Balance disorders vs. vertigo — Balance disorders vs vertigo — these two terms are often used interchangeably by patients, yet they represent fundamentally different clinical entities. As an ENT and vertigo specialist, the distinction matters enormously: it determines diagnosis, treatment, and outcomes. This detailed guide will walk you through every category of dizziness from classic peripheral vertigo to central neurological causes, medical dizziness, and the feared pre-syncope so you can understand exactly what is happening in your body.
Table of Contents
In my practice in Hardoi, I see these cases regularly. Based on my clinical experience with hundreds of patients, here’s what actually works.
- The 4 Types of Dizziness: A Framework
- Peripheral Vestibular Disorders
- Central Vestibular Disorders
- Medical (Non-Vestibular) Dizziness
- Pre-Syncope and Syncope
- The HINTS Exam: Bedside Stroke vs. Vestibular Neuritis
- Oscillopsia and Skew Deviation Explained
- Peripheral vs. Central: Comparison Table
- Treatment: Peripheral vs. Central
- Vestibular Rehabilitation Therapy (VRT)
- PPPD: The Chronic Dizziness You Didn’t Know About
- Frequently Asked Questions About Balance Disorders Vs Vertigo
Balance Disorders vs Vertigo: The 4 Types of Dizziness
The word “dizziness” is one of the most imprecise complaints in medicine. To properly evaluate balance disorders vs. vertigo, clinicians use the Drachman-Hart classification of four distinct dizziness subtypes. Each category has unique pathophysiology, red flags, and treatment pathways.
| Type | Sensation | Origin | Common Causes |
|---|---|---|---|
| Vertigo | Room spinning, self-spinning | Vestibular (peripheral or central) | BPPV, vestibular neuritis, Meniere’s, stroke |
| Pre-syncope | Lightheadedness, impending faint | Cardiovascular / autonomic | Orthostatic hypotension, POTS, cardiac arrhythmia |
| Disequilibrium | Unsteadiness while walking | Proprioceptive / cerebellar | Neuropathy, cerebellar ataxia, Parkinson’s |
| Non-specific dizziness | Floating, foggy, rocking | Psychosomatic / multifactorial | Anxiety, PPPD, medication side effects |
Understanding which type of dizziness a patient has is the essential first step. A patient with pre-syncope needs a cardiologist; a patient with BPPV needs the Epley maneuver. Confusing the two can be dangerous.
Peripheral Vestibular Disorders: The Inner Ear Causes of Vertigo
Peripheral vestibular disorders originate in the inner ear (labyrinth) or the vestibular nerve (CN VIII). These are the most common causes of vertigo and generally carry a benign prognosis. The three major conditions are BPPV, Vestibular Neuritis, and Meniere’s Disease.

1. Benign Paroxysmal Positional Vertigo (BPPV)
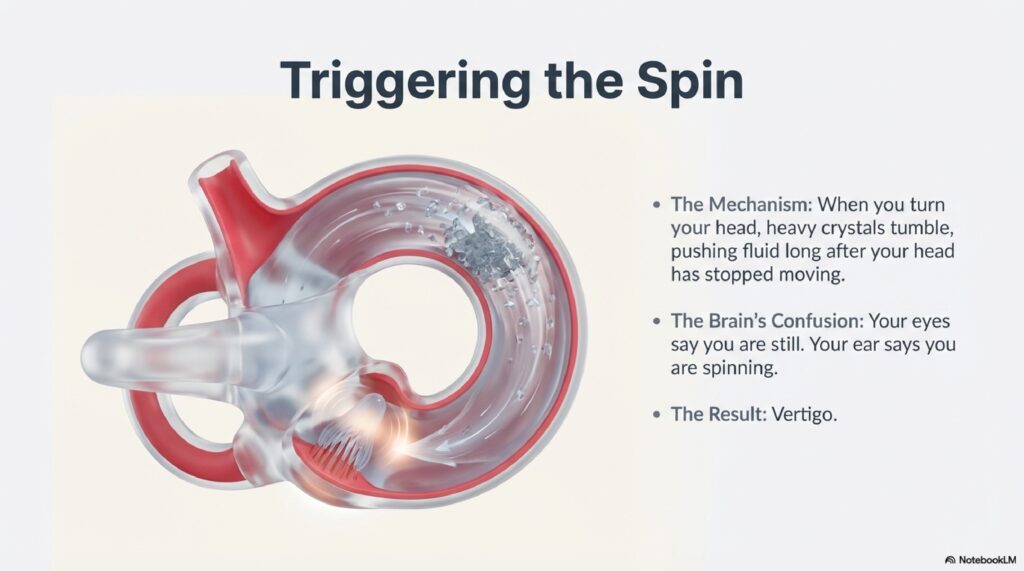
BPPV is the single most common cause of balance disorders vs. vertigo worldwide. It accounts for nearly 20-30% of all dizziness complaints. It occurs when calcium carbonate crystals (otoconia) dislodge from the utricle and enter the semicircular canals most commonly the posterior canal (85-90% of cases).
Key features of BPPV:
- Episodes last less than 60 seconds
- Triggered by head position changes (lying down, rolling over, looking up)
- Positive Dix-Hallpike test with geotropic nystagmus
- No hearing loss, no tinnitus
- Resolves with Epley maneuver (canalith repositioning)
BPPV is a mechanical problem, not a neurological one. It has no relationship to blood pressure, anxiety, or brain pathology. Diagnosis is clinical; no MRI or blood tests are needed in typical presentations.
2. Vestibular Neuritis and Labyrinthitis
Vestibular neuritis is an acute unilateral vestibular loss, typically following a viral upper respiratory illness. It presents as a sudden, severe, constant vertigo lasting days to weeks, with nausea, vomiting, and gait instability. Unlike BPPV, it is NOT positional the vertigo is present even at rest.
Vestibular neuritis vs. labyrinthitis: If hearing loss accompanies the vertigo, it is labyrinthitis (suggesting the cochlea is also affected). Vestibular neuritis affects only the vestibular branch of CN VIII, sparing hearing.
The critical concern with acute vestibular neuritis is distinguishing it from a posterior circulation stroke. This is where the HINTS exam becomes important. A positive Head Impulse Test (abnormal VOR) favors peripheral neuritis; a normal head impulse in the setting of acute vertigo should raise alarm for a central stroke.
3. Meniere’s Disease
Meniere’s disease is caused by endolymphatic hydrops excess fluid pressure in the inner ear. It is characterized by the classic tetrad: episodic vertigo (20 minutes to 12 hours), fluctuating sensorineural hearing loss, tinnitus, and aural fullness.
Meniere’s is distinguishable from BPPV by its longer duration of vertigo episodes, the presence of auditory symptoms, and its progressive nature. Over years, the hearing loss may become permanent. Management includes low-sodium diet, diuretics, betahistine, and in refractory cases, intratympanic gentamicin or endolymphatic sac surgery.
Central Vestibular Disorders: Brain-Origin Vertigo
Central vestibular disorders are caused by pathology within the brainstem or cerebellum the areas that process vestibular signals. Although less common than peripheral causes, central vertigo carries significantly higher morbidity and can be life-threatening. Missing a posterior fossa stroke presenting as vertigo is a known medicolegal hazard.
1. Vestibular Migraine
Vestibular migraine is the most common cause of central vestibular vertigo and is frequently underdiagnosed. According to the Barany Society / IHS criteria, vestibular migraine requires at least 5 episodes of vestibular symptoms (vertigo, positional dizziness, visual vertigo) lasting 5 minutes to 72 hours, with a current or past history of migraine headaches.
Importantly, headache need not be present during the dizzy episode. Many patients present with isolated vertigo and only report headaches when specifically asked. Photophobia, phonophobia, or visual aura during the episode supports the diagnosis. This is the most commonly missed diagnosis in dizzy patients.
2. Posterior Circulation Stroke (Cerebellar / Brainstem)
A cerebellar or brainstem stroke is the most dangerous cause of acute vertigo. It can mimic vestibular neuritis almost perfectly, making the HINTS exam (discussed below) critically important. Warning signs (“HINTS to INFARCT”) that suggest stroke rather than neuritis include:
- Normal head impulse test (intact VOR)
- Direction-changing nystagmus on lateral gaze
- Skew deviation (vertical misalignment of the eyes)
- New neurological deficits: diplopia, dysarthria, dysphagia, ataxia
- Inability to walk (truncal ataxia)
- Headache or neck pain (vertebral artery dissection)
Any patient with acute continuous vertigo who cannot stand or walk unassisted should be urgently evaluated for posterior fossa stroke with MRI (not CT, which misses posterior fossa infarcts in the first 24-48 hours).
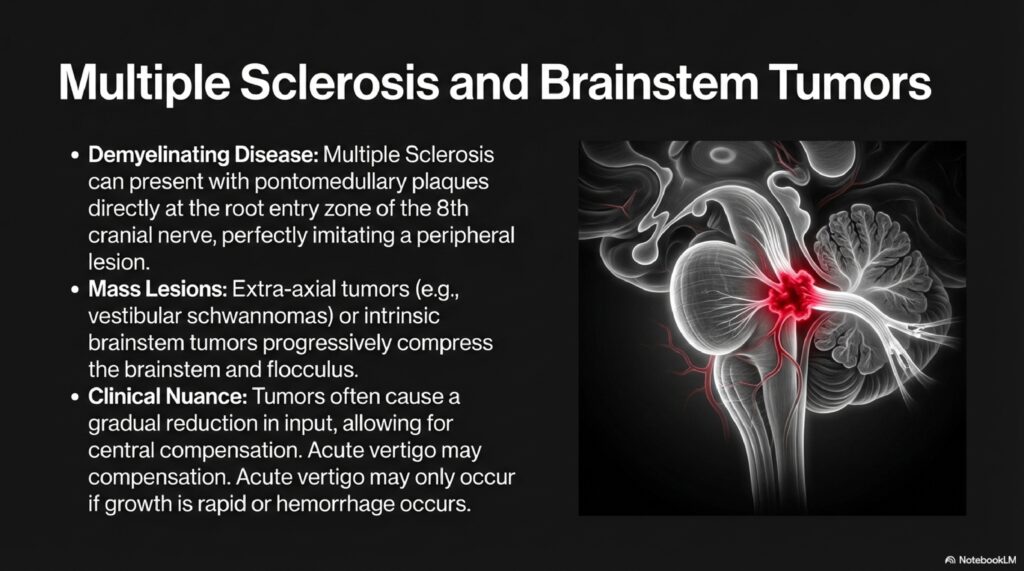
3. Multiple Sclerosis and Demyelinating Disease
MS can present with acute vertigo from demyelinating plaques in the brainstem or cerebellum. Features that raise suspicion include young patients, history of other neurological episodes (optic neuritis, limb weakness), internuclear ophthalmoplegia, and MRI white matter lesions. Pure vertigo as the sole presenting feature of MS is uncommon but documented.
4. Mal de Debarquement Syndrome (MdDS)
MdDS is a central vestibular adaptation disorder where patients feel a persistent rocking, swaying, or bobbing sensation after returning from travel (especially sea voyages or flights). Unlike most dizziness conditions, MdDS is relieved by passive motion (driving or sailing) and worsens at rest. It is more common in middle-aged women and can persist for months to years.
Medical (Non-Vestibular) Dizziness: True Dizziness
Many patients who present complaining of “dizziness” have no vestibular disorder whatsoever. Their symptoms arise from systemic medical conditions that affect cerebral perfusion, blood chemistry, or autonomic regulation. Distinguishing these from vestibular disorders prevents unnecessary vestibular testing and makes sure patients receive appropriate medical workup.
Orthostatic Hypotension
Orthostatic hypotension is defined as a drop in systolic BP of ≥20 mmHg or diastolic BP of ≥10 mmHg within 3 minutes of standing. Patients describe lightheadedness (not true spinning vertigo) upon rising from bed or a chair. Common causes include dehydration, antihypertensive medications, diabetic autonomic neuropathy, and Parkinson’s disease.
Unlike BPPV, this dizziness is positional but teh sensation is not spinning it is a “head rush” or feeling of impending faint. The Romberg test is negative; there is no nystagmus. Diagnosis is confirmed by lying-to-standing blood pressure measurements.
POTS (Postural Orthostatic Tachycardia Syndrome)
POTS is a dysautonomia characterized by a heart rate increase of ≥30 bpm (or HR >120 bpm) within 10 minutes of standing, without significant blood pressure drop. It predominantly affects young women and has become more prevalent following COVID-19. Symptoms include dizziness on standing, palpitations, brain fog, fatigue, and exercise intolerance.
POTS is frequently mistaken for anxiety or vestibular disorders. The tilt-table test is diagnostic. Management includes increased salt and fluid intake, compression garments, beta-blockers, fludrocortisone, and graded exercise programs.
Hypoglycemia and Metabolic Dizziness
Low blood sugar produces dizziness, diaphoresis, tremor, and confusion. Diabetic patients on insulin or sulfonylureas are at particular risk. Hypothyroidism, severe anemia, and electrolyte disturbances (hyponatremia, hypomagnesemia) can all produce dizziness that mimics vestibular disease. A basic metabolic panel and CBC should be part of the initial workup in any new dizziness patient.
Cardiac Arrhythmias and Dizziness
Intermittent cardiac arrhythmias particularly sick sinus syndrome, paroxysmal atrial fibrillation, and complete heart block can produce episodic dizziness or pre-syncope. These episodes may be brief and occur with exertion. A 24-hour Holter monitor or event recorder is essential if cardiac arrhythmia is suspected. Patients over 60 with new-onset dizziness and palpitations require cardiac evaluation before vestibular testing.
Pre-Syncope and Syncope: When Dizziness Means Fainting
Pre-syncope the sensation of impending faint is a distinct category of dizziness that must never be confused with vertigo. The patient typically describes a sudden onset of lightheadedness, dimming of vision (greying out), weakness, and nausea. Actual loss of consciousness (syncope) may follow if cerebral perfusion falls critically low.
Common causes of syncope and pre-syncope:
- Vasovagal syncope: The most common type; triggered by pain, emotion, prolonged standing, heat. Prodromal symptoms (nausea, pallor, diaphoresis) followed by brief LOC with quick recovery.
- Carotid sinus hypersensitivity: Syncope triggered by neck pressure (tight collars, turning head). Common in elderly men.
- Cardiac syncope: Sudden LOC without prodrome; caused by arrhythmias, structural heart disease (aortic stenosis, HCM). High mortality risk requires urgent cardiac workup.
- Orthostatic syncope: Faint on standing; caused by volume depletion, medications, autonomic failure.
- Situational syncope: Micturition, cough, defecation, swallowing-induced; Valsalva mechanism.
The key differentiator: syncopal dizziness is lightheadedness, not spinning. There is no nystagmus, no positional component, and no hearing symptoms. An ECG is mandatory in every syncope patient. A normal ECG does not exclude dangerous arrhythmias; prolonged monitoring may be required.
The HINTS Exam: Balance Disorders vs Vertigo at the Bedside
The HINTS exam (Head Impulse – Nystagmus – Test of Skew) is a three-part bedside examination that has been shown to be more sensitive than early MRI for distinguishing acute vestibular neuritis from posterior circulation stroke. But It should be performed by trained clinicians in every patient with acute constant vertigo.

| HINTS Component | Peripheral (Safe) Finding | Central (Dangerous) Finding |
|---|---|---|
| Head Impulse Test | Abnormal (catch-up saccade) | Normal (intact VOR = DANGER) |
| Nystagmus | Unidirectional, horizontal | Direction-changing, vertical, or torsional |
| Test of Skew | No skew deviation | Skew deviation present (vertical misalignment) |
“HINTS to INFARCT”: A normal head impulse + direction-changing nystagmus + presence of skew deviation = HIGH RISK for stroke. This pattern has a sensitivity of 100% and specificity of 96% for posterior fossa stroke in the appropriate clinical context (Kattah et al., 2009, NEJM).
Oscillopsia and Skew Deviation: Visual Symptoms of Vestibular Disease
Two visual phenomena deserve special attention in vestibular medicine: oscillopsia and skew deviation. Both provide important diagnostic information and can significantly impact quality of life.
Oscillopsia: The World That Won’t Stay Still
Oscillopsia is the illusory movement of the visual environment patients describe the world as “bouncing”, “jumping”, or “oscillating” with head movement or during walking. It occurs when the vestibulo-ocular reflex (VOR) fails to stabilize the retinal image adequately during head motion. Causes include bilateral vestibular loss (ototoxicity, autoimmune), superior canal dehiscence, and cerebellar degeneration.
Oscillopsia is a major cause of disability patients cannot read while moving, cannot drive, and may be unable to identify faces. It is distinct from vertigo (no spinning sensation) and represents a failure of the VOR gaze-stabilization mechanism.
Skew Deviation: A Critical Sign of Central Disease
Skew deviation is a vertical misalignment of the eyes (one eye higher than the other) caused by asymmetric input to the vertical eye movement pathways. It is a supranuclear ocular motor disturbance. In the context of the HINTS exam, skew deviation strongly suggests central pathology specifically posterior fossa stroke or demyelinating disease affecting the brainstem.
Skew deviation is tested with the alternate cover test: the examiner alternately covers each eye while watching for vertical refixation movements. If the uncovered eye drifts down and must refixate upward, skew deviation is present. It can appear as a subtle finding but carries enormous diagnostic weight its presence essentially rules out peripheral vestibular neuritis and mandates urgent neuroimaging.
Watch: Skew deviation examination technique
Peripheral vs. Central Vertigo: The Complete Comparison
The following table summarizes the key differences between peripheral and central balance disorders vs. vertigo. This is the most clinically useful reference for differentiating the two categories at the bedside.
| Feature | Peripheral Vertigo | Central Vertigo |
|---|---|---|
| Onset | Sudden (BPPV) or subacute (neuritis) | Sudden (stroke) or gradual (tumor) |
| Severity | Often intense | Variable, may be mild |
| Nausea/Vomiting | Severe | Mild to moderate |
| Nystagmus direction | Unidirectional, horizontal/torsional | Direction-changing, vertical, or purely torsional |
| Nystagmus fixation | Suppressed by visual fixation | NOT suppressed (or worsened) by fixation |
| Head impulse test | Abnormal (positive catch-up saccade) | Normal (DANGER sign) |
| Skew deviation | Absent | Present (suggests central) |
| Hearing loss | May be present (Meniere’s, labyrinthitis) | Usually absent (except AICA infarct) |
| Neurological signs | Absent | Present (diplopia, dysphagia, dysarthria) |
| Gait | Can walk (leans toward affected side) | Cannot walk independently (truncal ataxia) |
| MRI findings | Usually normal | Stroke, tumor, MS plaques |
| Prognosis | Excellent, resolves in days-weeks | Depends on cause; stroke = urgent |
Treatment of Balance Disorders vs. Vertigo
Treatment differs fundamentally based on the underlying diagnosis. There is no universal “vertigo medication” the right treatment depends on whether the cause is peripheral, central, or medical.
| Condition | First-Line Treatment | Specialist |
|---|---|---|
| BPPV | Epley maneuver (canalith repositioning) | ENT / Vestibular specialist |
| Vestibular Neuritis | Oral steroids, vestibular rehab | ENT / Neurologist |
| Meniere’s Disease | Low-sodium diet, betahistine, diuretics | ENT / Audiologist |
| Vestibular Migraine | SSRI, lifestyle modification | Neurologist |
| Posterior Fossa Stroke | Thrombolysis / thrombectomy (acute), antiplatelet (secondary prevention) | Neurologist (URGENT) |
| POTS | Salt/fluid loading, beta-blockers | Cardiologist / Autonomic specialist |
| PPPD | SSRIs, vestibular rehab, CBT | Psychiatry + Vestibular specialist |
Vestibular Rehabilitation Therapy (VRT): Retraining the Balance System
Vestibular Rehabilitation Therapy (VRT) is an evidence-based exercise-based program designed to reduce dizziness, improve gaze stability, and restore balance. It works by promoting central compensation the brain learns to reinterpret abnormal vestibular signals and substitute visual and proprioceptive inputs.
VRT is indicated for most chronic vestibular disorders including uncompensated vestibular neuritis, bilateral vestibular loss, oscillopsia, PPPD, and residual dizziness after successful BPPV treatment. It is NOT indicated as primary treatment for active BPPV (Epley maneuver is preferred) or for active Meniere’s hydrops episodes.
Key VRT exercise categories include:
- Gaze stabilization exercises: VOR x1 and x2 exercises to improve visual acuity during head movement
- Habituation exercises: Repeated exposure to provocative movements to reduce symptomatic response
- Balance training: Progressively challenging static and dynamic balance tasks
- Gait training: Walking with head turns, obstacles, and varied surfaces
PPPD: Persistent Postural-Perceptual Dizziness
PPPD (Persistent Postural-Perceptual Dizziness) is the most common chronic vestibular disorder in adults, yet it remains severely underdiagnosed. It is a functional vestibular disorder meaning there is no structural pathology, but the brain’s processing of vestibular and balance signals is aberrant.
Diagnostic criteria (Barany Society, 2017):
- Dizziness, unsteadiness, or non-spinning vertigo for ≥3 months
- Symptoms present on most days
- Exacerbated by upright posture, active/passive motion, and visually complex environments
- Precipitated by an acute vestibular event, balance disorder, or psychological stressor
- Not explained by another active disease
PPPD frequently develops after an acute peripheral event (BPPV, neuritis) when the brain fails to fully compensate and instead develops a maladaptive high-gain threat-detection pattern. Treatment requires SSRIs/SNRIs, vestibular rehabilitation emphasizing exposure-based therapy, and cognitive behavioral therapy (CBT) addressing avoidance behaviors.

Frequently Asked Questions About Balance Disorders vs. Vertigo
Is vertigo the same as a balance disorder?
No. Vertigo is the specific sensation of spinning, and it is one type of balance disorder. Balance disorders include all conditions that affect equilibrium vestibular, neurological, cardiovascular, and metabolic. Vertigo is a symptom; balance disorder is the broader category. A patient can have a balance disorder vs. vertigo distinction: they may have unsteadiness (a balance disorder) without any spinning (vertigo).
When should I be worried about my dizziness?
Seek urgent medical attention if your dizziness is accompanied by: sudden headache (worst of life), double vision, slurred speech, facial numbness, arm or leg weakness, inability to walk, or new hearing loss. These are red flags for a possible stroke or serious neurological emergency.
Can anxiety cause balance disorders?
Yes. Anxiety can directly cause dizziness through hyperventilation and can also trigger PPPD in predisposed individuals. Conversely, vestibular disorders frequently cause secondary anxiety because the unpredictability of episodes is distressing. The two conditions reinforce each other, which is why PPPD treatment addresses both the vestibular and psychological components.
What is the difference between central and peripheral vertigo?
Peripheral vertigo originates in the inner ear or vestibular nerve; it is usually intense, with severe nausea, but is benign and self-limiting. Central vertigo originates in the brainstem or cerebellum; it may be milder in intensity but is associated with neurological signs and can indicate a stroke or tumor. The HINTS exam is the key bedside tool to differentiate them in acute presentations.
How long does vestibular neuritis last?
The acute severe phase of vestibular neuritis typically lasts 3-5 days. Nausea and vomiting resolve within a week. Mild dizziness and imbalance can persist for weeks to months during the compensation phase. With adequate vestibular rehabilitation, most patients achieve full functional recovery within 3 months, though some residual sensitivity may persist longer.
Dr. Prateek Porwal is an ENT and Vestibular Disorders Specialist at Prime ENT Center. For evaluation of dizziness and balance disorders, book a consultation at our center.
Key Takeaways: Balance Disorders vs. Vertigo
Understanding the distinction between balance disorders vs. vertigo is foundational to correct diagnosis and treatment. Here are the essential points every patient and clinician should know about balance disorders vs. vertigo:
- Balance disorders vs. vertigo is not a single diagnosis it is a framework that covers peripheral vestibular, central neurological, and medical systemic causes.
- BPPV is the most treatable cause of balance disorders vs. vertigo and responds to the Epley maneuver in most cases.
- A normal head impulse test in a patient with acute vertigo should prompt urgent stroke evaluation.
- Syncope and pre-syncope are cardiovascular not vestibular emergencies and must be evaluated with ECG.
- PPPD represents the chronic, functional end of the balance disorders vs. vertigo spectrum and requires multimodal treatment.
- Oscillopsia and skew deviation are signs of VOR failure and central pathology respectively.
References and Further Reading
For those seeking to learn more about balance disorders vs. vertigo, the following authoritative resources are recommended:
- NIDCD: Balance Disorders National Institute on Deafness and Other Communication Disorders
- Vestibular Disorders Association (VEDA) Types of Vestibular Disorders
- Kattah JC et al. HINTS to Diagnose Stroke in the Acute Vestibular Syndrome. Stroke. 2009
About the Author — Balance Disorders Vs Vertigo Specialist
Dr. Prateek Porwal is an ENT & Vertigo Specialist with over 13 years of experience, holding MBBS (GSVM Medical College), DNB ENT (Tata Main Hospital), and CAMVD (Yenepoya University). He is the originator of the Bangalore Maneuver for Anterior Canal BPPV and has published research in Frontiers in Neurology and IJOHNS. Serving at Prime ENT Center, Hardoi.
Disclaimer: This article is for educational purposes only. Please consult Dr. Prateek Porwal or a qualified ENT specialist for personal medical advice. Always seek professional diagnosis before starting any treatment.

