Related Reading
- Semont Maneuver: BPPV Treatment (70-90% Success)
- The Cervical Vertigo Misdiagnosis Trap: Why Neck X-Rays Mislead
- Dix-Hallpike Test – Gold Standard for BPPV Diagnosis
- BBQ Roll Maneuver: Treatment for Horizontal Canal BPPV
- Supine Roll Test, Diagnosing Horizontal Canal BPPV
By Dr. Prateek Porwal, DNB ENT | Prime ENT Center, Hardoi
Let me start with a patient I still remember clearly. A 58-year-old woman came to me after being told by two different doctors that her vertigo was “anxiety-related.” She had been on betahistine for four months with no improvement. When I did the Dix-Hallpike test in my clinic, she had a very characteristic downbeat nystagmus. It lasted about 25 seconds, fatigued with repetition, and was clearly positional. This was anterior canal BPPV — a diagnosis that gets missed far too often because most doctors simply aren’t looking for it.
After one session of the Bangalore Maneuver, she was symptom-free.
I’m writing this to explain what the Bangalore Maneuver is, how it works, and why we developed it in the first place — because there’s a lot of confusion out there about anterior canal BPPV and how to treat it.
What Is Anterior Canal BPPV, and Why Is It So Underdiagnosed?
BPPV — Benign Paroxysmal Positional Vertigo — happens when calcium carbonate crystals (called otoconia or “ear stones”) get displaced from the utricle and enter one of the three semicircular canals. The posterior canal is affected in about 80-85% of cases. The lateral canal accounts for another 10-15%. And the anterior canal? Less than 5% of cases.
Because anterior canal BPPV is rare, most textbooks barely mention it. Most ENT residency programs don’t teach a specific maneuver for it. And the hallmark sign — downbeat nystagmus on positional testing — immediately makes clinicians nervous, because downbeat nystagmus is also a feature of serious central pathology like cerebellar or brainstem lesions.
So what typically happens? The doctor sees downbeat nystagmus, orders an MRI, the MRI comes back normal, and the patient gets labelled as “central vertigo — cause unclear” or sent home with vestibular suppressants. Months pass. The patient suffers.
Read my article published in frontiers of neuro-otology on 13 cases of anterior canal BPPV and Pubmed.

The difference between central downbeat nystagmus and the positional downbeat nystagmus of anterior canal BPPV is actually quite identifiable if you know what to look for. In AC-BPPV, the nystagmus is triggered specifically by the Dix-Hallpike or supine head-hanging position, has a short latency, fatigues with repeated testing, and resolves within 60 seconds. Central nystagmus tends to be direction-fixed, non-fatiguing, and present in multiple positions. This distinction is critical — and it is something that can be learned, but requires deliberate training.
Why a New Maneuver Was Needed
Before we developed the Bangalore Maneuver, the main option for anterior canal BPPV was the Yacovino maneuver (also called the deep head-hanging maneuver). It works by using gravity in a straight sagittal plane to guide crystals from the anterior canal through the common crus and back into the utricle.
The Yacovino maneuver is useful and was an important contribution to vestibular medicine. But it has two significant limitations that we kept running into clinically.
First, it requires extreme neck extension — full deep head-hanging off the examination table. Many of our patients, particularly older individuals with cervical spondylosis (which is extremely common in North India), simply cannot tolerate this position. Trying to force the position in a 70-year-old with a stiff neck is both painful for the patient and counterproductive because muscle guarding prevents the head from reaching the required angle.
Second, the Yacovino maneuver does not have a rotation component. It assumes the crystal clump is sitting perfectly in the midline of the canal. But what if the debris is off-center? What if there is a canal stricture, or a larger clump that needs an additional rotational force to mobilize it? In those cases, straight sagittal movement alone is not enough.
These were the real-world problems that drove us to develop a different approach.
The Bangalore Maneuver: Step by Step
The Bangalore Maneuver was developed by myself along with Dr. Srinivas Dorasala and Dr. Pradeep Vundavalli. It has been validated in a series of 48 patients with confirmed anterior canal BPPV diagnosed between 2018 and 2024. All 48 patients achieved complete symptom resolution — confirmed by repeat Dix-Hallpike and supine head-hanging tests showing no residual nystagmus.
One practical advantage worth mentioning upfront: this maneuver does not require lateralization — meaning you don’t need to identify whether it’s the right or left anterior canal that’s affected. This simplifies clinical decision-making considerably, since lateralization of anterior canal BPPV from nystagmus patterns is often ambiguous.
The maneuver is performed in four steps:
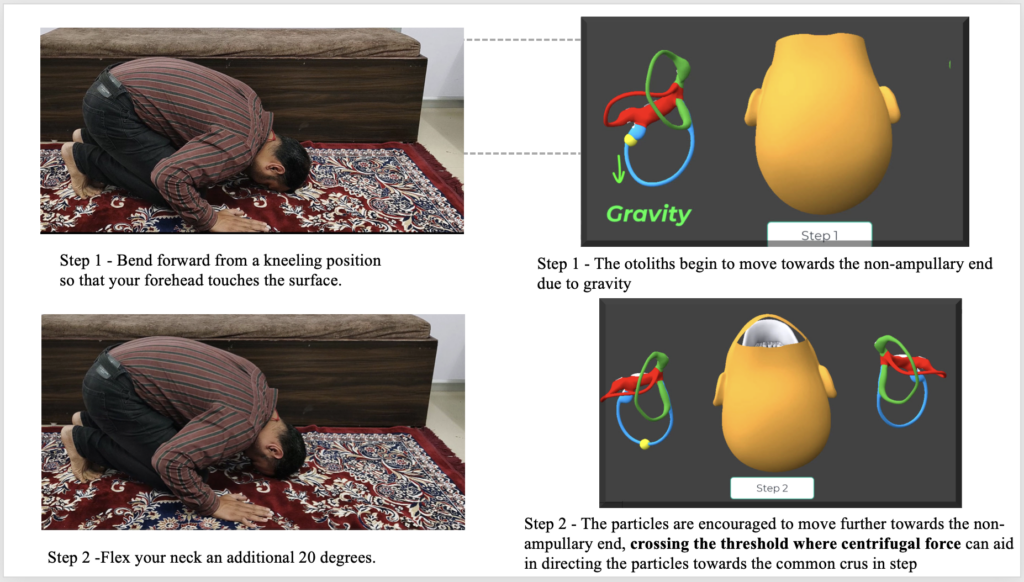
Step 1 — Forehead-to-Floor Position
The patient kneels on the examination table (or on a firm surface), then bends forward until the forehead touches the surface — similar to a child’s pose in yoga, if your patients are familiar with that reference. The nose points straight down toward the floor.
In this position, gravity acts directly on the anterior canal. The otolith debris begins moving toward the non-ampullary end of the canal — away from the sensory cells. This is the essential first movement that sets up everything that follows.
Hold this position for 30-45 seconds, or until any dizziness the patient feels begins to settle.
Step 2 — Additional Neck Flexion of 20°
Without lifting the forehead from the surface, the patient is asked to flex the neck an additional 20 degrees. This sounds subtle, but it’s actually the step that does the critical geometric work.
This extra 20° of flexion deepens the angle of the anterior canal relative to gravity, pushing the debris further along the non-ampullary direction — past an important anatomical threshold. Once the debris crosses this threshold, it comes within reach of the common crus, the shared passageway connecting the anterior and posterior canals to the utricle. The centrifugal force in the next step can then take over.
Hold for another 30 seconds.
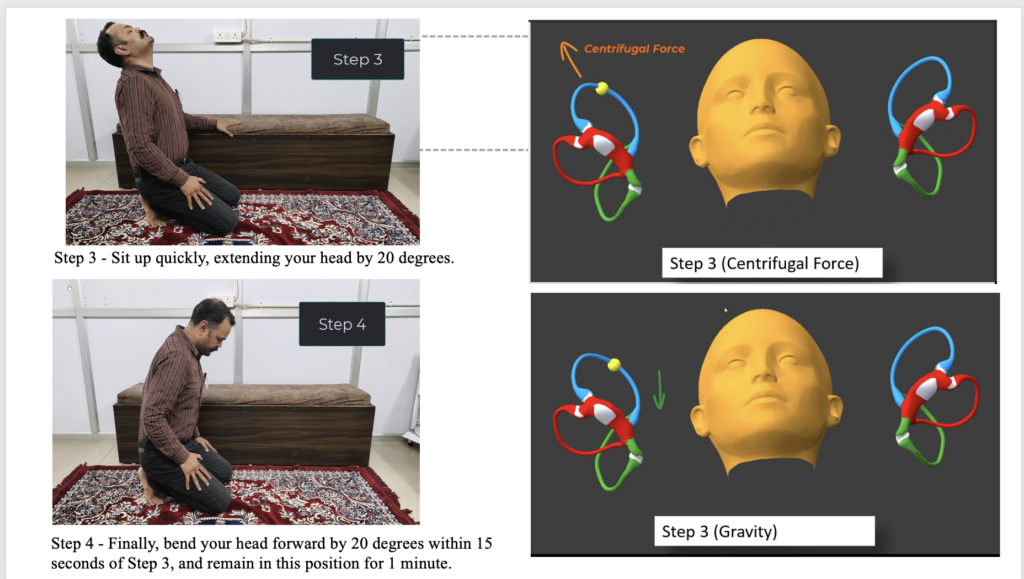
Step 3 — Rapid Sit-Up with 20° Head Extension
This is the most important step — and also the one that requires the most precise timing.
The patient sits up quickly from the forehead-to-floor position, and as they do so, the head is extended back by 20°. The rapid upward movement generates centrifugal force, and because the debris has already crossed the non-ampullary threshold in steps 1 and 2, this force now acts in exactly the right direction — pulling the otoliths toward the common crus and propelling them into the utricle.
Critical timing: Step 3 must not be held for more than 15 seconds. This is non-negotiable. If the head extension is maintained beyond 15 seconds, the anatomy of the posterior canal creates a real risk of the particles inadvertently falling into the non-ampullary end of the posterior canal — which would convert anterior canal BPPV into posterior canal BPPV. We would be trading one problem for another.
So: sit up quickly, head slightly extended, move to Step 4 within 15 seconds.
Step 4 — Head Forward Flexion of 20° for 1 Minute
Immediately after Step 3, within those 15 seconds, the patient bends the head forward by 20° and holds this position for a full minute.
This step does two things. First, it closes off the gravitational path into the posterior canal — acting essentially as a safety lock that prevents the debris from going the wrong way. Second, it gives the mobilized particles enough time to settle fully into the utricle, completing the repositioning.
One minute may feel long to a patient who is dizzy, but it is necessary. I usually talk to the patient during this step to keep them calm.
What to Expect After the Maneuver
Most patients feel a surge of dizziness during Step 3 — this is expected and is actually a good sign that the crystals are moving. I always warn patients beforehand so they’re not alarmed.
After the maneuver, patients should sit quietly for 10-15 minutes before standing. For the rest of that day, I advise avoiding rapid head movements. Sleeping with the head elevated at 30-45° for the first night (two pillows is usually enough) helps prevent any displaced crystals from re-entering the canal.
Most patients are significantly better or completely symptom-free after one session. A small number — maybe 10-15% in my clinical experience — need a repeat session at one week. Before repeating, I always recheck with Dix-Hallpike because sometimes what remains is not residual anterior canal BPPV but a small amount of debris that has converted to another canal — and that requires a different treatment approach.
Who Is This Maneuver For?
Any patient with confirmed anterior canal BPPV is a candidate. Specifically:
Patients with downbeat (or mixed downbeat-torsional) nystagmus on positional testing, after central causes have been properly excluded.
Patients in whom the Yacovino maneuver has failed.
Patients with cervical spine limitations who cannot tolerate deep neck extension.
Patients with suspected larger debris clumps or canal strictures where a pure gravity-based approach may be insufficient.
It should not be attempted without proper diagnostic evaluation. Downbeat nystagmus must never be assumed to be BPPV without first ruling out central pathology — this point cannot be overstated.

Final Note
Anterior canal BPPV is real, it is diagnosable, and it is treatable. The patients who end up on betahistine for months, or who are told their vertigo is psychological, often have a fixable inner ear problem that simply requires the right diagnostic lens and the right maneuver.
The Bangalore Maneuver is our contribution toward filling that gap.
Dr. Prateek Porwal, MBBS, DNB ENT, CAMVD — ENT & Vertigo Specialist, Prime ENT Center, Hardoi, Uttar Pradesh. Originator of the Bangalore Maneuver. Honorary Secretary, NES India 2025-26.
Dr. Prateek Porwal
MBBS, DNB ENT, CAMVD
Vertigo & BPPV Specialist
Prime ENT Center, Nagheta Road, Hardoi, UP 241001
For appointments: Call or WhatsApp 7393062200
This article is for educational purposes only. Please consult Dr. Prateek Porwal at Prime ENT Center, Hardoi or book an online consultation at 7393062200. Website: drprateekporwal.com
