Introduction to Vestibular Neuritis — Complete Guide
I remember a patient who walked into my clinic — or more accurately, was practically carried in — a 38-year-old man who woke up at 3 am with the room spinning so violently he couldn’t sit up. He vomited six times before morning. By the time his family brought him to me, he was pale, exhausted, and genuinely terrified he was having a stroke or brain tumour.
He had vestibular neuritis.
This is one of the most common conditions I see in vertigo practice, and also one of the most under-diagnosed. Most patients spend days — sometimes weeks — getting CT scans, cardiac workups, and neurological evaluations before anyone looks at the vestibular nerve. By that time, the acute phase is over but the damage is done and recovery is already being delayed.
This article covers everything — what vestibular neuritis actually is, why it happens, how we diagnose it, how we treat it, and what the road to recovery genuinely looks like.
Table of Contents
- What Is Vestibular Neuritis?
- Causes — Why Does It Happen?
- Symptoms — What Patients Experience
- How Vestibular Neuritis Differs From Labyrinthitis
- Diagnosis — How We Confirm It
- Treatment — Acute Phase and Long-Term
- Vestibular Rehabilitation
- Recovery Timeline — What to Realistically Expect
- When Symptoms Don’t Go Away
- Frequently Asked Questions
What Is Vestibular Neuritis?
Vestibular neuritis is inflammation of the vestibular nerve — the nerve that carries balance information from the inner ear to the brain. When this nerve becomes inflamed, it stops sending accurate signals. The brain receives no input from one side, while the other ear continues to send normal signals. This mismatch is what creates the sensation of violent spinning.
The vestibular nerve has two divisions — superior and inferior. In most cases of vestibular neuritis, it’s the superior division that gets affected. This is important because the superior division supplies the horizontal and anterior semicircular canals, and the superior utricle. The inferior division, which supplies the posterior semicircular canal and saccule, is usually spared — which is one reason why BPPV can sometimes develop later (the posterior canal becomes vulnerable after a period of reduced blood supply and degeneration).
It’s a peripheral vestibular disorder — meaning the problem is in the inner ear nerve, not the brain itself. This distinction matters enormously for prognosis. Peripheral vestibular disorders compensate. The brain is remarkably good at learning to function with unequal inputs from the two sides — a process called vestibular compensation.
Causes — Why Does It Happen?
The honest answer is that we’re still not completely certain what triggers vestibular neuritis in every case. But the evidence points strongly in one direction.
Viral infection — the leading hypothesis
The most widely accepted cause is reactivation of herpes simplex virus type 1 (HSV-1) in the vestibular ganglion (Scarpa’s ganglion). This is the same virus that causes cold sores, and like all herpes viruses it stays dormant in nerve tissue for life after the initial infection.
Supporting this theory — Schuknecht and Kitamura found inflammatory changes consistent with viral neuritis in temporal bone histopathology studies. Arbusow and colleagues isolated HSV-1 DNA from vestibular ganglia in a significant proportion of specimens. Animal studies have demonstrated that HSV-1 inoculation can produce vestibular neuritis-like syndromes.
Why it reactivates when it does — stress, immune suppression, intercurrent illness — isn’t entirely clear. Many patients report a flu-like illness one to two weeks before the vertigo attack, which fits with viral reactivation triggered by systemic immune stress.
Vascular causes
Some cases may result from ischaemia of the vestibular nerve or its blood supply. The anterior vestibular artery, which supplies the superior vestibular nerve, is an end-artery with limited collateral circulation. In older patients particularly, vascular compromise is a plausible mechanism.
What this means clinically
The viral hypothesis explains why antiviral medication (with corticosteroids) has been studied as treatment. It also explains why vestibular neuritis can recur — reactivation of the latent virus can happen more than once, though recurrence rates are relatively low, somewhere around 10-15% over several years.
Symptoms — What Patients Experience
The acute attack
Vestibular neuritis typically begins suddenly — often upon waking, or with a specific head movement. The main symptom is severe, persistent rotatory vertigo. Not the brief spinning of BPPV that lasts seconds, not the episodic vertigo of Menière’s — but continuous, relentless spinning that can last hours to days.
Accompanying this are:
- Nausea and vomiting — often severe, especially in the first 24–48 hours
- Imbalance — patients lean or fall toward the affected side
- Oscillopsia — the visual world appears to jump or oscillate during head movement
- Nystagmus — involuntary eye movements, which a trained examiner can see and which confirm the vestibular origin
Crucially, there is no hearing loss in vestibular neuritis. This is an important distinction from labyrinthitis. If hearing is affected, the diagnosis changes.
There is also no ear pain, no tinnitus, no neurological symptoms like facial weakness, double vision, difficulty swallowing, or limb weakness.
The sub-acute phase (days 3 to 14)
Continuous vertigo gradually settles over the first week. What remains is a more persistent imbalance and the feeling that movement provokes dizziness — walking down a corridor, turning the head quickly, looking at busy visual environments like a supermarket.
Patients often describe this as feeling “off,” “foggy,” or like they’re on a boat. It’s not the violent spinning of the acute phase, but it’s disabling in its own way.
The compensation phase (weeks to months)
The brain begins adapting to the permanent asymmetry between the two vestibular inputs. Symptoms gradually improve, though the timeline varies considerably between individuals.
How Vestibular Neuritis Differs From Labyrinthitis
This is a question I get from patients and colleagues alike. The distinction is actually straightforward.
Vestibular neuritis: Inflammation confined to the vestibular nerve. No hearing loss.
Labyrinthitis: Inflammation that also involves the cochlea (the hearing organ). Hearing loss is present, often with tinnitus, alongside the vestibular symptoms.
The vestibular symptoms — vertigo, imbalance, nausea — are essentially identical between the two conditions. It’s the hearing that separates them.
Why does it matter clinically? Because labyrinthitis affecting hearing may require different management considerations, and because hearing loss during a vestibular episode can also point toward other diagnoses — Menière’s disease being the most important one to differentiate.
If a patient comes to me with vertigo and any degree of hearing loss, I do not diagnose vestibular neuritis without further evaluation.
Diagnosis — How We Confirm It
Vestibular neuritis is a clinical diagnosis — there is no single definitive blood test or scan that says “this is it.” Diagnosis is based on the history, the pattern of symptoms, and clinical examination findings. Investigations serve mainly to exclude other diagnoses.
Clinical examination
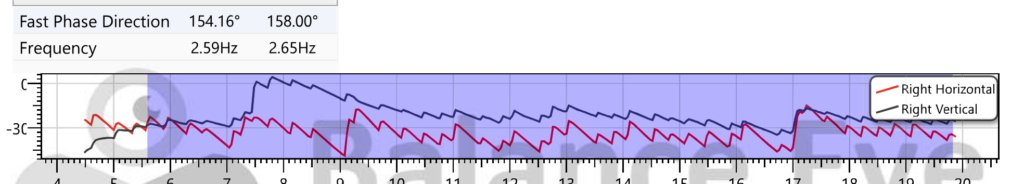
Vestibular Neuritis patient showing Right and Up beating Spontaneous Nystagmus
The most important finding on examination is spontaneous nystagmus — horizontal or horizontal-torsional nystagmus beating away from the affected side. This is present in the acute phase and typically suppressed by visual fixation (looking at a fixed target reduces it). As seen in this image above the spontaneous nystagmus is Right and Up beating which points towards superior vestibular neuritis.
The Head Impulse Test (HIT) is perhaps the most useful single bedside test. The examiner turns the patient’s head rapidly toward the affected side. In vestibular neuritis, the vestibulo-ocular reflex is impaired — the eyes don’t stay fixed on the target and a corrective saccade (catch-up eye movement) is visible. A positive HIT toward one side strongly suggests peripheral vestibular hypofunction on that side.
The HINTS examination — Head Impulse, Nystagmus, Test of Skew — is used particularly in emergency settings to differentiate peripheral vestibular disorders from central causes (stroke). In vestibular neuritis: HIT is positive (abnormal), nystagmus is unidirectional and horizontal, and there is no skew deviation. A negative HIT (normal) in the context of acute vertigo should raise concern for central pathology.
Videonystagmography (VNG)
In my practice, VNG is the standard test for objectively documenting vestibular hypofunction. Caloric testing as part of VNG measures the response of each vestibular labyrinth separately. In vestibular neuritis, the caloric response on the affected side is reduced (canal paresis). This confirms the diagnosis and gives a baseline for tracking recovery.
VNG also documents the nystagmus characteristics, documents gaze stability, and helps guide vestibular rehabilitation.
Imaging
MRI of the brain with gadolinium contrast is performed when there is any clinical concern for central pathology — atypical nystagmus, neurological symptoms, normal HIT in an acute vertiginous patient, severe headache, or any other red flag. In straightforward vestibular neuritis, MRI is normal (or may show enhancement of the vestibular nerve on high-resolution sequences, though this is not always present).
CT scan is generally not useful for vestibular neuritis — it doesn’t show the soft tissue structures of the inner ear well. I see many patients who’ve had CT scans before reaching me, and the result is almost invariably normal. Which is fine as an exclusion of hemorrhage, but it doesn’t help diagnose the problem.
Audiometry
Pure tone audiometry is performed to formally assess hearing. This confirms whether hearing is affected (labyrinthitis) or not (vestibular neuritis), and provides a baseline.
Treatment — Acute Phase and Long-Term
Treatment of vestibular neuritis has two phases with quite different goals.
Acute Phase Treatment (First 3–5 Days)
The priority in the first few days is symptom control. Vestibular neuritis in its acute phase is miserable — severe vertigo, continuous nausea, vomiting. The patient cannot function.
Vestibular suppressants
Medications that reduce the acute vestibular mismatch signal:
- Diazepam (2.5–) — very effective for the severe acute phase. Reduces nausea and the intensity of vertigo. Should be used for the shortest time necessary — typically 2–3 days maximum.
- Prochlorperazine or ondansetron — for nausea and vomiting control.
- Cinnarizine — a vestibular suppressant commonly used in India, reasonable for mild-moderate acute symptoms.
I want to be clear about something here — these medications are for the acute phase only. Continuing vestibular suppressants beyond the first few days actively delays recovery. The brain compensates by detecting and adapting to the vestibular asymmetry. Vestibular suppressants blunt this signal. I’ve seen patients on cinnarizine for months, still symptomatic, and their recovery began once we stopped the medication and started rehabilitation.
Corticosteroids
The evidence for corticosteroids in vestibular neuritis is mixed but leans toward benefit — particularly for improving the degree of vestibular function recovery. Strupp et al. (2004) showed that methylprednisolone significantly improved caloric recovery compared to placebo. Most vestibular specialists, including myself, use a course of oral Prednisolone (as prescribed by your doctor) — when there are no contraindications.
Antivirals
Despite the viral hypothesis, aciclovir or valaciclovir alone has not demonstrated benefit in controlled trials. The combination of antiviral plus steroid (as tested in the Strupp study) also didn’t outperform steroids alone for vestibular recovery. Based on current evidence, antivirals are not routinely recommended as standard of care for vestibular neuritis, though practice varies.
IV fluids and supportive care
For patients with severe vomiting who can’t keep anything down, IV fluids and IV antiemetics in the first day or two are appropriate. Most patients can be managed as outpatients once the vomiting is controlled.
Long-Term Treatment: Vestibular Rehabilitation
This is the most important part of treatment for most patients, and the part most often neglected.
Vestibular Rehabilitation
Vestibular rehabilitation therapy (VRT) works by exploiting the brain’s capacity for vestibular compensation and plasticity. The brain can learn to function with asymmetrical vestibular input — but only if it’s given the right challenges.
The core principles:
Gaze stabilization exercises: The patient moves their head while keeping their eyes fixed on a target. This trains the vestibulo-ocular reflex to become accurate despite the impaired input, by forcing the brain to develop compensatory strategies using visual and neck proprioceptive inputs.
Balance training: Progressive challenges to balance — firm surface with eyes open, firm surface with eyes closed, foam surface with eyes open, foam surface with eyes closed. Each step increases the demand on vestibular input and trains the brain to use it more efficiently.
Habituation exercises: Repeated exposure to movements that provoke dizziness gradually reduces the brain’s sensitivity to them. The key word is gradual — pushing too hard causes distress; too gentle causes no adaptation.
Walking and functional activity: Simply walking — on different surfaces, at different speeds, in different environments — is one of the most important rehabilitation activities. The vestibular inputs from walking help drive compensation.
Formal vestibular rehabilitation, prescribed and supervised by a specialist, substantially outperforms general advice and home exercise alone. The VNG findings guide which specific exercises are most beneficial for each patient.
I typically start vestibular rehabilitation during the first or second week after onset — not during the first 2–3 days when symptoms are most severe, but as soon as the patient can tolerate gentle movement without vomiting.
Recovery Timeline — What to Realistically Expect
Days 1–3: Acute phase. Severe vertigo, nausea, vomiting. Bed rest is appropriate but not prolonged. Vestibular suppressants and antiemetics.
Days 4–14: Acute symptoms settling. Persistent imbalance and movement-provoked dizziness. Start vestibular rehabilitation. Many patients can manage light activity, though driving is not appropriate yet.
Weeks 2–6: Progressive improvement with rehabilitation. Balance on stable surfaces improves substantially. Most patients return to desk work in this period. Dizziness increasingly becomes triggered only by specific provocations — busy visual environments, rapid head turns, uneven ground.
Weeks 6–12: Most patients reach 70–85% of pre-illness functional level. Moderate physical activity is possible. Driving can typically be resumed (with clinical assessment) once balance and visual stability are adequate.
Months 3–6: Residual symptoms in challenging conditions continue improving. Many patients achieve complete symptom resolution during this phase.
Beyond 6 months: A minority of patients — particularly older adults, those with poor initial vestibular function, and those who had inadequate rehabilitation — have persisting balance difficulties. This is not a failure of treatment; it’s an indication for more intensive assessment and ongoing rehabilitation.
The single biggest predictor of poor recovery in my experience is prolonged use of vestibular suppressants combined with physical inactivity in the weeks following the acute phase. These two things together essentially prevent the brain from compensating. I’ve seen patients who are still significantly symptomatic at 3 months, started proper VRT, and recovered substantially within 6–8 more weeks. It is almost never too late to start rehabilitation.
When Symptoms Don’t Go Away — PPPD
Some patients with vestibular neuritis develop a secondary condition called Persistent Postural-Perceptual Dizziness (PPPD). This is chronic dizziness — typically described as a rocking, swaying, or floating sensation rather than true spinning — that persists after the acute vestibular event has resolved.
PPPD develops when the brain gets stuck in a heightened state of vestibular monitoring. Anxiety about dizziness, avoidance of movement, and maladaptive visual dependence all contribute. It is a recognised neuro-otological condition, not “just anxiety,” though anxiety and PPPD are closely intertwined.
Treatment of PPPD combines vestibular rehabilitation with cognitive behavioural approaches, and sometimes SSRIs (sertraline or venlafaxine have the best evidence).
If you’ve been told your vestibular neuritis has “resolved” but you’re still significantly symptomatic at 3 months or beyond — please seek reassessment. You may have PPPD, or you may have incomplete vestibular compensation, or occasionally an alternative diagnosis may need to be reconsidered. But there is almost always something we can do.
Frequently Asked Questions
Q: Is vestibular neuritis the same as labyrinthitis?
No. Vestibular neuritis affects the vestibular nerve only — there is no hearing loss. Labyrinthitis also involves the cochlea and causes hearing loss alongside the vestibular symptoms. Both cause vertigo and imbalance, but the presence or absence of hearing loss is the key distinguishing feature.
Q: How long will I be off work?
For desk work or sedentary jobs — typically 2–4 weeks from onset. For physically demanding work, work requiring balance, or work at heights — 6–8 weeks minimum, with individual assessment. Driving should be discussed with your doctor specifically before resuming.
Q: Can vestibular neuritis come back?
Yes, but it’s relatively uncommon — recurrence happens in roughly 10–15% of patients over several years. When it does recur, it usually affects the same ear (same nerve) and is often less severe because the brain already has some compensation in place.
Q: Will I need surgery?
No. Vestibular neuritis does not require surgery. Treatment is medical — corticosteroids in the acute phase — and rehabilitative, through vestibular rehabilitation therapy.
Q: My balance still isn’t right after 4 months. Is this permanent?
Not necessarily. Incomplete compensation at 4 months warrants reassessment — to document your current vestibular function with VNG, to review your rehabilitation programme, and to check whether PPPD has developed. In many cases, intensified and properly targeted rehabilitation significantly improves symptoms even months after the initial episode.
Q: Can I exercise during recovery?
Yes — and you should. Movement drives vestibular compensation. From around day 4–7 onwards (once acute vomiting has settled), light walking and gentle vestibular rehabilitation exercises should begin. Avoid intense high-impact exercise in the first couple of weeks, but gentle to moderate activity is actively beneficial.
Q: Is vestibular neuritis a sign of something more serious?
In the vast majority of cases, no. It is a self-limiting condition caused by viral inflammation of the vestibular nerve. However, because acute vestibular neuritis can occasionally mimic stroke — particularly cerebellar infarction — an experienced clinician should evaluate any acute severe vertigo episode to exclude central causes. This is not something to self-diagnose.
Conclusion
Vestibular neuritis is a real, physiological injury to the vestibular nerve. The vertigo is not imagined, the imbalance is not psychological, and the recovery is not simply a matter of “waiting it out.”
What I tell my patients is this — the brain has an extraordinary ability to compensate for vestibular damage, but it needs to be challenged to do so. The worst thing you can do is rest completely and take vestibular suppressants indefinitely. The best thing you can do is get accurate diagnosis early, take appropriate treatment in the acute phase, and commit to proper vestibular rehabilitation.
Most patients with vestibular neuritis recover substantially. Many recover completely. And even those with persisting symptoms can improve significantly with the right approach.
If you’ve been struggling with dizziness and imbalance after an acute vertigo episode, don’t accept a non-answer. Get properly assessed by someone who understands vestibular disorders.
→ Related Articles:
About the Author
Dr. Prateek Porwal is an ENT & Vertigo Specialist with over 13 years of experience, holding MBBS (GSVM Medical College), DNB ENT (Tata Main Hospital), and CAMVD (Yenepoya University). He is the originator of the “Bangalore Maneuver” for Anterior Canal BPPV and has published research in Frontiers in Neurology and IJOHNS. Serving at Prime ENT Center, Hardoi — and available for Online Consultation.
Medical Disclaimer: This article is for informational and educational purposes only. It does not constitute medical advice. Diagnosis and treatment of vestibular disorders should be done by a qualified healthcare professional. If you are experiencing acute vertigo, please seek medical evaluation.
