By Dr. Prateek Porwal, ENT & Vertigo Specialist | Prime ENT Center, Hardoi
Last Updated: February 2026 | VAI Budapest 2025 Award Recipient
Vertigo in elderly patients is remarkably common—approximately 30% of people over age 60 experience it at some point. But it’s also profoundly misunderstood. Often it’s dismissed as “just old age” or attributed to inevitable decline. This is wrong. In my practice across Uttar Pradesh, I see elderly patients who’ve been disabled for months or years because of undiagnosed or inappropriately treated BPPV, vestibular neuritis, or other treatable conditions. Vertigo in elderly is treatable — many could have recovered fully, but instead they became increasingly isolated, fearful, and dependent.
The stakes with elderly vertigo are higher than with younger patients. A young person with BPPV has brief episodes and feels fine between them. Vertigo in elderly has higher stakes — one episode, a fall, breaks a hip, enters the hospital, develops complications, and loses independence. The fall is the danger. This fundamentally changes how we approach elderly vertigoit’s not just about resolving dizziness; it’s about preventing catastrophic falls.
How Vertigo Presents in Older Adults
Older adults often don’t describe vertigo as “spinning.” Many say they feel “dizzy,” “unsteady,” or “off-balance,” so careful history-taking is essential.
Common descriptions include:
- Generalized dizziness (“woozy,” “the room feels unsteady”)
- Loss of balance or unsteadiness (wobbly walking, veering, needing support)
- Lightheadedness (feeling faint or like they may black out)
- Nausea and vomiting (sometimes less dramatic than in younger patients)
- Difficulty walking in darkness (when visual cues are reduced)
- Fear of falling (loss of confidence, activity avoidance)
- Hearing-related symptoms (tinnitus, hearing loss, ear fullness)
- Cognitive complaints (“brain fog,” poor concentration, feeling mentally unsteady)
Key Difference: Elderly vs Younger Patients
Why Vertigo in the Elderly Manifests Differently
The vestibular system doesn’t age gracefully. Multiple age-related changes occur simultaneously:
Hair cell loss in the inner ear: Hair cells in the semicircular canals and otolith organs naturally decline with age. By age 70, approximately 40% of hair cells may be lost. These cells don’t regenerate. This fundamental decline in sensory input means the inner ear sends less information to the brain.
Reduced central compensation: A young person’s brain compensates for partial vestibular loss quickly through neuroplasticity. An elderly brain is still capable of compensation, but it happens more slowly. The neural pathways take longer to establish. This is why recovery from vestibular neuritis takes months in elderly versus weeks in younger patients.
Declining proprioception: The body’s position sense deteriorates with age. This is the backup system for balance. When both vestibular and proprioceptive input decline, balance is severely compromised.
Vision changes: Visual acuity declines, contrast sensitivity diminishes (making movement in dim light harder), and coordination between eye and head movement slows. These visual contributions to balance become less reliable just when they’re most needed.
Muscle weakness (sarcopenia): Elderly lose muscle mass and strength, particularly in legs. This makes maintaining balance harder even with good vestibular input. A strong young person can compensate for vestibular loss with muscle strength. A weak elderly person cannot.
Vitamin D deficiency: This is common in India, especially among elderly with limited sun exposure. Vitamin D is important for vestibular function and bone health (preventing fractures from falls). Deficiency increases both vertigo risk and fall injury risk.
Polypharmacy effects: Elderly take multiple medications for hypertension, diabetes, arthritis, cardiac disease. Many of these antihypertensives, antihistamines, sedatives, pain medications affect balance and cause dizziness as side effects.
Common Causes of Vertigo in Elderly: What I See in Practice
BPPV (Benign Paroxysmal Positional Vertigo) – The Most Common
BPPV is far more common in elderly. In my practice, roughly 40% of elderly patients and seniors with vertigo have BPPV, compared to maybe 20% in younger populations. Why? Hair loss in the inner ear predisposes to otoconia (crystal) dislodgement. And elderly fall frequently, which dislodges crystals.
Presentation in elderly: Often triggered by minor head movements that young people wouldn’t notice rolling over in bed, getting up quickly, looking up at something. A single episode can last longer in elderly (though still typically under a minute). Nausea is common.
Diagnosis: The Dix-Hallpike test is standard, though in very stiff elderly patients with arthritis, positioning may be difficult. Alternative maneuvers (Semont, roll test) work equally well.
Treatment: Repositioning maneuver (Epley maneuver) done in office. Usually works in 1-2 sessions even in very elderly. I’ve successfully treated patients in their 90s. The key: careful positioning considering any arthritis or mobility limitations.
Why elderly are at higher fall risk: One episode of BPPV-induced vertigo and an elderly person falls hard. Bones are often osteoporotic. Hip fractures are common consequences. This is why I see BPPV treatment as urgent in elderly.
Vestibular Neuritis
Viral inflammation of the vestibular nerve causes sudden severe vertigo, nausea, unsteadiness. Onset is abrupt. The inner ear function may be partially or completely lost acutely.
In elderly: Recovery is much slower than in younger patients. A 30-year-old with vestibular neuritis might recover substantially in 4-6 weeks. A 75-year-old might take 3-6 months. The same condition, dramatically different timelines.
The risk: During the acute phase (first week), severe vertigo and nausea make it hard for elderly to safely move. But the moment acute symptoms improve, movement and VRT exercises become essential. Bed rest beyond the acute phase is harmful. Yet many well-meaning families insist on prolonged bed rest, which delays recovery and worsens deconditioning.
Treatment approach:
- Acute phase (days 1-3): Vestibular suppressants, anti-nausea medication, bed rest are appropriate
- Once nausea improves (day 3-7): Start gentle movements and balance exercises
- Ongoing: Progressive VRT exercises, gaze stabilization, balance training
- Important: Don’t prolong medication beyond acute phase. The goal is active recovery, not passive suppression
Vestibular Migraine
Less common in elderly than in younger patients, but does occur. Dizziness or vertigo accompanied by headache, light sensitivity, sound sensitivity, nausea. Sometimes vertigo is more prominent than headache.
Challenge in elderly: Distinguishing from other causes. Elderly often have multiple potential causes for dizziness. Careful history helps — migraine triggers, family history, pattern of symptoms.
Treatment: Identify and avoid triggers, prophylactic migraine medications if episodes frequent, supportive care during acute episodes.
Medication Side Effects and Polypharmacy
This is a hidden major cause of vertigo/dizziness in elderly that’s often missed. Common culprits:
Antihypertensive medications: ACE inhibitors, beta-blockers, diuretics, calcium channel blockersall can cause dizziness, orthostatic hypotension (dizzy on standing). The irony: the medication keeping blood pressure safe causes dizziness that causes falls.
Antihistamines: For allergies, sleeping aidscause sedation and dizziness
Pain medications: NSAIDs can cause inner ear problems; opioids cause dizziness and sedation
Psychiatric medications: Antidepressants, anti-anxiety drugsvestibular side effects
Diabetes medications: Can cause low blood sugar (hypoglycemia) which presents as dizziness and confusion
What to do: Review entire medication list carefully. Sometimes dose adjustment helps. Sometimes switching to a different medication in same class works (different antihypertensive with fewer vestibular effects, for example). Sometimes the dizziness benefit justifies continuing the medication because the underlying condition it treats is worse.
Work with the patient’s primary care doctor. Don’t stop medications without consultationsome are essential for life. But identifying which medications contribute to dizziness is important.
Stroke or Transient Ischemic Attack (TIA) – The Scary One
Sudden vertigo in an elderly person is stroke until proven otherwise. While BPPV is more common, missing a stroke is catastrophic.
Red flags for stroke (not simple peripheral vertigo):
- Associated weakness or numbness (facial, arm, leg)
- Associated speech difficulty or slurred speech
- Loss of coordination beyond just balance
- Sudden severe headache with vertigo
- Vision loss (partial or complete)
- Double vision
- Abnormal eye movements (nystagmus that’s different from BPPV)
- Nystagmus that’s vertical or torsional (typically indicates central cause)
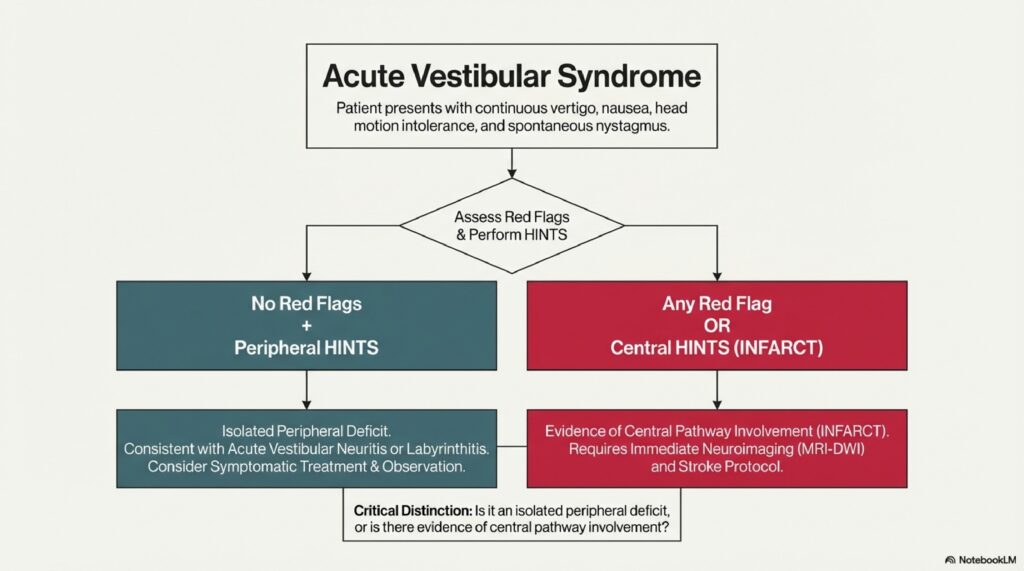
The HINTS exam: This bedside test (Head Impulse, Nystagmus, Test of Skew) can help distinguish peripheral from central causes of vertigo. It’s not perfect but helps guide urgency of imaging.
When in doubt, get MRI. Better to scan and be reassured than miss a stroke.
Bilateral Vestibular Hypofunction
Both sides of the vestibular system gradually lose function. This causes chronic unsteadiness (not true vertigo spinning sensation, but balance problems). The person feels unsteady, especially in dim light, moving their head makes them feel more unsteady.
Cause: Age-related degeneration, sometimes both inner ears affected by infections or ototoxic medications sequentially
Management: No cure, but VRT helps. The goal is maximizing remaining vestibular function and relying more on vision and proprioception. Walking with walking stick, making sure good lighting, careful movements all help.
Vertigo in Elderly: Special Diagnostic Challenges
Atypical presentations: Elderly sometimes don’t describe symptoms clearly. Instead of “the room is spinning,” they might say “I’m unsteady” or “I feel off balance.” This vagueness makes diagnosis harder. Careful questioning helps.
Multiple potential causes: A elderly patient might have BPPV AND medication effects AND vision decline AND arthritis-related mobility issues all contributing. Identifying which is primary is important.
Reduced cooperation with testing: Elderly with arthritis may not tolerate Dix-Hallpike positioning. Alternative tests (Semont maneuver, supine roll test) work instead.
Cognitive limitations: Some elderly have mild cognitive impairment. They may have trouble describing the onset and pattern of symptoms accurately. Information from family members becomes important.
Imaging challenges: Some elderly can’t tolerate MRI (claustrophobia, inability to remain still). CT scan sometimes substituted, though it’s less ideal.
Vertigo in Elderly: Why Fall Risk Is the Central Issue
Let me be clear: the goal with elderly vertigo isn’t just to reduce dizziness. It’s to prevent falls. Falls in elderly are catastrophic:
Statistics from my practice and literature:
- Falls are the leading cause of injury death in people age 65+
- Falls are the leading cause of nonfatal trauma in elderly
- One in four elderly have falls each year
- Hip fracture from fall leads to hospitalization, surgery, complications in 90% of cases
- A patient with hip fracture who was independent before often never regains independence afterward
- 1 in 5 elderly people who fracture hip die within a year of injury
- Vertigo increases fall risk 3-4 fold
The tragedy: It’s preventable. But A quick diagnosis (BPPVone maneuver), correct management (VRT for vestibular neuritis), medication adjustment (address blood pressure meds causing dizziness)these prevent the fall.
This is why I prioritize elderly vertigo. Treating a 75-year-old with vertigo aggressively might prevent a hip fracture that would steal their independence.
Vertigo in Elderly: Treatment Approaches
BPPV Management in Elderly
The Epley maneuver or other repositioning maneuvers work equally well in elderly as younger patients. Key modifications:
- Positioning carefully: Consider arthritis. If patient can’t tolerate head-hanging position of classic Epley, alternative maneuvers work (Semont, barbecue roll)
- Go slow: Don’t rush through positioning. Move slowly and carefully to avoid sudden vertigo or nausea
- Reassure continuously: Elderly may be more anxious. Reassurance reduces anxiety
- Success rate is high: 80-90% of BPPV resolves in 1-2 sessions even in very elderly
- Restrict head movements briefly after: For 24-48 hours after maneuver, advise against sudden head movements, sleeping on treated ear
Vestibular Neuritis Management in Elderly
Acute phase (first 3-7 days):
- Anti-nausea medication (ondansetron is gentler on elderly than older antihistamines)
- Vestibular suppressants briefly (dimenhydrinate, meclizine) only for first few days
- Bed rest initially while severe
- IV fluids if vomiting prevents adequate oral intake
Recovery phase (beyond one week): This is critical and where many elderly fail. The moment nausea allows, movement becomes essential.
- Start gentle head movements in bed
- Sitting up, standing up with support
- Walking with walker or rail, gradually increasing distance
- Formal VRT exercises
- Progress over weeks and months
- Full recovery may take 3-6 months in elderly (vs 4-8 weeks in younger)
Why prolonged bed rest is harmful: Deconditioning occurs rapidly in elderly. After a week of bed rest, elderly lose significant strength. Muscles atrophy. Balance worsens. Getting back up becomes harder. The original vertigo may improve but deconditioning makes them more unsteady. Avoid this trapmobilize as soon as medically safe.
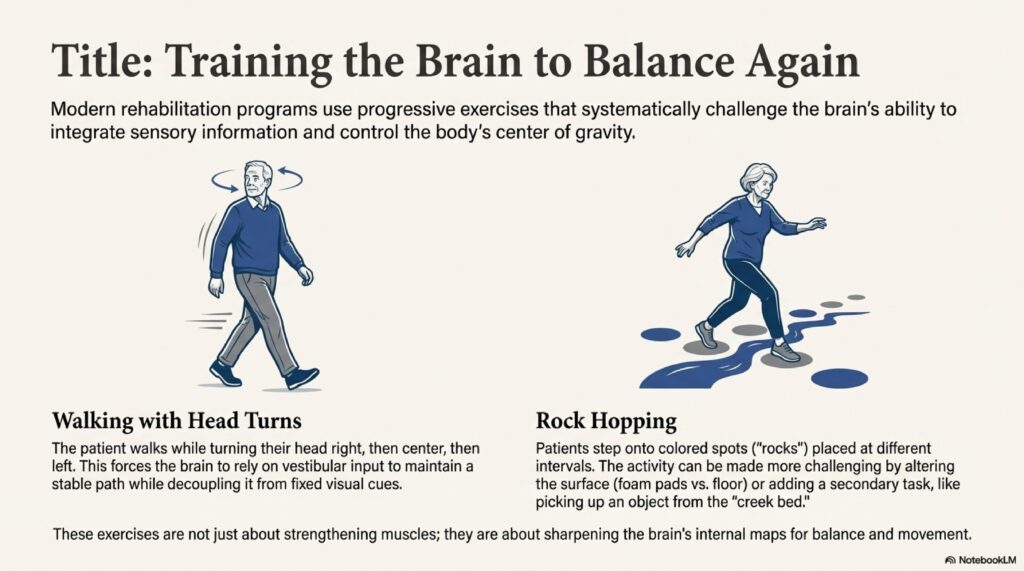
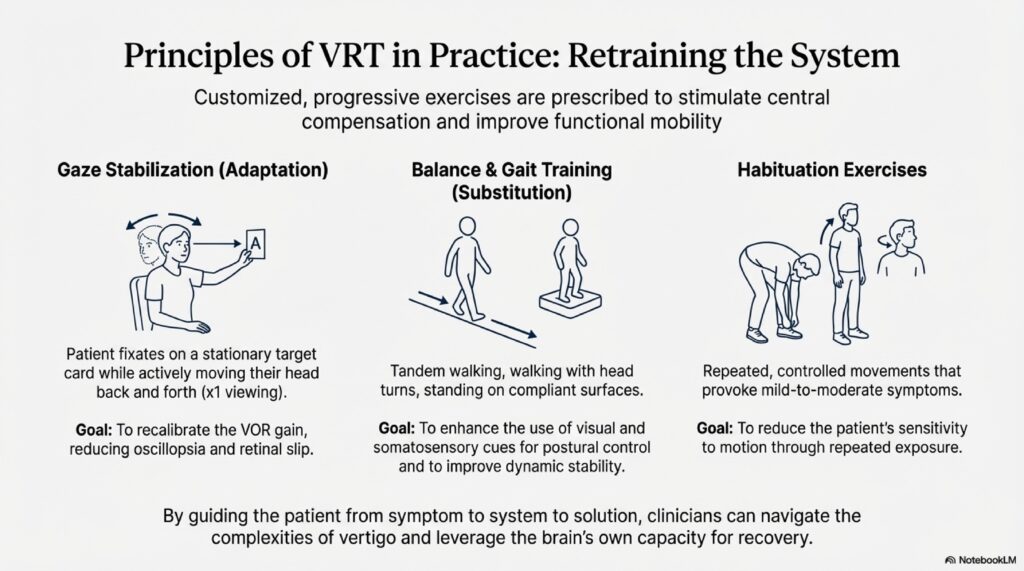
Vestibular Rehabilitation (VRT) in Elderly
VRT works well in elderly. Improvements take longer (3-6 months vs 4-8 weeks in younger), but they’re substantial. Key modifications:
Safety first:
- Exercises near wall or with walker nearby
- Family member or caregiver present initially
- Non-slip footwear
- Well-lit environment
- Gradual, careful progression
Modified exercises for limitations:
- If arthritis limits head movement, modify gaze stabilization
- If strength is poor, support balance training with chair or rail
- If vision is poor, more reliance on proprioceptive exercises (feeling body position)
- Shorter sessions (15-20 minutes) done multiple times daily vs one longer session
Motivation: Progress is slower, so encouragement matters. Show improvement (demonstrate on video that head movements are now smoother, that balance is visibly better). Small gains are meaningful victories.
Medication Considerations in Elderly with Vertigo
Avoid antihistamines: Meclizine, dimenhydrinate, promethazine cause drowsiness and fall risk in elderly. Use only very briefly (first 3-5 days) if nausea is severe
Avoid benzodiazepines: Diazepam, lorazepam increase fall risk, cause dependency, confusion. Avoid in elderly even if effective for acute vertigo
Prefer ondansetron: For nausea, ondansetron (Zofran) is safer than older antihistamines. Fewer side effects in elderly
Short-term medication only: Goal is to treat acute symptoms (nausea, severe dizziness) for a few days, then stop. Long-term medication is usually not indicated if diagnosis is correct
Review all medications: Work with primary care doctor to identify contributing medications. Sometimes small dose adjustment helps
Vertigo in Elderly: Home Safety Modifications
Prevention is critical. Modifying the home environment can prevent catastrophic falls:
Remove fall hazards:
- Loose rugssecure or remove
- Clutter in walkwaysclear pathways
- Low furnitureremove or make sure stable
- Wet floorsmop quickly, use non-slip mats in bathroom
Install safety features:
- Grab bars in bathroom, beside toilet, in shower
- Handrails on stairs, both sides if possible
- Non-slip flooring or non-slip mats
- Raised toilet seats with grab rails
- Walk-in shower with grab bar instead of tub (prevents falls getting in/out)
Improve visibility:
- Bright lighting in hallways, stairways, bedrooms
- Nightlights in hallways and bathroom for nighttime trips
- Remove bright lights that cause glare (glare affects balance)
- Good contrast in stairs (light edge stripe helpful)
Furniture placement:
- Clear paths from bed to bathroom
- Sturdy furniture to hold onto (secure furniture so it won’t move if leaned on)
- Avoid rearranging furnitureelderly deal with by memory
Mobility aids:
- Cane or walkeruse them! No shame in aids; they prevent falls
- Well-fitted aids; wrong height increases fall risk
- Shoes with good traction
Vertigo in Elderly: Caregiver Guidance
Family members often provide essential care:
Understanding the condition: Explain that vertigo is real, not “in the head.” Explain BPPV is benign but repositioning maneuver will help. Explain vestibular neuritis will improve but takes time and exercise, not bed rest.
Medication management: Make sure medications taken as prescribed. Keep updated list of all medications. Help identify which ones might contribute to dizziness.
Supervision during exercises: Elderly doing VRT should be supervised, especially initially. Prevent falls during exercises.
Transportation: Elderly shouldn’t drive during acute vertigo. Arrange transportation to doctor visits.
Nutrition and hydration: Make sure adequate nutrition and fluids. Dehydration worsens dizziness.
Emotional support: Vertigo frightens elderly. Loss of balance threatens independence. Reassurance and encouragement matter.
Vertigo in Elderly: Indian-Specific Scenarios
Joint family structure: Often 3-4 generations in one house. Can mean good supervision and support for exercises, or overprotection and insistence on bed rest.
Vitamin D deficiency: Common in India due to cultural dress practices (women in saris), pollution limiting sun exposure, dietary deficiency. Contributes to both vestibular dysfunction and osteoporosis (fracture risk). Supplementation important.
Limited access to rehab care: Many areas don’t have physical therapists trained in VRT. Teaching family to help with exercises or telemedicine guidance helps.
Stigma around balance problems: Some elderly reluctant to use canes or admit to balance issues. Overcoming this reluctance through education important.
Pressure to lie down: Cultural belief in rest for illness means family insists on prolonged bed rest. Education that movement helps is necessary.
Frequently Asked Questions
Is vertigo a normal part of aging?
It’s common (30% of people 60+) but not inevitable. Just because you’re elderly doesn’t mean you have to accept vertigo. Proper diagnosis and treatment often resolve it or significantly improve it, even in very elderly patients.
Will my vertigo improve at my age?
Yes, typically significant improvement occurs. Vertigo in elderly takes longer to recover than in younger people (sometimes 3-6 months vs 4-8 weeks), but meaningful improvement is common with appropriate management and consistent exercise. Age alone is not a reason to accept vertigo.
Is it safe for me to exercise with vertigo?
not just is it safe, it’s essential for recovery. Movement and balance retraining accelerate recovery. Do exercises in safe environmentnear wall or with help initiallybut exercise is important. Avoid bed rest beyond the acute phase.
How many medications do I need for my vertigo?
Depends on cause. BPPV needs none (just a repositioning maneuver). Vestibular neuritis may benefit from anti-nausea medication briefly, or migraine prevention if that’s the cause. Goal is to address root cause, not just suppress symptoms with long-term medication. Most elderly vertigo needs minimal medication once cause is identified.
What should I do immediately when vertigo strikes?
Sit or lie down safely, avoiding sudden movements. Focus eyes on a fixed point. Call for help if needed or if you feel like you might fall. Most episodes pass within minutes to hours. Once acute symptoms improve, gradual movement helps recovery.
Can surgery help my vertigo at my age?
Rarely. Surgery is last resort for severe, untreatable Meniere’s disease. Most elderly vertigo is managed successfully with proper diagnosis, medical management, and rehabilitation. Very few elderly vertigo patients need surgery.
Vertigo in Elderly: My Clinical Observations from UP
In 13+ years treating elderly vertigo patients across Uttar Pradesh, I’ve seen outcomes transform with proper management. The elderly patient who comes in terrified, thinking they’re having a stroke, feeling like they’re losing independenceseeing them recover and return to their normal activities is deeply satisfying.
I’ve learned that elderly respond excellently to treatment when the diagnosis is correct and when they’re motivated to do their exercises. The ones who recover fastest are those with family support, clear understanding of their condition, and motivation to maintain independence.
I’ve also learned the tragedy of delayed diagnosis. An elderly person with undiagnosed BPPV who falls and breaks a hip faces a trajectory that often leads to loss of independence, depression, and shorter lifespan. This is preventable.
The key message: elderly vertigo is common but treatable. Don’t accept “it’s just old age.” Get proper diagnosis. Do your exercises. Prevent falls. The investment of a few weeks in proper management can preserve independence for years or decades.
Experiencing vertigo or chakkar? Get diagnosed usually in one visit.
Dr. Prateek Porwal, ENT Surgeon & Vertigo Specialist at PRIME ENT Center, Hardoi UP has treated thousands of vertigo patients across Uttar Pradesh. VAI Budapest 2025 International Award recipient. Most BPPV cases resolved in the same appointment no long medication courses, no unnecessary MRIs.
Call/WhatsApp: 7393062200 | Chat on WhatsApp
Medical Disclaimer: This article is for educational purposes only. It does not constitute medical advice or prescribing guidance. All medications mentioned should only be taken under the direct supervision of a qualified physician. Specific doses, durations, and drug choices depend on your individual clinical condition and must be determined by your treating doctor. If you experience severe symptoms, please seek immediate medical attention.
References
- Tinetti ME, Williams CS, Gill TM. Dizziness among older adults: A possible geriatric syndrome. Annals of Internal Medicine. 2000;132(5):337–344.
About the Author — Vertigo In Elderly Specialist
Dr. Prateek Porwal is an ENT & Vertigo Specialist with over 13 years of experience, holding MBBS (GSVM Medical College), DNB ENT (Tata Main Hospital), and CAMVD (Yenepoya University). He is the originator of the Bangalore Maneuver for Anterior Canal BPPV and has published research in Frontiers in Neurology and IJOHNS. Serving at Prime ENT Center, Hardoi.
