in women over 50
The diagnostic approach doesn’t change based on gender, but I do pay extra attention to certain things in women over 50.
First, I take a very detailed history. “Chakkar” can mean many things. I need to know: is the room spinning (true vertigo) or are you feeling lightheaded/unsteady (not vertigo)? Does it happen when you change position? How long does it last? Any hearing loss or tinnitus? Any headaches? What medications are you on? When did menopause happen?
Then I do the clinical tests. The Dix-Hallpike test for BPPV, the supine roll test if I suspect horizontal canal involvement, a detailed cranial nerve exam, and I check blood pressure in lying and standing positions (to rule out orthostatic hypotension).
For cases that aren’t straightforward, I do a VNG (videonystagmography) test in my clinic. We’re one of the few centres in central UP with VNG capability. It maps eye movements precisely and tells me exactly which part of the vestibular system is involved.
I also routinely order blood tests for vitamin D, calcium, thyroid function, and HbA1c (diabetes affects the inner ear more than people realize).
Treatment: what actually works
Treatment depends entirely on the diagnosis. That’s why getting the right diagnosis matters more than anything.
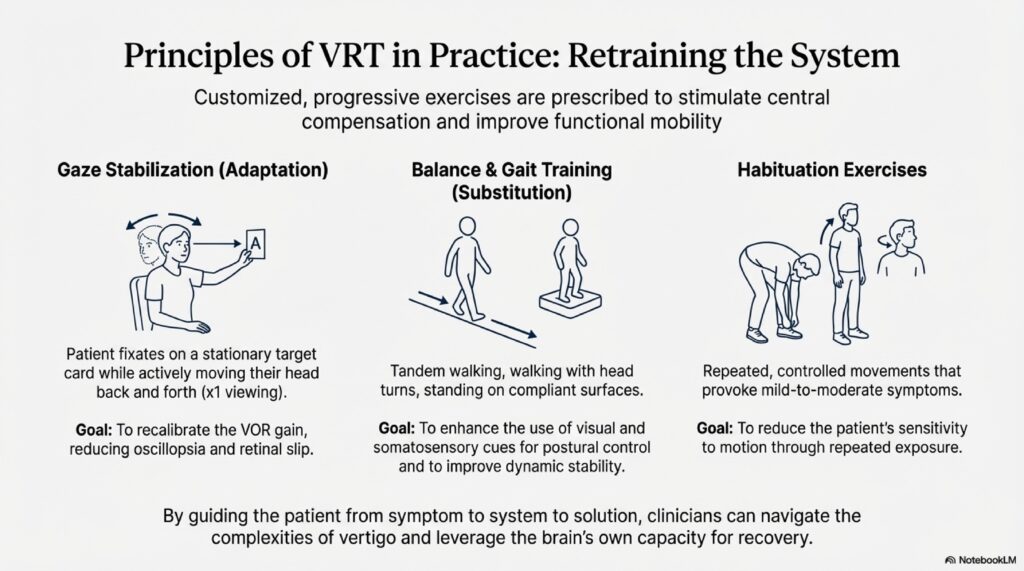
For BPPV, I do repositioning maneuvers in the clinic. The Epley maneuver for posterior canal BPPV, the BBQ roll for horizontal canal BPPV. Most women are significantly better after one session. For recurrent BPPV, I add vitamin D 60,000 IU weekly for 8 weeks, then maintenance dosing.
For vestibular migraine, we use preventive medications (low-dose amitriptyline or flunarizine work well in my experience) plus lifestyle modifications. Dietary triggers, sleep hygiene, stress management. I’ve found that women going through menopause often have disrupted sleep which makes vestibular migraine worse. Fixing the sleep sometimes fixes the vertigo.
For PPPD, it’s a combination of vestibular rehabilitation therapy, low-dose SSRIs, and frankly, a lot of reassurance. These patients need to understand that their brain is creating the dizziness, not their ear.
Medicines like betahistine (Vertin) and cinnarizine (Stugeron) are prescribed a lot in India for vertigo in women over 50. Honestly, they’re overused. Betahistine has some evidence for Meniere’s disease but for BPPV it does nothing. You can’t dissolve calcium crystals with a tablet. You need to physically move them. And cinnarizine just suppresses symptoms temporarily while the actual problem stays untreated.
Preventing recurrent vertigo after 50
Prevention in this age group comes down to a few practical things that I tell all my patients:
Keep your vitamin D levels above 30 ng/mL. Get it tested every 6 months. In Hardoi and most of UP, I find that women who cover their heads and spend most time indoors are almost universally deficient. Supplementation is cheap and safe.
Stay physically active. Walking 30 minutes daily does wonders for vestibular health. The vestibular system needs regular input to stay calibrated. Women who become sedentary after menopause have worse balance and higher fall risk.
Get your eyes and hearing checked regularly. The balance system depends on three inputs: inner ear, vision, and proprioception (joint sense). If two of these start declining with age, even mild vestibular dysfunction becomes a big problem.
Manage your other conditions properly. Uncontrolled diabetes, untreated thyroid problems, and unmanaged hypertension all worsen vestibular function. I see this pattern constantly in my OPD.
And if you’ve had one episode of BPPV, learn the home Epley maneuver. About 30% of my patients have a recurrence within a year, and knowing how to handle it at home gives them confidence and saves them an emergency visit.
When should you worry? Red flags
Most vertigo in women over 50 is BPPV or vestibular migraine. Scary, but not dangerous.
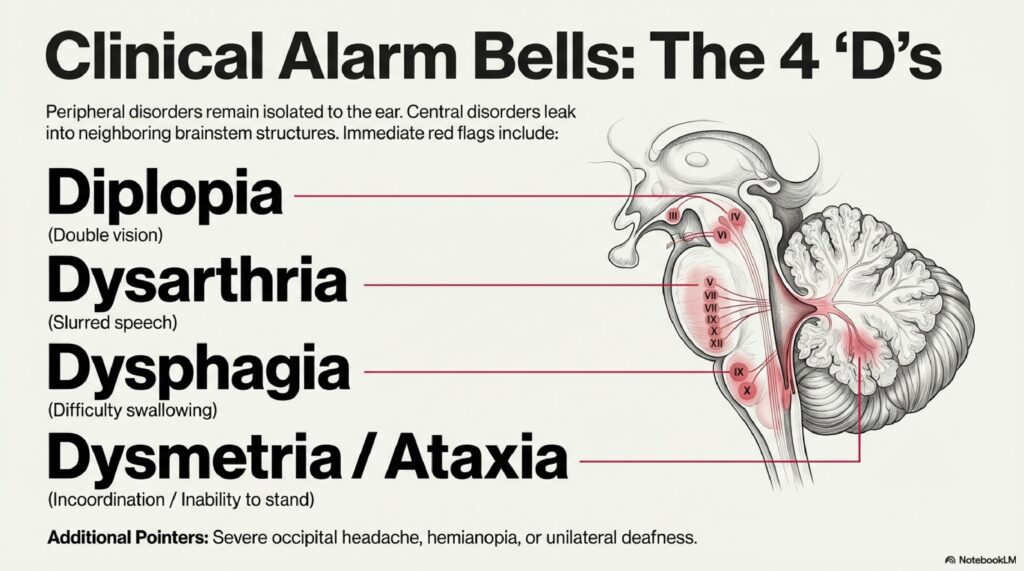
But there are red flags. If vertigo comes with sudden hearing loss in one ear, that’s an emergency. You have a 2-week window to treat sudden sensorineural hearing loss with steroids. Miss that window and the hearing loss may be permanent.
If vertigo comes with trouble speaking, facial drooping, weakness on one side, or the worst headache of your life, that could be a stroke. Don’t wait. Go to the nearest hospital.
And if dizziness is constant (not episodic), progressively worsening, and associated with headaches, I’d want to rule out a posterior fossa tumour with an MRI. This is rare, but I check for it when the presentation doesn’t fit the common diagnoses.
FAQs about vertigo in women over 50
Can menopause directly cause vertigo?
Menopause doesn’t directly cause vertigo, but the hormonal changes (especially estrogen decline) make the inner ear more vulnerable to conditions like BPPV. The estrogen drop affects otoconial metabolism, making the tiny ear crystals more likely to break loose. So menopause increases the risk of vertigo in women over 50, but it’s usually BPPV or vestibular migraine that’s the actual diagnosis.
Should I take HRT to prevent vertigo?
I don’t prescribe HRT specifically for vertigo prevention. While research shows HRT can lower BPPV risk, the decision to use HRT involves weighing many factors including cardiovascular and breast cancer risk. That’s a conversation to have with your gynaecologist. For vertigo specifically, vitamin D supplementation and repositioning maneuvers are safer, more targeted approaches.
Why do I get dizzy every morning when I get out of bed?
If the room spins briefly when you sit up or roll over, that’s classic BPPV. If you feel lightheaded or “blackout” feeling when standing up, that could be orthostatic hypotension, which is common in women over 50 especially if you’re on blood pressure medication. Either way, it’s treatable. Get it checked rather than just living with it.
Is vertigo in women over 50 linked to osteoporosis?
Yes, there’s a connection. The otoconia in your inner ear are made of calcium carbonate, similar in composition to bone. Osteoporosis reflects a systemic calcium metabolism problem, and the same process can affect the ear crystals. Women with osteoporosis have higher rates of BPPV. Another reason to keep your calcium and vitamin D levels in check.
How often does BPPV come back in older women?
Recurrence rates are about 30-50% within the first year, and they’re higher in postmenopausal women. But don’t let that discourage you. Each episode is treatable with a 5-minute maneuver. And vitamin D supplementation has been shown to reduce recurrence by about 24%. I teach all my patients the home Epley so they can manage mild recurrences themselves.
Dr. Prateek Porwal is an ENT surgeon and vertigo specialist with 13+ years of experience. He runs Prime ENT Center in Hardoi, UP, one of the few centres in central Uttar Pradesh with VNG testing and specialized vertigo treatment. For appointments, call the clinic or visit the website.
Disclaimer: This article is for informational purposes. It does not replace a face-to-face consultation with your doctor. Every patient is different and treatment decisions should be made after proper clinical evaluation.
Dr. Prateek Porwal
MBBS, DNB ENT, CAMVD
Vertigo & BPPV Specialist
Prime ENT Center, Nagheta Road, Hardoi, UP 241001
For appointments: Call or WhatsApp 7393062200
This article is for educational purposes only. Please consult Dr. Prateek Porwal at Prime ENT Center, Hardoi or book an online consultation at 7393062200. Website: drprateekporwal.com
