Vestibular Migraine: 4-Step Treatment Guide (2026)
TL;DR: Vestibular migraine is a spinning form of migraine where vertigo and imbalance are often more disabling than the headache, and standard pain drugs like triptans frequently fail to control the dizziness. Effective treatment usually needs a 4‑pillar plan: strict trigger and diet control, daily preventive migraine medicines (including newer CGRP therapies when needed), customized vestibular rehabilitation, and psychological support such as CBT to retrain the brain’s balance and pain networks. For patients in Hardoi, working with a vertigo‑focused migraine specialist allows this full protocol to be tailored to your specific triggers, comorbid anxiety, and lifestyle so that attacks become shorter, less intense, and less frightening over time
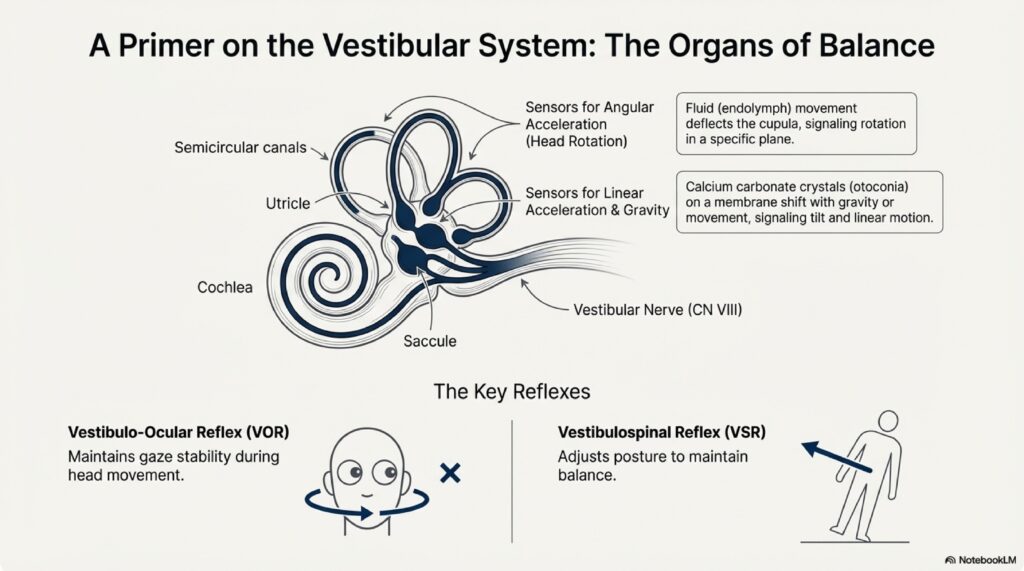
What is BPPV? Types, Symptoms & Best Treatments
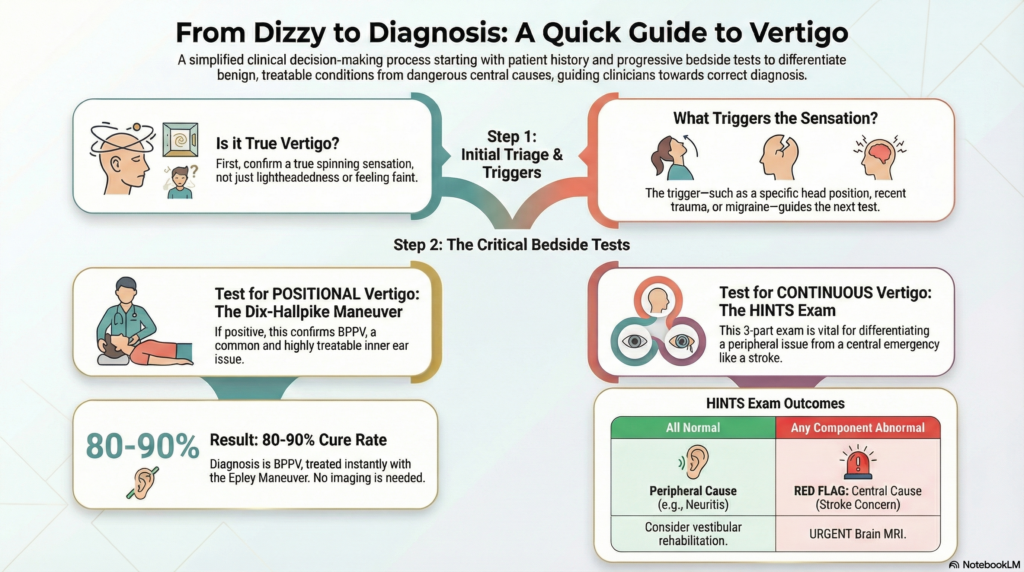
Last Updated: February 2026 | Medically Reviewed by Dr. Prateek Porwal, ENT & Vertigo Specialist | Prime ENT Center, Hardoi You wake up at 3 AM. Your bedroom begins spinning violently—like the world has become a carnival ride you never boarded. You reach for the bedside lamp but stop yourself. Any movement makes it worse. […]
The Cervical Vertigo Misdiagnosis Trap: Why Neck X-Rays Mislead
🎯 TL;DR (Too Long; Didn’t Read)
Main trap: Cervical spondylosis (bone spurs, disc space narrowing) on X-rays is INCIDENTAL and usually NOT the cause of vertigo
Most common misdiagnosed cause: BPPV (Benign Paroxysmal Positional Vertigo)—displaced inner ear crystals, NOT a neck problem
Gold standard test: Dix-Hallpike maneuver (90–95% sensitivity; bedside; FREE; diagnostic AND therapeutic)
Time to cure: 80–90% of BPPV cases cured within MINUTES with Epley maneuver
Why imaging misleads: Neck X-rays/CT show bone spurs (incidental in 70–80% of elderly) but CANNOT explain spinning sensation
Red flag for emergency: Abnormal HINTS exam (3-minute eye movement test) suggests central cause (stroke)—needs MRI urgently
Action plan: If told you have “cervical vertigo,” request Dix-Hallpike test; if positive, ask for Epley maneuver IMMEDIATELY
Your Anxiety Is Making You Dizzy: The Stress-Vertigo Link

Main concept: PPPD (Persistent Postural-Perceptual Dizziness) = anxiety + brain’s threat system overdrive—NOT structural ear problem
Brain connection: Vestibular system directly wired to amygdala (fear center); anxiety triggers false “balance alarms”
Common misconception: “All in your head”—WRONG; it’s a real functional disorder, not psychiatric (though anxiety is involved)
Diagnostic test: Standard imaging (MRI, hearing tests) = NORMAL (explains why doctors say “nothing wrong”)
Diagnostic criteria: 3+ months symptoms, triggered by upright posture/movement/complex visuals (supermarket effect)
Best treatment combination: SSRI medication + Cognitive Behavioral Therapy (CBT) + Vestibular Rehabilitation Therapy (VRT) = 70–80% improvement
Critical mistake: Bed rest + avoidance = WORSE (isolates patient, maintains threat loop; movement + exposure = recovery)
The Vertigo Medication Trap: Why Pills Make It Worse
🎯 TL;DR (Too Long; Didn’t Read)
Main trap: Vestibular suppressants (antihistamines, benzodiazepines, anticholinergics) provide SHORT-TERM relief but PREVENT the brain’s natural healing process (central compensation)
72-hour rule: Suppressants appropriate ONLY for first 24–72 hours of acute vertigo attack; beyond that, they delay recovery by months
BPPV reality: Physical repositioning maneuvers (Epley, Semont) cure 80–90% of cases; NO medication can move ear crystals back to normal position
Rebound dizziness: Abrupt medication withdrawal causes temporary severe dizziness, BUT this is a sign the brain is waking up—not disease recurrence
Safe exit: Gradual medication taper + early mobilization + vestibular rehabilitation therapy (VRT) = true recovery (60–80% improvement)
Elderly risk: Suppressants dramatically increase fall risk, cognitive slowing, and drug-induced Parkinsonism in adults 65+
Action plan: If on dizziness pills >72 hours without diagnosis, ask for vestibular evaluation (Dix-Hallpike, HINTS) and supervised medication taper
Stop Calling Everything ‘Chakkar’: BPPV vs Vestibular Neuritis
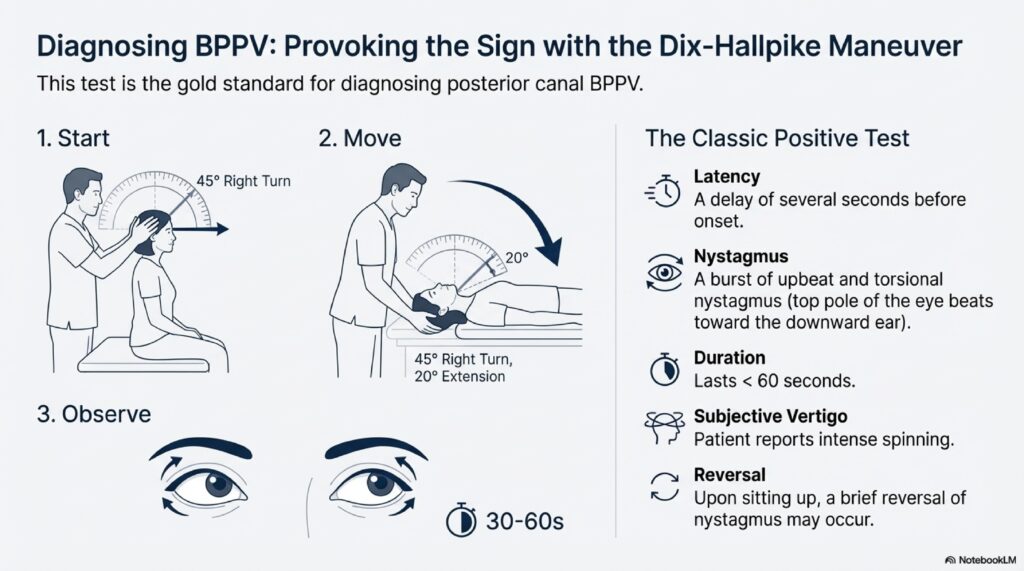
BPPV (Benign Paroxysmal Positional Vertigo): Seconds-long spinning triggered by specific head movements, caused by loose crystals in the inner ear. Treatable with Epley Maneuver (success rate 80-90%).
Vestibular Neuritis: Viral inflammation of the balance nerve causing persistent dizziness lasting hours to days. Self-limiting; recovery occurs with central compensation.
Posterior Circulation Stroke: Dangerous condition mimicking vestibular neuritis but identified by failing the HINTS exam (Head Impulse, Nystagmus, Test of Skew). Requires immediate emergency intervention.
Traveling with Vertigo? The 5-Minute Motion Sickness Hack

The problem: Motion sickness = sensory mismatch (inner ear, eyes, body position disagree)—brain interprets as “toxin” → triggers vomiting center
The 5-minute hack: Daily vestibular habituation (gaze stabilization X1, head movement drills) for 3–7 days BEFORE travel = brain recalibrates
Immediate travel trick: Sit in front seat + fixate on horizon (aligns visual + vestibular signals) = prevents nausea
Critical medication rule: Vestibular suppressants (scopolamine, meclizine) = max 1–3 days ONLY (longer use = permanent dizziness)
Special conditions require prep: BPPV = morning exercises; migraine = 48-hour dietary restriction; Menière’s = sodium reduction; PPPD = visual desensitization
Pharmacological backup: Scopolamine patch (most effective), meclizine (less sedating), ondansetron (for breakthrough nausea)
Recovery goal: Teach brain to accept motion = habituation = sustained travel confidence without medication
Vertigo or Stroke? The 60-Second HINTS Test

