By Dr. Prateek Porwal, ENT & Vertigo Specialist | Prime ENT Center, Hardoi
Last Updated: February 2026 | VAI Budapest 2025 Award Recipient
In my clinic, patients often use “dizziness” and “vertigo” interchangeably, but they’re different things. Dizziness is a broader termlightheadedness, unsteadiness, feeling faint, floating sensation. Vertigo is spinning. The distinction matters because the causes of dizziness and treatments differ significantly. Let me walk through what I actually see causing dizziness in my UP practice and help you understand which category your symptoms fall into.
Dizziness vs. Vertigo: The Critical Distinction
I see patients every week who’ve been misdiagnosed because their doctor didn’t distinguish between dizziness and what is vertigo. Dizziness is any sensation of lightheadedness or feeling unsteady. Vertigo is specifically the sensation that you or the room is spinning. This matters because:
- Dizziness usually comes from cardiovascular, metabolic, or neurological causes
- Vertigo usually comes from inner ear or central nervous system problems
- Treatment approaches are completely different
The Main Dizziness Causes I Treat
1. Dehydration: The Hidden Culprit in North India
Among all causes of dizziness, I see this constantly in Hardoi, especially during hot months. When your body loses fluids faster than you replace them, blood volume drops, oxygen to the brain decreases, and you feel lightheaded or dizzy. This is one of the most common causes of dizziness I see, yet it’s often overlooked because it seems too simple.

Signs I look for:
- Thirst (obvious, but people ignore it)
- Dry mouth and sticky feeling
- Dark yellow urine
- Fatigue and weakness
- Headache
- Dizziness that improves within 15-30 minutes of drinking water
- Symptoms worse in afternoon and evening
Why it’s so common in UP: Heat exposure during summer months, inadequate water intake during work, diarrhea from foodborne illness, vomiting, sweating from physical labor in fields. In my practice, I’ve had farmers come in with severe dizziness that resolved completely after one glass of water.
The fix is simple: drink enough water that your urine is pale yellow. For some patients, oral rehydration solution (salt and sugar water, like you’d use for cholera prevention) works faster than plain water because it replaces electrolytes too, not just fluid.
2. Low Blood Sugar (Hypoglycemia)
Image Source: Canva
Another overlooked causes of dizziness — your brain runs on glucose. When it drops too low, the brain panics and triggers symptoms. I see this especially in diabetic patients who take insulin but skip mealsa dangerous combination. It also happens in non-diabetics who fast too long, skip breakfast, or have intense physical activity on an empty stomach.
Symptoms to recognize:
- Dizziness and shakiness
- Rapid heartbeat (pounding sensation)
- Sweating (even in cool environments, which is distinctive)
- Difficulty concentrating or mental fog
- Intense hunger
- Anxiety or feeling of impending doom
- Comes on suddenlypatient is fine one moment, dizzy the next
- Improves within 5-10 minutes of eating sugar
Treatment: Eat something with quick carbssugar, fruit juice, fruit. If diabetic, keep glucose tablets or candy available. For diabetics, medication adjustment with their doctor is necessary to prevent recurrence. I always ask my dizzy diabetic patients: “When did you last eat?” A shocking number haven’t eaten in 12+ hours.
3. Orthostatic Hypotension (The Stand-Up Syndrome)
Image Source: Canva
One of the scariest causes of dizziness for patients — a sudden drop in blood pressure when you stand up. Your brain temporarily doesn’t get enough oxygen. One of the most common causes of dizziness in the elderly and in patients on blood pressure medications.
This also applies to seniors and older adults who may face similar symptoms.
When it happens:
- Standing up quickly from lying down or sitting
- After bed rest or lying down for extended time
- In elderly patients (very commonperhaps 30% of my elderly patients and seniors report this)
- With blood pressure medications, especially if dose is too high
- Dehydration makes it dramatically worse
- During hot weather or fever
- After large meals
How to prevent it:
- Stand up slowly, wait a moment before moving
- Sit on the edge of bed for 30 seconds before standing
- Flex your leg muscles while sitting (calf raises help pump blood)
- Stay well-hydrated
- Compression stockings can help in severe cases
- Avoid sudden position changes
- Have your blood pressure medications checkeddose might be too high
4. Anemia: The “Hidden” Cause in India
India has one of the highest rates of anemia in the world. I see anemic womenparticularly in the childbearing yearswith dizziness as a primary complaint. When your red blood cell count is low, oxygen delivery to the brain is reduced, causing lightheadedness.
Signs of anemia:
- Dizziness, especially with activity or exertion
- Fatigue out of proportion to activity
- Shortness of breath with normal activity
- Pale skin, pale inner eyelids
- Rapid heartbeat
- Headaches
- Difficulty concentrating
- History of heavy menstrual periods (in women)
Why it’s endemic in India: Vegetarian diet low in bioavailable iron, high burden of parasitic infections, heavy menstrual bleeding in women without access to treatment, poverty affecting nutrition. A simple blood test (hemoglobin level) diagnoses this. If anemia is the cause, iron supplementation or treatment of underlying causes (like parasites) resolves the dizziness.
5. Hypothyroidism: The Metabolic Dizziness Cause
Low thyroid function slows metabolism and can affect blood pressure regulation and brain function. This is common in both men and women but often missed because the presentation is subtle.
Associated symptoms:
- Dizziness
- Weight gain despite normal eating
- Fatigue
- Cold intolerance
- Dry skin
- Hair loss
- Slow heart rate
- Constipation
- Depression or low mood
A TSH blood test confirms this. If it’s thyroid-related dizziness, thyroid hormone replacement resolves it reliably over weeks to months.
6. Inner Ear Disorders Causing Dizziness (Not Vertigo)
Sometimes dizziness (not true vertigo or spinning) comes from inner ear problems. The symptoms are milder than true BPPVunsteadiness rather than spinning sensation.
Presentation:
- Unsteadiness, especially in darkness or with eyes closed
- Balance problems walking in straight line
- Difficulty with stairs or uneven ground
- May have hearing changes or tinnitus
- Feeling of instability, not spinning
These often benefit from vestibular rehabilitation exercises that retrain the brain’s balance compensation. Some patients also benefit from treating underlying conditions like vestibular migraine.
7. Anxiety and Stress: The Psychological Component
I see a lot of anxiety-causing dizziness in my practice. Stress triggers fight-or-flight response, which changes breathing (hyperventilation), heart rate, and blood pressure. This causes real dizziness, not imaginary.
The pattern I recognize:
- Dizziness comes during stressful periods or times of anxiety
- Racing heart and rapid, shallow breathing
- Feeling of impending doom
- Muscle tension in neck, shoulders
- Improves with relaxation or reassurance
- No physical exam findings suggesting inner ear or cardiac disease
- Patient’s stress level clearly correlates with symptom severity
My approach: I never dismiss anxiety-related dizziness as “just in your head.” It’s real physiology. But it requires ruling out medical causes first (physical exam, maybe simple tests). Then address the anxietybreathing exercises, meditation, sometimes medication. Cognitive behavioral therapy is very effective.
8. Medication-Induced Dizziness: A Very Common Cause
Many drugs cause dizziness as a side effect. Medication-related causes of dizziness are common. Drug-related causes of dizziness include blood pressure meds, antidepressants, antihistamines, pain meds, antibioticsthe list is long. Every time I see a patient with dizziness, I review their medication list carefully.
Common culprits I see frequently:
- Blood pressure medications (especially if dose too high)patient’s BP drops too much
- Antihistamines for allergiescause drowsiness and dizziness
- Antidepressants (SSRIs, tricyclics)can lower blood pressure
- Sleep medicationsleave person groggy and unsteady next day
- Pain medications with sedationimpair balance and coordination
- Anticonvulsantscause dizziness as known side effect
- Antibiotics, particularly aminoglycosides (like an ototoxic antibiotic for infections)can cause ototoxicity and damage inner ear
- a vasodilator medication for vertigoironically, some patients get worse dizziness
If dizziness started after starting a new medication, don’t stop it without talking to your doctor, but mention the side effect. Often dose adjustment or switching to a different drug helps. I’ve had patients on blood pressure meds for years at doses that were too high for themsmall adjustment fixed the dizziness.
9. Cervicogenic Dizziness: The Neck Connection (Or Lack Thereof)
I need to address this because I see cervical vertigo misdiagnosis constantly. Patients come in convinced their dizziness is from cervical spondylosis (neck arthritis) because they have neck pain, and somewhere they read that the neck can cause dizziness.
The controversy: Yes, the neck has balance-related nerves and sensors. Can severe neck problems cause some balance issues? Theoretically yes. But is this actually a common diagnosis? No. And most “cervical chakkar” diagnosed by non-specialists is actually BPPV, anxiety, or vestibular migraine.
Signs of actual cervicogenic dizziness (rare):
- Dizziness specifically triggered by neck movement in certain directions
- Associated with significant neck pain and limited range of motion
- Dizziness reproduced by positioning neck in specific way
- Imaging shows severe cervical pathology
The problem: Many doctors X-ray the neck, see some arthritis (common in anyone over 40), and blame that for dizziness without considering other causes. Result: patients waste money on neck treatments that don’t help, miss the real diagnosis, and remain dizzy. If true BPPV is present, it continues untreated.
Causes of Dizziness: Red Flags Requiring Urgent Assessment
Most dizziness is benign, but some causes need urgent medical evaluation:
- Dizziness with chest pain or shortness of breath – Could be cardiac
- Sudden severe dizziness with weakness, numbness, or speech problems – Could be stroke
- Dizziness after head injury with loss of consciousness – Head trauma
- Persistent dizziness with high fever – Infection
- Dizziness with loss of consciousness or syncope – Cardiac issue
- New dizziness in elderly patient on new medications – Often medication-induced, needs urgent review
Causes of Dizziness: How I Sort Out The Cause
When a patient comes to my clinic with dizziness, here’s roughly how I think through it:
First: History (5 minutes of questions)
- Onset: Sudden (more likely cardiovascular/neurological) vs. gradual (more likely metabolic)
- Duration: Seconds (BPPV) vs. minutes (anxiety) vs. hours (migraine)
- Character: Spinning (vertigo) vs. lightheadedness (non-vertigo)
- Associated symptoms: Hearing loss (inner ear)? Chest pain (cardiac)? Anxiety (psychological)?
- Medications: Any started recently?
Second: Examination (10 minutes)
- Blood pressure: Sitting and standing – check for orthostatic drop
- Heart rate and rhythm
- Balance tests
- Neurological exam
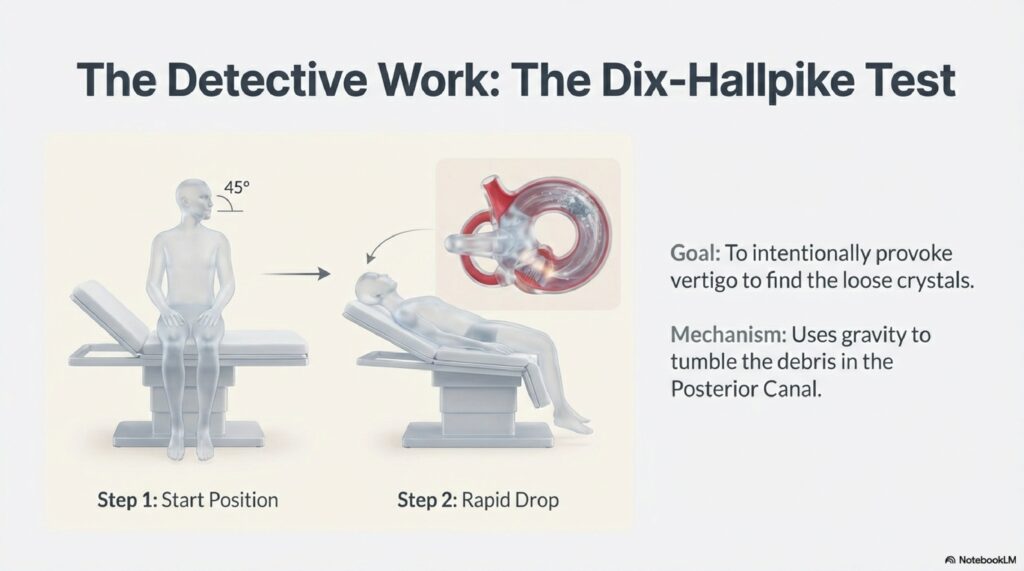
- Dix-Hallpike test (if vertigo suspected)
Third: Testing (if needed)
- Blood tests: Hemoglobin, glucose, thyroid, electrolytes
- ECG: If cardiac cause suspected
- VNG: If inner ear pathology suspected
Usually this diagnostic process resolves most cases.

Frequently Asked Questions — Causes of Dizziness
Is dizziness dangerous? — causes of dizziness explained
Usually no. Most dizziness comes from dehydration, low blood pressure, or anxietyeasily correctable. But persistent unexplained dizziness warrants evaluation to rule out medical causes like cardiac issues or metabolic problems.
What’s the difference between dizziness and vertigo again?
Dizziness is lightheadedness, unsteadiness, floating feeling. Vertigo is spinninga specific sensation that you or the room is rotating. Different causes, different treatments.
Should I see a doctor for dizziness?
See a doctor if: dizziness persists despite addressing obvious causes (hydration, eating, standing slowly), it’s accompanied by other symptoms, or it’s affecting your daily life and safety.
Can I treat my dizziness at home?
For simple causes like dehydration or low blood sugar, yes. For persistent or unexplained dizziness, proper diagnosis is important. Don’t just ignore it and hope it goes away.
What medication can I take for dizziness?
That depends on the cause. Antihistamines help some types of dizziness but treating the underlying cause (hydration, medication change, anxiety management) is better than masking symptoms.
Is dizziness a sign of serious illness?
It can be, but it usually isn’t. Most dizziness is benign and self-limited. However, dizziness with stroke-like symptoms or cardiac symptoms is an emergency.
Why am I dizzy when I stand up?
Most likely orthostatic hypotensionblood pressure drop when standing. Happens especially with dehydration, medications, or in elderly. Prevention: stand slowly, stay hydrated.
Can anemia cause dizziness?
Yes, absolutely. Low hemoglobin means less oxygen to brain. Iron supplementation after confirming anemia usually resolves this.
Is “cervical chakkar” a real diagnosis?
True cervical dizziness from neck problems is rare. Most patients labeled with this actually have BPPV, anxiety, or vestibular migraine. Get a proper diagnosis before accepting the cervical spondylosis explanation.
Can stress cause dizziness?
Yes, absolutely. Anxiety and stress trigger fight-or-flight response, hyperventilation, and blood pressure changesall causing real dizziness. But rule out medical causes first.
Experiencing vertigo or chakkar? Get diagnosed usually in one visit.
Dr. Prateek Porwal, ENT Surgeon & Vertigo Specialist at PRIME ENT Center, Hardoi UP VAI Budapest 2025 International Award recipient. Most BPPV cases resolved in the same appointment.
Call/WhatsApp: 7393062200 | Chat on WhatsApp
Medical
Causes of Dizziness — When to See a Doctor
If you’re experiencing symptoms related to this condition, it’s important to seek professional evaluation. In my practice in Hardoi, I typically recommend scheduling a consultation if symptoms persist for more than a few days or significantly impact your daily activities.
Don’t wait for symptoms to worsen. Early diagnosis and intervention often lead to better outcomes. Contact Prime ENT Center to schedule your VNG evaluation with advanced vestibular testing equipment available in Hardoi.
Causes of Dizziness: Management and Prevention
While some causes can’t be prevented, there are steps you can take to manage and reduce risk:
- To prevent common causes of dizziness, maintain good overall health with regular exercise
- To prevent hearing-related causes of dizziness, protect your ears from loud noise exposure
- Practice good hygiene to reduce infection risk
- To address common causes of dizziness, stay hydrated and maintain balanced nutrition
- Address stress through relaxation techniques
We’ve seen significant improvements in patient outcomes when these preventive measures are combined with proper medical care.
References
- Karatas M. Central vertigo and dizziness: Epidemiology, differential diagnosis, and common causes. Neurologist. 2008;14(6):355–364.
Further Reading
This article is for educational purposes only. Please consult Dr. Prateek Porwal at Prime ENT Center, Hardoi or book an online consultation at 7393062200. Website: drprateekporwal.com
