By Dr. Prateek Porwal, ENT & Vertigo Specialist | Prime ENT Center, Hardoi
Last Updated: February 2026 | VAI Budapest 2025 International Award Recipient
What is Vertigo? Understanding the Spinning Sensation
Every week, I see patients in my Hardoi clinic who walk in looking genuinely scared convinced they’re either having a stroke or “going mad.” One lady from Sitapur last month told me, “Doctor saab, mujhe lagta hai ghar goom raha hai.” Her husband had dragged her across three hospitals before reaching me. She had BPPV completely treatable, took me 8 minutes. But she’d suffered for 4 months.
That’s the real problem with vertigo in India. It’s one of the most common conditions I see, yet most patients have no idea what it actually is or that it can be fixed quickly. So let me explain it plainly, the way I’d explain it sitting across from you in my clinic.
Defining Vertigo: More Than Just Dizziness
Vertigo is a specific kind of dizziness. Not the “I stood up too fast” kind. Not the lightheaded feeling you get when you’re hungry. Vertigo is the false, unmistakable sensation that you or the room around you is spinning, tilting, or swaying when absolutely nothing is moving.
The American Academy of Otolaryngology defines it as “the sensation of motion when no motion is occurring relative to earth’s gravity.” In simpler terms: your brain is receiving wrong signals from your balance system, and it’s convinced you’re spinning when you’re perfectly still.
People in North India often say “chakkar aa raha hai” but there are actually at least 3-4 completely different conditions that get lumped under that phrase. Understanding which one you have changes everything about the treatment. This is why I wrote a full piece on how BPPV, vestibular neuritis, and other chakkar conditions differ worth reading if you’ve been confused about your diagnosis.
Vertigo vs. Acrophobia Not the Same Thing
People often use “vertigo” to mean fear of heights. Even Hollywood did this the Hitchcock film “Vertigo” is about acrophobia, not the medical condition. Medically, acrophobia (fear of heights) and vertigo are completely different. Yes, some people with balance disorders feel worse on heights, but vertigo doesn’t require any height at all. My patient with BPPV got her spinning attack while rolling over in bed at ground level.
Symptoms of Vertigo: What Does It Feel Like?

The main symptom is that spinning or rotating sensation as if the world is on a turntable. But it comes in different flavors:
- The room is spinning rapidly (most common in BPPV)
- You feel like YOU are spinning
- A feeling of being pulled sideways or tilted
- The ground feels like it’s moving under your feet
- Everything is rocking, like being on a boat
The duration varies hugely. In BPPV (the most common type), attacks last 10-60 seconds and stop on their own. In vestibular neuritis, it can last days. In Meniere’s disease, attacks run 20 minutes to several hours.
Intensity also ranges wildly. Some patients feel mild unsteadiness. Others vomit, can’t walk, and lie frozen in bed. Both can be the same condition BPPV just different canals affected.
Other Symptoms That Come Along
Vertigo rarely shows up alone. In my experience, patients usually also have:
- Nausea and sometimes vomiting (especially in acute attacks)
- Abnormal eye movements eyes flicking back and forth involuntarily (nystagmus) this is actually what we look for to confirm teh diagnosis
- Headache (especially in vestibular migraine)
- Ringing in the ears (tinnitus) more common in Meniere’s
- Hearing loss again, Meniere’s, or vestibular neuritis
- Sweating, pale skin during acute attacks
- Difficulty concentrating, “brain fog” afterward
These associated symptoms are diagnostically useful. When a patient tells me they have ringing AND vertigo AND hear muffled sounds, I’m thinking Meniere’s before they finish the sentence. When it’s pure spinning attacks with head movement and no hearing symptoms, it’s almost certainly BPPV.
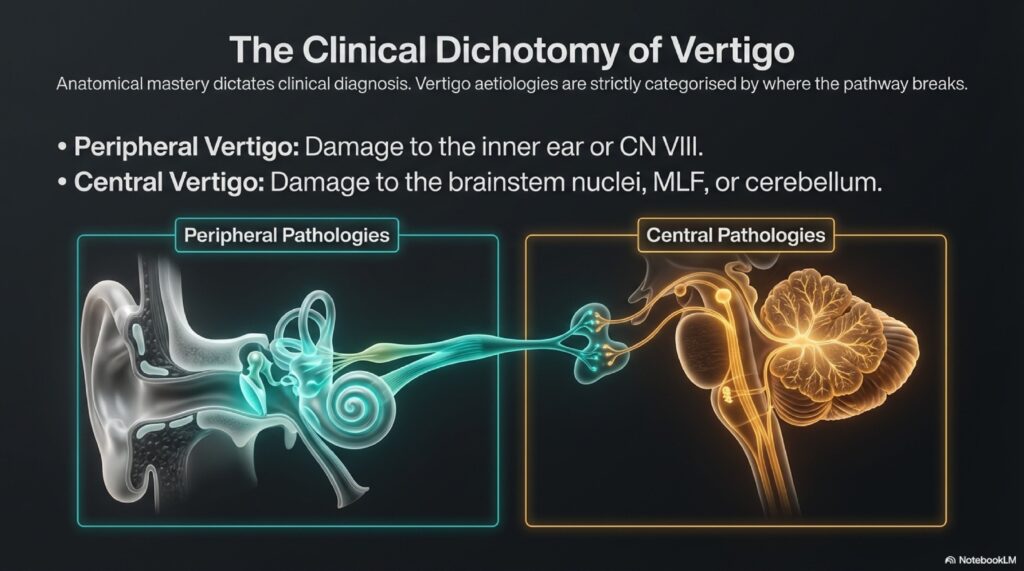
Types of Vertigo: Peripheral vs. Central
This is the most important distinction in vestibular medicine, and yet most general practitioners don’t explain it clearly.
Peripheral Vertigo
This is where the problem is in the inner ear or the vestibular nerve connecting it to the brain. 80-85% of all vertigo is peripheral. The good news: peripheral vertigo is nearly always treatable, often quickly.
Common causes:
- Benign Paroxysmal Positional Vertigo (BPPV) the most common, caused by displaced crystals in the inner ear
- Vestibular neuritis viral infection of the vestibular nerve, causes days of severe spinning
- Meniere’s disease fluid buildup in the inner ear, episodic attacks with hearing changes
- Labyrinthitis inflammation of the entire inner ear
- Superior canal dehiscence syndrome a bony defect in the inner ear roof
Peripheral vertigo is typically intense and episodic. The nystagmus (eye flicking) follows predictable patterns that a trained ENT can read like a map to the diagnosis.
Central Vertigo
Central vertigo means the problem is in the brain itself brainstem or cerebellum. This is the 15-20% that concerns us more, because the causes can be serious:
- Stroke or TIA this is the one nobody wants to miss. I’ve written about how to distinguish vertigo from stroke and it’s reading every patient should do.
- Brain tumors pressing on balance centers
- Multiple sclerosis
- Vestibular migraine (technically central in origin)
- Certain medications some blood pressure drugs, antibiotics, and antiepileptics can affect the cerebellum
Central vertigo tends to be more constant, less dramatic moment-to-moment, and accompanied by other neurological signs: double vision, slurred speech, limb weakness, severe headache. The nystagmus patterns are “atypical” they don’t match any inner ear pattern. This is what makes the HINTS exam so valuable in emergency settings.
Common Causes of Vertigo
Benign Paroxysmal Positional Vertigo (BPPV)
BPPV causes about 32% of all peripheral vertigo cases and in my clinic, it feels like more. These are patients who get brief, violent spinning episodes when they roll over in bed, look up at a high shelf, or tilt their head. The cause: tiny calcium carbonate crystals (otoconia) have dislodged from their proper home in the inner ear and wandered into one of the semicircular canals.
The treatment is mechanical we physically reposition the crystals using a specific head maneuver (Epley is most common, but for complex cases I use the Bangalore Maneuver, which I’ve developed for difficult horizontal canal variants). But Most patients feel better within one session. No surgery, no long-term medications.
If you suspect BPPV, read my complete BPPV guide it covers all 3 types, diagnosis, and treatment in detail.
Vestibular Neuritis and Labyrinthitis
This is when a virus attacks the vestibular nerve. Patients typically wake up one morning with severe, constant spinning often so bad they can’t walk and are vomiting. It lasts days. The acute phase is managed with vestibular suppressants (careful overuse makes recovery slower). The recovery phase is managed with vestibular rehabilitation exercises.
Labyrinthitis is similar but the infection reaches the cochlea too, causing hearing loss alongside the vertigo.
Meniere’s Disease
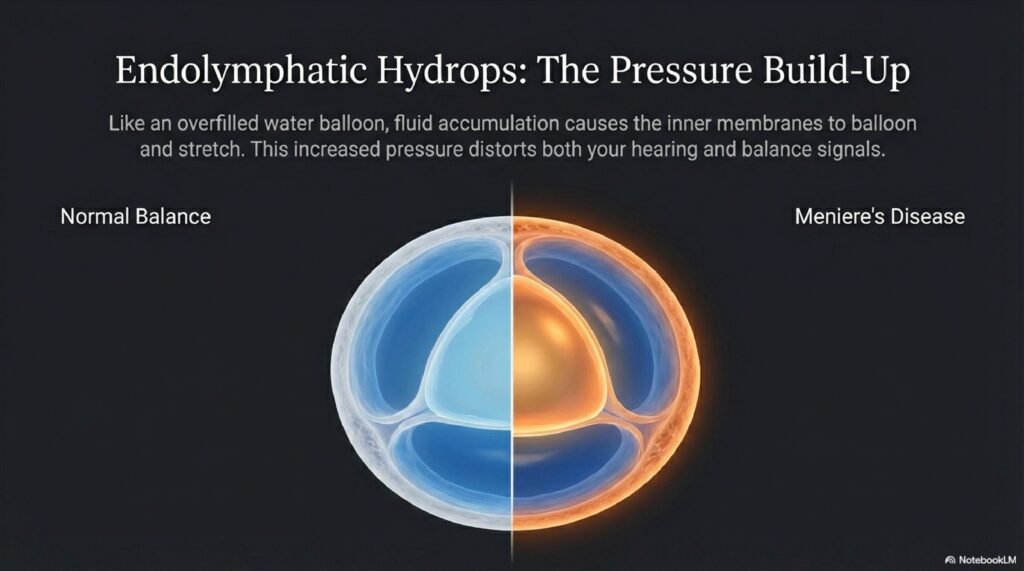
Meniere’s is a chronic inner ear disorder involving excess fluid (endolymph) buildup. It presents as a triad: episodic vertigo (attacks lasting 20 minutes to several hours), fluctuating low-frequency hearing loss, and tinnitus (roaring or whooshing sound, usually one-sided). Many patients also feel “ear fullness” like the ear is blocked.
This is one of the more challenging conditions to manage long-term, but very manageable with dietary changes (low salt diet primarily), diuretics, and in some cases, intratympanic injections.
Vestibular Migraine
This is massively underdiagnosed in India. Patients get vertigo attacks sometimes without any headache at all triggered by hormonal changes, certain foods, bright lights, or stress. It’s the second most common cause of recurrent vertigo and I see it weekly. Read my full vestibular migraine guide if you get recurrent attacks without a clear BPPV diagnosis.
Anxiety and PPPD
Yes, anxiety genuinely causes dizziness and it’s not “all in the head” in the dismissive sense. There’s a real physiological mechanism. Persistent Postural-Perceptual Dizziness (PPPD) is now a recognized diagnosis chronic dizziness driven by over-sensitized balance centers, often triggered initially by a real vestibular event like BPPV or neuritis.
Cervicogenic Dizziness
One of the most overtreated “diagnoses” in India is “cervical spondylosis causing vertigo.” Most cervical X-rays are over-read, and most patients labeled with “cervical vertigo” actually have BPPV or vestibular migraine. I wrote about this misdiagnosis problem in detail it’s one of the most common traps I see patients falling into.
Diagnosing Vertigo: Tests and Procedures

Diagnosing vertigo properly starts with a good history when does it happen, how long does it last, what triggers it, does it come with hearing symptoms or headache? From there, the physical exam does most of the work.
Key diagnostic tests I use:
- Dix-Hallpike maneuver the gold standard for BPPV. I lay the patient flat with their head turned and hanging, and watch the eyes. The nystagmus pattern tells me exactly which canal is involved.
- Supine Roll Test for horizontal canal BPPV, which Dix-Hallpike misses.
- HINTS exam Head Impulse, Nystagmus, Test of Skew used when I’m worried about stroke. More on that here.
- VNG (Videonystagmography) records eye movements using infrared cameras. Useful for complex cases where the bedside exam alone isn’t conclusive.
- Audiometry hearing test, essential when Meniere’s or vestibular neuritis is suspected.
- MRI only when there’s suspicion of central cause. I don’t order MRI for every vertigo patient in straightforward BPPV, it’s unnecessary and expensive.
Honestly, most clear-cut BPPV is diagnosed and treated in the same appointment. No waiting for lab results.
When to See a Doctor And When to Go Straight to Emergency
Not every vertigo attack is an emergency. But some red flags need immediate attention:
- Vertigo with sudden severe headache (“worst headache of your life”)
- Vertigo with double vision, facial numbness, or arm/leg weakness
- Vertigo with slurred speech or difficulty swallowing
- Falling toward one side, can’t walk at all
- New vertigo after a head injury
If any of these are present emergency department, not the local clinic. If it’s just spinning that comes and goes with head movement, no headache, no weakness book an ENT appointment.
Conclusion
Vertigo is not a single disease it’s a symptom that points to a cause. Find the cause, treat the cause, resolve the vertigo. In 2026, we have excellent diagnostic tools and highly effective treatments for most vertigo conditions. The majority of patients I see even those who’ve suffered for months can be treated effectively once properly diagnosed.
If you or someone in your family is struggling with chakkar, spinning, or balance problems, don’t keep taking a vasodilator medication indefinitely without a diagnosis. Come in, get examined properly, and find out what’s actually going on.
Frequently Asked Questions
What is the difference between vertigo and dizziness?
Vertigo is the specific sensation of spinning you or the room is rotating when it’s not. Dizziness is a broader term covering lightheadedness, unsteadiness, or faintness. All vertigo is dizziness, but not all dizziness is vertigo. This distinction matters because treatment is completely different.
What are the most common symptoms of vertigo?
The core symptom is spinning rotational movement sensation when stationary. This is usually accompanied by nausea, sometimes vomiting, involuntary eye movements (nystagmus), and balance difficulty. In BPPV, attacks last under a minute. In Meniere’s, they can last hours.
What causes vertigo?
Most vertigo (80-85%) comes from inner ear problems: BPPV (crystal displacement), vestibular neuritis (viral infection of the balance nerve), Meniere’s disease (fluid buildup), or labyrinthitis. The remaining 15-20% comes from brain causes including stroke, migraine, or medication side effects.
What is the difference between peripheral and central vertigo?
Peripheral means the inner ear or vestibular nerve is the problem this is more common and usually very treatable. Central means the brain (brainstem or cerebellum) is affected this is less common but potentially more serious, requiring imaging and careful evaluation.
Is vertigo a sign of a serious health problem?
Most vertigo is NOT serious BPPV and vestibular neuritis together account for the vast majority of cases and both are benign. However, vertigo with neurological symptoms (weakness, vision changes, severe headache, speech problems) can indicate stroke and needs immediate evaluation.
Can vertigo be cured?
BPPV can be resolved completely in 1-2 sessions with a repositioning maneuver. Vestibular neuritis usually resolves in weeks with rehabilitation. Meniere’s is managed rather than cured, but well-controlled with lifestyle changes and treatment. Vestibular migraine responds well to preventive medication.
How is vertigo diagnosed?
Diagnosis is primarily clinical a detailed history followed by bedside tests (Dix-Hallpike, Supine Roll, HINTS exam). For complex cases, VNG testing and audiometry are added. MRI is reserved for suspected central (brain) causes.
What should I do during a vertigo attack?
Sit or lie down immediately on the floor if necessary. Don’t drive. Keep your eyes open and fix your gaze on a stationary object. Avoid sudden head movements. If the attack is accompanied by chest pain, sudden severe headache, or weakness in limbs call emergency care immediately.
Can lifestyle changes help manage vertigo?
For Meniere’s disease, a low-salt diet makes a real difference. For vestibular migraine, avoiding triggers (certain foods, bright lights, poor sleep) matters. For BPPV, there are no lifestyle changes that prevent it but prompt treatment when it occurs prevents unnecessary suffering.
Are there exercises that help with vertigo?
Yes but the right exercises depend on the cause. Epley maneuver and related repositioning maneuvers are exercises for BPPV. Vestibular rehabilitation exercises (Cawthorne-Cooksey, gaze stabilization) help in vestibular neuritis recovery and PPPD. These should be guided by a vestibular specialist, not done randomly from YouTube.
Experiencing vertigo or chakkar? Get diagnosed usually in one visit.
Dr. Prateek Porwal, ENT Surgeon and Vertigo Specialist at PRIME ENT Center, Hardoi UP, has treated thousands of vertigo patients across Uttar Pradesh. VAI Budapest 2025 International Award recipient. Most BPPV cases resolved in the same appointment using proven repositioning maneuvers no long medication courses, no unnecessary MRIs.
Call/WhatsApp: 7393062200 | Chat on WhatsApp
Medical
When to See a Doctor
Seek immediate medical attention if you experience severe symptoms or sudden changes. For ongoing concerns, contact Prime ENT Center to schedule an evaluation. Early consultation often prevents complications and speeds recovery.
Disclaimer: This article is for educational purposes only. It does not constitute medical advice or prescribing guidance. All medications mentioned should only be taken under the direct supervision of a qualified physician. Specific doses, durations, and drug choices depend on your individual clinical condition and must be determined by your treating doctor. If you experience severe symptoms, please seek immediate medical attention.
References
- Karatas M. Central vertigo and dizziness: Epidemiology, differential diagnosis, and common causes. Neurologist. 2008;14(6):355–364.
About the Author
Dr. Prateek Porwal is an ENT & Vertigo Specialist with over 13 years of experience, holding MBBS (GSVM Medical College), DNB ENT (Tata Main Hospital), and CAMVD (Yenepoya University). He is the originator of the Bangalore Maneuver for Anterior Canal BPPV and has published research in Frontiers in Neurology and IJOHNS. Serving at Prime ENT Center, Hardoi.
