When I first saw Rajesh, a 42-year-old businessman from Lucknow, he had been suffering for five years without a proper diagnosis. He would have sudden, violent spinning episodes that lasted anywhere from two hours to half a day, leaving him unable to work or even stand. Between attacks, he heard a constant roaring sound in his left ear, and felt pressure building up inside it. His hearing kept getting worse. He’d been told it was stress, nerve problems, high blood pressure-anything except what it actually was: Meniere’s disease. This post covers meniere’s disease in detail.
I see this pattern often in my ENT clinic here in Hardoi. Meniere’s disease is poorly understood, frequently misdiagnosed, and causes tremendous disruption to patients’ lives. Today I want to explain what it is, how to recognize it, and what we can do about it.
What is Meniere’s Disease?: Menieres Disease Guide
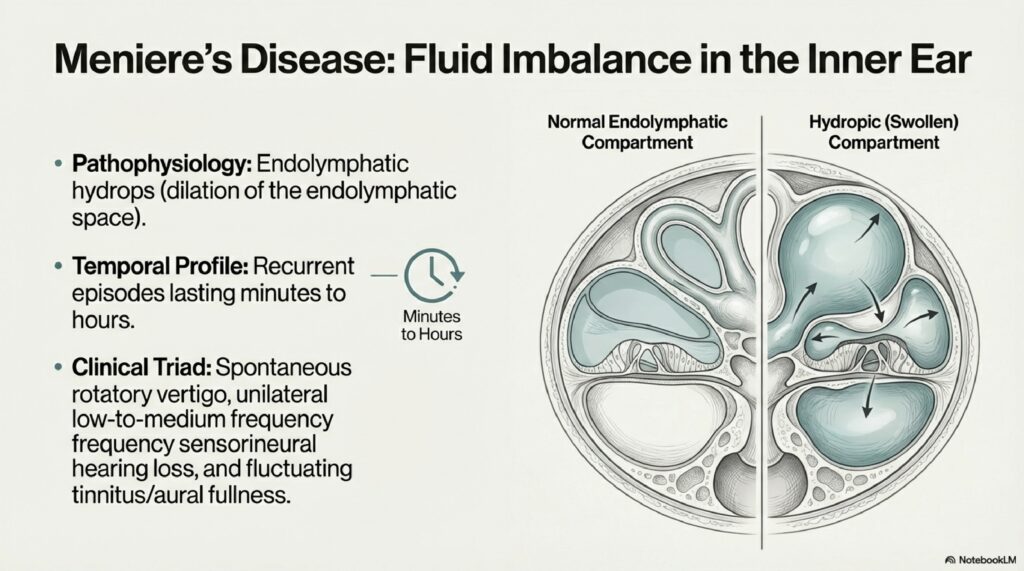
At its core, Meniere’s disease is a disorder of the inner ear caused by abnormal accumulation of fluid called endolymph. This fluid normally sits in delicate chambers inside your inner ear that control balance and hearing. When too much fluid builds up-a condition called endolymphatic hydrops-it puts pressure on these sensitive structures and causes symptoms.
Think of it like a water balloon that’s overfilled. When pressure spikes, it distorts everything inside. That distortion is what causes the symptoms.
Why does the fluid accumulate? We don’t know exactly. Some experts think it’s a problem with how the ear drains fluid. Others suggest it could be triggered by infection, immune problems, genetics, or even viral infections. Most likely, it’s a combination of factors in each patient.
The Four Classic Symptoms (The Tetrad)
Meniere’s disease presents with what we call a “tetrad” of symptoms that occur together:
1. Vertigo Attacks
The vertigo in Meniere’s is severe and sudden. It’s not mild dizziness-it’s the room spinning violently, often accompanied by intense nausea and vomiting. Attacks last anywhere from 20 minutes to 12 hours, sometimes longer. During a bad attack, patients can’t stand, can’t walk, can’t even open their eyes without severe dizziness. This is very different from BPPV (Benign Paroxysmal Positional Vertigo), where attacks last seconds to minutes when you move your head.
2. Fluctuating Hearing Loss
The hearing loss in Meniere’s starts with lower frequencies. Patients often notice they can’t hear deep voices or bass sounds clearly. Importantly, the hearing loss fluctuates-it gets worse during or just before an attack, and partially recovers afterward. Over years, if untreated, the hearing loss becomes permanent and progresses to higher frequencies.
3. Tinnitus
Most patients with Meniere’s hear a constant roaring, rushing, or ocean-wave sound in the affected ear. Unlike the high-pitched “ee-ee-ee” tinnitus you might hear after noise exposure, Meniere’s tinnitus is usually low-pitched, like a low rumble or roar. It often changes during attacks.
4. Aural Fullness
Patients describe a feeling of fullness, pressure, or blockage in the affected ear-as if the ear is “full of cotton” or about to pop. This sensation often precedes an attack and can last for hours or days. It’s one of the earliest symptoms many people notice.
To diagnose Meniere’s disease, the patient must have attacks of vertigo lasting 20 minutes to 12 hours, plus at least two of these symptoms: hearing loss documented on audiogram, tinnitus, and aural fullness. This is according to the American Academy of Otolaryngology (AAO-HNS) diagnostic criteria, which I follow in my practice.
👉 Also read: Low Sodium Diet Meniere India
Early, Middle, and Late Stage Disease
Meniere’s disease progresses through stages over years, though not every patient follows this pattern exactly:
Early Stage: Episodic attacks of severe vertigo with full recovery between attacks. Hearing usually recovers between attacks. Attacks might be once a month to once every few months. Many patients function relatively normally between episodes.
Middle Stage: Attacks become more frequent (weekly or multiple times per week). Hearing loss increases and doesn’t fully recover between attacks. Patients start experiencing constant tinnitus and aural fullness even between vertigo attacks. Quality of life significantly declines-they might lose their job or stop driving.
Late Stage: Attacks may become less frequent or even stop, but the damage is done. The patient is left with permanent hearing loss, chronic tinnitus, and persistent balance problems. About 30% of patients develop bilateral Meniere’s disease (both ears affected), which is particularly devastating.
How We Diagnose Meniere’s Disease
Diagnosis is primarily based on your history and symptoms. But we use several tests to confirm it:
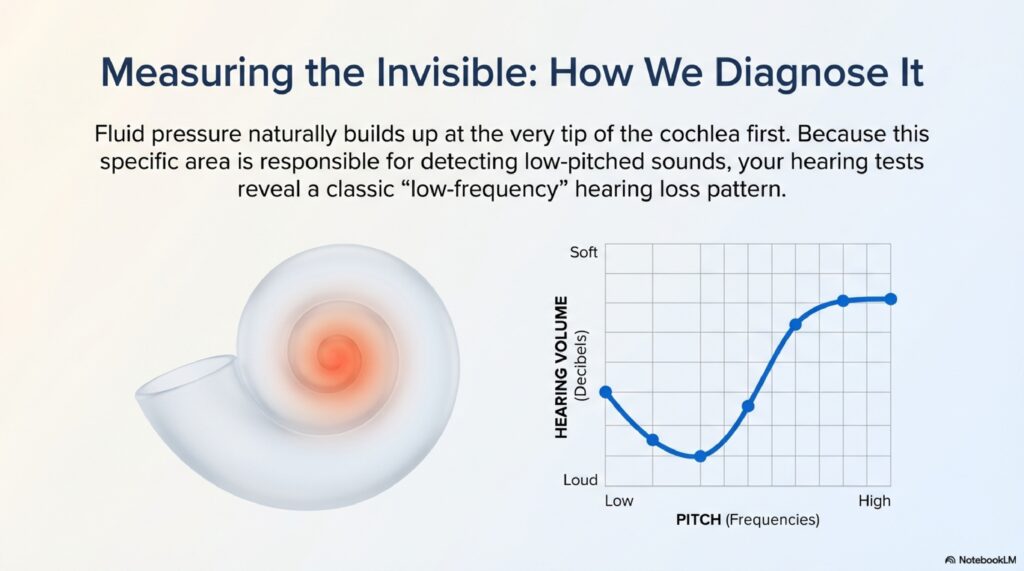
Pure Tone Audiogram: This hearing test shows a characteristic pattern-sensorineural hearing loss affecting low frequencies first. In early disease, the audiogram might be normal between attacks, but as disease progresses, the loss becomes permanent.
Electrocochleography (ECochG): This is a specialized test that measures electrical activity in the inner ear. An abnormally high ratio suggests endolymphatic hydrops. This is often positive in Meniere’s disease and helps confirm the diagnosis.
MRI with Delayed Gadolinium: Modern imaging can actually visualize the swollen endolymphatic sac. This test is increasingly used to confirm Meniere’s disease, especially when diagnosis is unclear.
Caloric Test: This tests how your vestibular system responds to warm and cold water. In Meniere’s, we might see reduced response on the affected side during attack or progressive changes over time.
Video Head Impulse Test (VHIT): This tests your eye reflexes during head movement. It’s good for detecting vestibular dysfunction.
👉 Also read: Electrocochleography Meniere
Importantly, MRI is also done to rule out other conditions like acoustic neuroma or multiple sclerosis that can mimic Meniere’s disease.
Treatment: The Ladder Approach
We treat Meniere’s disease using a step-by-step approach, starting conservative and moving to more aggressive options only if needed:
Step 1: Dietary Management
The single most important thing any patient can do is reduce sodium intake. A low-sodium diet reduces fluid buildup in the inner ear. I recommend limiting sodium to less than 1,500mg per day — though for severe cases, some patients go to 1,000mg or lower. This means avoiding namkeen, papad, achar (pickle), salty snacks, restaurant food, and processed foods.
Other dietary modifications: limit caffeine and alcohol, stay well hydrated, maintain regular meals. Some patients report improvement with a low-sugar diet, though evidence is weaker.
In my experience, about 30% of mild-to-moderate Meniere’s cases improve significantly with diet alone. Rajesh reduced his attacks from 2-3 per week to 1-2 per month just by cutting salt and sticking to home-cooked meals.
Step 2: Diuretics
If diet alone doesn’t work, I add a diuretic medication, typically a thiazide diuretic or a potassium-sparing diuretic medication. These pills reduce fluid volume in the body and decrease pressure in the inner ear. Combined with low-sodium diet, about 60-70% of patients get improvement.
Step 3: Vestibular Suppressants
For acute attacks, medications like vestibular suppressants help control nausea and vomiting. But here’s important: long-term use of vestibular suppressants like betahistine is not recommended. Some patients feel it helps; studies show modest benefit at best.

Step 4: Betahistine
Betahistine is sometimes prescribed as it may improve microcirculation in the inner ear. I use it in some patients, though international evidence of its effectiveness varies. In India, it’s widely prescribed but its not my 1st preference.
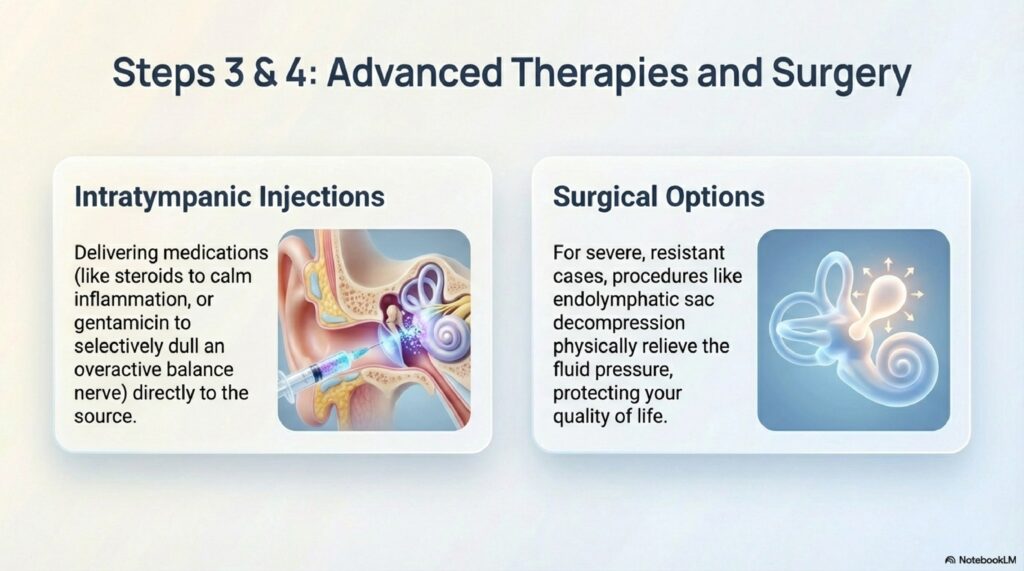
Step 5: Intratympanic Steroids
When oral medications fail, I consider injecting steroid medication directly through the eardrum into the middle ear space. This delivers high-dose anti-inflammatory medication directly to the inner ear. The procedure takes about 10 minutes under local anesthesia. I do a series of 3-4 injections over weeks. Success This is my preferred next step for intractable Meniere’s.
Step 6: Intratympanic Gentamicin
If steroids don’t work, gentamicin can be injected into the middle ear. This is a “chemical labyrinthectomy”-it essentially destroys the diseased vestibular function on that side. Vertigo control is excellent (70-80%), but there’s a 5-15% risk of hearing loss even though we’re trying to save it. This is reserved for patients with intractable disease and acceptable hearing loss risk.
👉 Also read: Meniere Disease Symptoms
Step 7: Surgery
If everything else fails, surgery is an option. Endolymphatic sac decompression surgery improves symptoms in some patients. Labyrinthectomy completely removes balance function from the affected ear but reliably stops vertigo (though hearing is already usually lost by this stage). Vestibular neurectomy is another option where we cut the balance nerve while preserving hearing.
Less commonly, patients with advanced disease and poor hearing might benefit from cochlear implant, which helps both hearing and balance.
What Triggers Meniere’s Attacks — And Can We Prevent Them?
This is one of the first questions every patient asks me after diagnosis: “Doctor, why does it happen? Is there something I’m doing wrong?” The honest answer is — we can’t always predict an attack. But over years of treating hundreds of Meniere’s patients in my clinic, I’ve noticed clear patterns. Triggers vary from person to person, but some are remarkably consistent.
High salt intake is the single most common trigger I see in North Indian patients. A wedding, a festival, three days of eating restaurant food — and suddenly attacks spike. The mechanism is straightforward: excess sodium causes fluid retention, and in a Meniere’s ear, any increase in fluid pressure can tip the balance (literally).
Stress and emotional upheaval are next on the list. I had a patient — a school principal from Sitapur — who went years with controlled Meniere’s. Then her husband had a sudden health crisis. Within two weeks she was having attacks daily. The connection between psychological stress and vestibular function is well documented and, in my observation, very real.
Sleep deprivation matters more than most people realise. When patients tell me their attacks are clustering, I always ask about sleep. More often than not, they’ve been sleeping poorly — late nights, interrupted sleep, irregular schedules. The body’s fluid regulation is tightly linked to circadian rhythm. Disrupting sleep disrupts the inner ear.
Weather changes and barometric pressure fluctuations — a number of my patients report increased symptoms before rain, storms, or when they travel to higher altitudes. The inner ear in Meniere’s disease behaves like a very sensitive barometer, and sudden pressure changes can provoke attacks in susceptible individuals.
Caffeine and alcohol both act as triggers in a subset of patients. Caffeine affects inner ear blood flow; alcohol directly alters the composition of endolymph fluid. I don’t tell every patient to completely eliminate chai — that would be unrealistic in UP — but I do recommend reducing to one small cup a day and avoiding strong coffee, energy drinks, and any alcohol during active phases.
Infections and systemic illness — even a common cold, viral fever, or sinusitis can set off a cluster of Meniere’s attacks. The inner ear is very sensitive to systemic inflammation. During monsoon season particularly, I see a spike in vertigo presentations among my Meniere’s patients.
The good news: by tracking triggers in a diary and making conscious lifestyle modifications, many patients significantly reduce attack frequency without any medication change. I strongly encourage every patient to maintain a simple attack diary — noting date, time, severity, what they ate, their stress level, and how they slept the previous night. Patterns often emerge within six to eight weeks, and that information helps me adjust treatment in a targeted way.
Meniere’s Disease vs. Other Vertigo Conditions — How to Tell the Difference
One of the most common situations I encounter in clinic is patients who’ve been labelled with “vertigo” as a general catch-all diagnosis — no specification of type, no proper workup, and often months or years of inappropriate treatment. This matters enormously because treatment differs completely depending on the underlying cause. Let me walk you through how Meniere’s compares to other common vestibular conditions.
Meniere’s vs. BPPV (Benign Paroxysmal Positional Vertigo): BPPV is the most common cause of vertigo overall, and I see dozens of cases every month. The key distinguishing features are duration and triggering factor. BPPV attacks last seconds — typically 20 to 40 seconds — and are triggered by specific head movements: turning over in bed, looking up to reach a shelf, bending forward. There is no hearing loss, no tinnitus, no ear fullness in BPPV. And importantly, BPPV is correctable with the Epley manoeuvre in most cases, often within one or two clinic visits. If someone has been doing Epley manoeuvres for years without lasting relief, and they also have ear symptoms — they probably do not have BPPV. Meniere’s must be considered.
Meniere’s vs. Vestibular Migraine: This is the trickiest distinction in my day-to-day practice. Vestibular migraine causes episodic vertigo that can last anywhere from minutes to 72 hours — overlapping significantly with Meniere’s. A history of migraine headaches, visual aura, light and sound sensitivity during attacks, and a family history of migraine help point towards vestibular migraine. Critically, significant cochlear symptoms — documented hearing loss, prominent tinnitus, aural fullness — are usually absent in vestibular migraine. ECochG testing helps distinguish between the two. Sometimes both conditions coexist in the same patient, which makes management genuinely complex.
Meniere’s vs. Acoustic Neuroma: Acoustic neuroma is a benign tumour of the vestibular nerve that can cause unilateral hearing loss, tinnitus, and balance problems — mimicking Meniere’s disease quite closely. The vertigo in acoustic neuroma tends to be a chronic imbalance rather than discrete spinning attacks. MRI with gadolinium contrast is definitive — it immediately rules this in or out, which is why I always perform MRI in any atypical or diagnostically uncertain case.
Meniere’s vs. Autoimmune Inner Ear Disease (AIED): AIED can present almost identically to Meniere’s but typically progresses faster, frequently affects both ears early in the course, and responds dramatically to high-dose corticosteroids. If a patient has rapid bilateral sensorineural hearing loss along with vestibular symptoms, I always investigate for autoimmune markers before settling on a Meniere’s diagnosis.
The bottom line is simple: if you’ve been told you have vertigo but haven’t had a proper audiogram, ECochG, MRI, and a detailed history taken by an ENT specialist — there is a real possibility that your diagnosis is incomplete. Please seek specialist evaluation. Getting the right diagnosis is the foundation of getting the right treatment.
👉 Also read: Meniere Disease Symptoms
Vestibular Rehabilitation Therapy: The Underused Treatment Option
I will be direct here: vestibular rehabilitation therapy (VRT) is one of the most underutilised treatments for Meniere’s disease in India. The vast majority of patients who come to me have received only medications. Almost none have been referred for vestibular physiotherapy. This is a significant gap in care that I try to address in my practice.
VRT is a specialised form of physiotherapy designed to retrain the brain to compensate for inner ear dysfunction. It doesn’t cure Meniere’s — nothing currently does — but it substantially reduces the day-to-day imbalance, the “foggy” or “off” feeling many patients experience between acute attacks. It also significantly reduces the risk of falls, which is a serious concern, particularly in elderly patients and in those with late-stage disease and chronic balance impairment.
This also applies to seniors and older adults who may face similar symptoms.
A typical VRT programme involves gaze stabilisation exercises — training the patient to maintain visual focus while moving the head — which is impaired in vestibular dysfunction. It also involves habituation exercises, which gradually expose the patient to movements that provoke mild dizziness, training the brain to stop overreacting to vestibular input. And balance retraining exercises that work on postural stability and core strength.
One important clinical nuance: VRT is most effective during the stable phase of Meniere’s, not during periods of active frequent attacks. Attempting VRT when attacks are occurring multiple times a week can actually worsen symptoms. So timing is critical — I typically refer patients for VRT only after attack frequency has been substantially reduced through medical treatment.
In Lucknow and larger cities in UP, there are now physiotherapists with specific training in vestibular rehabilitation. For patients in smaller towns or rural areas, I can guide basic home exercises that provide meaningful benefit, and online supervised programmes have also become more available.

Meniere’s Disease and Mental Health: The Conversation We Must Have
I address this in every Meniere’s consultation, because it is consistently underdiagnosed and undertreated — and because it directly impacts the physical disease course.
Living with Meniere’s disease is psychologically exhausting in a very specific way. It’s not just the attacks themselves — it’s the relentless uncertainty. A patient of mine, a 38-year-old teacher from Unnao, described it perfectly: “Doctor, I can cope with the attacks when they happen. It’s the not knowing when the next one is coming that has broken me.” She had stopped attending school functions, stopped cooking because of fear of falling near the stove, and hadn’t driven in two years. She had completely reorganised her life around a disease that only affected her intermittently — but the anticipatory anxiety was constant.
Research consistently shows anxiety disorders in 60-80% of Meniere’s patients. Depression rates are also significantly elevated. And importantly, anxiety itself becomes a physiological trigger for attacks — fear generates stress hormones, stress hormones affect inner ear fluid dynamics, which can provoke the very attack the patient was dreading. This creates a vicious cycle that is very difficult to break with medication alone.
I routinely screen all Meniere’s patients for anxiety and depression. When symptoms are clinically significant, I involve a psychiatrist or clinical psychologist as part of the treatment team. Cognitive behavioural therapy (CBT) has reasonable evidence for reducing Meniere’s-related anxiety and improving quality of life. In some patients, appropriate low-dose anxiolytic or antidepressant medication makes a meaningful difference to overall functioning and even to attack frequency.
Diaphragmatic breathing during the prodrome — the ear fullness or warning sensation that often precedes an attack — can reduce attack severity in a subset of patients. I teach this in clinic. It costs nothing and has no side effects.
To family members reading this: your person with Meniere’s is not exaggerating. The fear is rational — they have experienced genuinely terrifying attacks. Your practical support at home, particularly with dietary management and accompanying them to appointments, makes a measurable clinical difference in outcomes.
Living with Meniere’s in India: Practical Guidance for Daily Life
Standard international guidelines are written for a Western context and lifestyle. Here is what I actually tell my patients in UP and surrounding areas — practical, realistic guidance for Indian daily life.
Salt in the Indian kitchen: Our cuisine is inherently high in sodium, and this is the biggest challenge for Meniere’s patients in India. I encourage families to transition the whole household to low-salt cooking rather than making separate food for the patient — this is both practical and avoids the patient feeling singled out. Namkeen, papad, achar, processed masalas, and readymade snacks need to go. Use lemon juice, amchur, jeera, ajwain, fresh coriander, and ginger for flavour instead of salt. Plain curd, cucumber raita without salt, and coconut water (in moderation) are good snack options.
Managing an attack safely at home: I advise patients to identify a “safe space” — ideally a mattress or low bed close to the floor where they can lie down immediately when an attack begins. Keep a bucket nearby for nausea. Have the prescribed emergency medication — usually an anti-nausea suppository or dissolvable tablet — in a consistent, easy-to-reach location. Alert a family member or neighbour if you feel the prodrome symptoms. Never attempt to walk to another room or climb stairs during an active spinning attack. Stay still, lie down, close your eyes if that helps, and let the attack pass.
Driving: I need to be unambiguous here. If you are having active, uncontrolled Meniere’s attacks, you must not drive. A vertigo attack can come on suddenly and completely incapacitate you within seconds — this is an accident waiting to happen. Once your disease is controlled and you have been reliably attack-free for a sustained period, we can reassess driving. Until then, please arrange alternative transport.
Occupation and work: For desk-based or sedentary work, controlled Meniere’s usually allows continued employment with appropriate accommodations. For work involving operating machinery, working at height, driving vehicles, or physical labour in unsafe environments — individual assessment is essential. I write formal medical letters for employers and for occupational health purposes when needed.
Air and train travel: Travel is possible with careful planning. Aircraft cabin pressure changes can trigger attacks — I advise patients to fly only during stable phases, carry emergency medication in hand luggage, stay hydrated, and avoid the salty snacks airlines provide. Train travel is generally more tolerable than air travel for patients with active disease, and often a better option for distances within UP and neighbouring states.
Monitoring your own hearing: I ask all Meniere’s patients to do a simple daily self-check — cover one ear at a time and listen to a set sound at a fixed distance. Any sudden significant worsening of hearing in the affected ear should prompt an immediate clinic visit, as early intratympanic steroid intervention within the first 48-72 hours can significantly improve the chances of hearing recovery.
When Should You See an ENT or Vertigo Specialist?
If you have episodes of vertigo lasting more than 20 minutes, accompanied by ear fullness, roaring tinnitus, or fluctuating hearing — you should see an ENT specialist. Not just a general physician. Not just a neurologist. An ENT with specific interest in vestibular disorders, who can arrange audiogram, ECochG, and VHIT testing. Without these tests, a proper Meniere’s workup is incomplete.
Seek urgent specialist care if you notice: sudden severe hearing loss in one ear — this is a medical emergency where the treatment window is 48-72 hours; vertigo lasting more than 24 hours without improvement; new neurological symptoms alongside vertigo such as double vision, slurred speech, difficulty swallowing, or limb weakness — these warrant immediate emergency evaluation to rule out stroke; or if you have fallen and sustained a significant injury during an attack.
For patients already diagnosed with Meniere’s, come in for review if: attack frequency or severity increases despite current treatment, you notice progressive hearing deterioration in the affected ear, you begin noticing symptoms in the second ear, you are struggling significantly with anxiety or depression related to the disease, or you are considering stopping or changing your medications.
I see Meniere’s patients from across Uttar Pradesh — Lucknow, Kanpur, Lakhimpur Kheri, Unnao, Sitapur, Shahjahanpur, Hardoi district. For patients who cannot travel, teleconsultation is available. I review audiograms and clinical history remotely and then direct patients for in-person testing when needed.
New and Emerging Treatments for Meniere’s Disease
Meniere’s disease research has advanced considerably over the past decade, and I want to give you an honest assessment of what’s available now versus what may be coming.
Endolymphatic Hydrops MRI: The ability to directly visualise endolymphatic hydrops on delayed gadolinium-enhanced MRI has been genuinely changes things for diagnosis. We can now confirm Meniere’s with imaging in uncertain cases — something that wasn’t possible ten years ago. This has reduced misdiagnosis rates in centres with access to this protocol. More specialist centres in India are beginning to offer this.
Improved Intratympanic Drug Delivery: We are getting better at targeted inner ear treatment. Ongoing research into sustained-release intratympanic drug delivery systems — where a single injection provides a slow release of medication over weeks — could dramatically improve convenience and efficacy compared to the current series of multiple injections.
Biological and Immunological Therapies: A growing body of research suggests that a subset of Meniere’s patients have an autoimmune or inflammatory component. Biologics targeting specific inflammatory pathways are being investigated. This is still at the research and early clinical trial stage, but it represents a potentially important shift in how we understand and treat a proportion of Meniere’s cases.
Vestibular Implants: For patients with end-stage bilateral Meniere’s disease who have lost most vestibular function bilaterally, vestibular implants — conceptually similar to cochlear implants but targeting the balance system — are in clinical trials in Europe and the USA. These could be changes things for the most severely affected patients within the next decade.
For now, in my day-to-day practice, the most impactful practical advances are: better diagnostic accuracy through ECochG and MRI protocols, more proactive use of intratympanic steroids as first-line interventional therapy before resorting to destructive procedures, and much greater recognition of the mental health dimension of this disease. These advances, applied consistently, are already meaningfully improving outcomes for my patients.
Bilateral Meniere’s Disease
About 30% of patients eventually develop Meniere’s disease in the second ear. This is particularly difficult-bilateral disease is much harder to manage because we can’t rely on one healthy ear for balance. Some patients progress within months; others take years. If you’ve been diagnosed with unilateral Meniere’s, be watchful for symptoms in the opposite ear.
Quality of Life Impact
I want to be honest about the emotional and practical toll. Patients with uncontrolled Meniere’s often can’t drive safely. They might lose their jobs. Unpredictable attacks create anxiety and depression. Social life suffers because they can’t attend events or travel. In India, particularly in UP, where many families depend on one earning member, Meniere’s can be economically devastating.
But with proper management-diet, medications, and when needed, intratympanic treatments-most patients get their lives back. It requires patience and persistence, but improvement is absolutely possible.
Rajesh’s Outcome
I’m pleased to report that Rajesh responded excellently to conservative management. His wife learned to cook low-salt meals (she actually became quite creative with lemon, ginger, and herbs for flavoring). He started on diuretic. Within three months, his attacks dropped to once every 2-3 weeks. Within six months, they were rare-maybe once a month. His tinnitus decreased and he regained some of his lost confidence. He returned to work part-time and recently took his first trip outside Hardoi in five years.
FAQ: Meniere’s Disease
Q: Can Meniere’s disease be cured?
No, there is no cure — but that doesn’t mean you have to live with uncontrolled attacks. With proper treatment, most patients achieve excellent control of their vertigo episodes. Diet, diuretics, and intratympanic treatments have transformed outcomes. Some patients do go into prolonged remission, particularly in the later stages when the inner ear may “burn out.” About 1 in 3 patients see significant spontaneous improvement over time.
Q: Is Meniere’s life-threatening?
The disease itself is not. But the attacks are dangerous — you can fall and seriously injure yourself, or have an attack while driving. This is why fall prevention and not driving during active disease phases are non-negotiable parts of management.
Q: Will I go deaf?
Not necessarily, and not if we manage the disease properly. In early and middle stages, the hearing loss fluctuates and much of it is recoverable. Long-term studies show that with treatment, the majority of patients retain serviceable hearing in the affected ear. In untreated or severely progressive disease, permanent significant hearing loss occurs in about 30-50% of cases. Regular audiograms to monitor hearing are essential.
Q: How long do attacks last?
Anywhere from 20 minutes to 12 hours — this wide range is actually one of the diagnostic features. If your spinning episodes consistently last only seconds (like BPPV) or consistently last more than 24 hours, we need to reconsider the diagnosis.
Q: What is the best diet for Meniere’s in India?
Low sodium is the foundation — under 1,500mg per day in most cases. This means eliminating namkeen, papad, achar, all processed and restaurant food. Use lemon, jeera, amchur, and fresh herbs for flavour. Avoid caffeine and alcohol. This dietary change alone can reduce attacks by 30-40% in many patients.
Q: Can I fly if I have Meniere’s?
Yes, but with precautions. Only fly when your disease is in a stable phase. Carry emergency medication in hand luggage. Stay well hydrated. Avoid salty airline snacks. Cabin pressure changes can trigger attacks, so timing your travel carefully is important.
Q: Is intratympanic injection painful?
It is much less uncomfortable than most patients expect. We numb the ear canal first with local anaesthetic. The injection through the eardrum takes a few seconds. Most patients feel a cold sensation as the medication enters the middle ear space. The procedure takes about 10-15 minutes total, and most patients can drive home afterwards.
Q: Can stress alone cause Meniere’s attacks?
Stress doesn’t cause Meniere’s, but it reliably triggers attacks in susceptible patients. The physiological mechanism involves stress hormones affecting inner ear fluid dynamics. Managing stress — through sleep, exercise, psychological support — is an active treatment component, not just a lifestyle nicety.
Author Bio
Dr. Prateek Porwal, MBBS, DNB ENT, CAMVD | ENT & Vertigo Specialist is an ENT Surgeon with special interest in vertigo and vestibular disorders at Prime ENT Center, Hardoi, UP. He has been managing complex cases of Meniere’s disease, BPPV, and vestibular dysfunction for over a decade. Dr. Porwal believes in patient education and combining evidence-based medicine with personalized care for each patient’s unique situation.
If you’re experiencing symptoms of Meniere’s disease, please reach out. Early diagnosis and treatment can significantly improve your quality of life.
Call 7393062200 or WhatsApp https://wa.me/917393062200
Prime ENT Center, Hardoi, UP
Website: drprateekporwal.com
Medical Disclaimer:
References
- Magnan J, Özgirgin ON, Trabalzini F et al.. European Position Statement on Diagnosis, and Treatment of Meniere’s Disease. J Int Adv Otol. 2018. PubMed
- Hoskin JL. Ménière’s disease: new guidelines, subtypes, imaging, and more. Curr Opin Neurol. 2022. PubMed
- Zhang S, Guo Z, Tian E et al.. Meniere disease subtyping: the direction of diagnosis and treatment in the future. Expert Rev Neurother. 2022. PubMed
This article is for educational purposes only and does not constitute medical advice, diagnosis or prescribing guidance. All medications must be taken under direct supervision of a qualified physician. Consult Dr. Prateek Porwal at Prime ENT Center, Hardoi for personalised treatment.
References
- Committee on Hearing and Equilibrium guidelines for the diagnosis and evaluation of therapy in Meniere’s disease. Otolaryngology–Head and Neck Surgery. 1995;113(3):181–185.
- Thirlwall AS, Kundu S. Diuretics for Ménière’s disease or syndrome. Cochrane Database of Systematic Reviews. 2006;(3):CD003599.
- Pullens B, van Benthem PP. Intratympanic gentamicin for unilateral Ménière’s disease or syndrome. Cochrane Database of Systematic Reviews. 2011;(3):CD008234.
- Espinosa-Sanchez JM, Lopez-Escamez JA. Menière’s disease. Handbook of Clinical Neurology. 2016;137:257-277.
- van Esch BF, et al. Efficacy of Betahistine and Diuretics in Menière’s Disease: A Systematic Review. Otolaryngology–Head and Neck Surgery. 2017;157(3):421-427.
- Staab JP, et al. Diagnostic criteria for persistent postural-perceptual dizziness (PPPD): Consensus document of the Committee for the Classification of Vestibular Disorders of the Bárány Society. Journal of Vestibular Research. 2017;27(4):191-208.
- Nevoux J, et al. International consensus (ICON) on treatment of Ménière’s disease. European Annals of Otorhinolaryngology, Head and Neck Diseases. 2018;135(1S):S29-S32.
- Tyrrell JS, et al. Meniere’s disease and psychological morbidity: a study using the Nottingham Health Profile. Clinical Otolaryngology. 2015;40(5):466-471.
- Strupp M, et al. Management of vestibular disorders. Journal of Neurology. 2016;263(Suppl 1):S24-S34.
- Lopez-Escamez JA, et al. Diagnostic criteria for Menière’s disease. Journal of Vestibular Research. 2015;25(1):1-7. (Bárány Society/AAO-HNS 2015 Criteria)
